Epidemiology
- Typical age of onset: bimodal distribution with one peak at 15–35 years and another one at 55–70 years
Tip
Compared with Ulcerative colitis, which peaks at 15-35 y/o.
- Populations with higher prevalence
- Individuals of Northern European descent
- Individuals of Ashkenazi Jewish descent
Etiology
- Risk factors
- Familial aggregation
- Genetic predisposition (e.g., mutation of the NOD2 gene, HLA-B27 association)
- Tobacco smoke
Tip
- Nicotine consumption is the only (known) controllable risk factor for CD. Therefore, smoking cessation is especially important in patients with CD.
- While smoking is a protective factor in Ulcerative colitis
Pathophysiology
- An inappropriate immune response to gut microbiota in genetically susceptible individuals (e.g., NOD2 gene mutations).
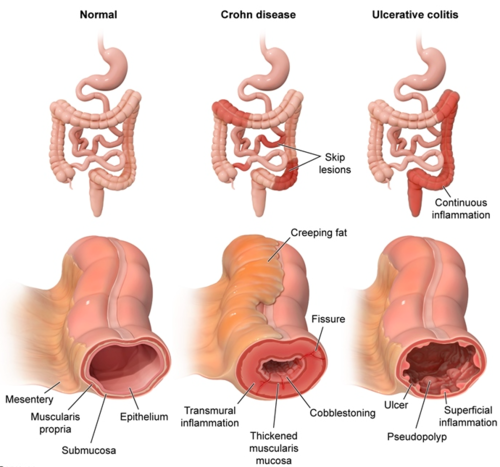
- Characterized by transmural inflammation, meaning it affects the entire thickness of the bowel wall. This can lead to fistulas and strictures.
- Can affect any part of the GI tract from mouth to anus, but most commonly involves the terminal ileum.
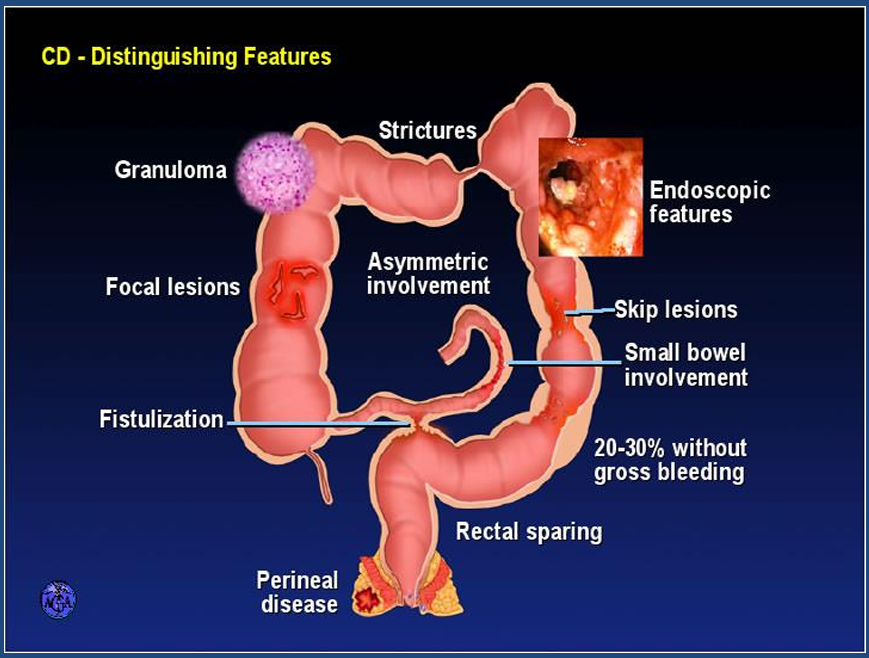
- Inflammation is discontinuous, resulting in “skip lesions”—areas of diseased bowel interspersed with healthy tissue.
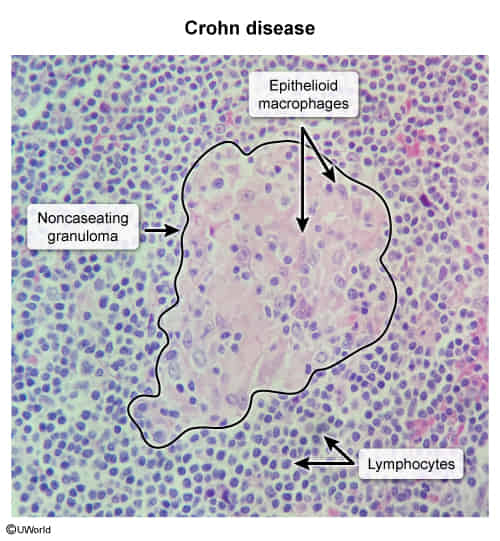
- Hallmark histologic finding is non-caseating granulomas.
Clinical features
- Common in young adults, presenting with intermittent, relapsing symptoms.
- Symptoms: Chronic, non-bloody diarrhea, RLQ abdominal pain, weight loss, and low-grade fever.
- Perianal disease, including skin tags, fissures, and fistulas, is common.
- GI Complications:
- Fistulas (e.g., enterocutaneous, enterovesical), strictures leading to bowel obstruction, and abscesses are common.
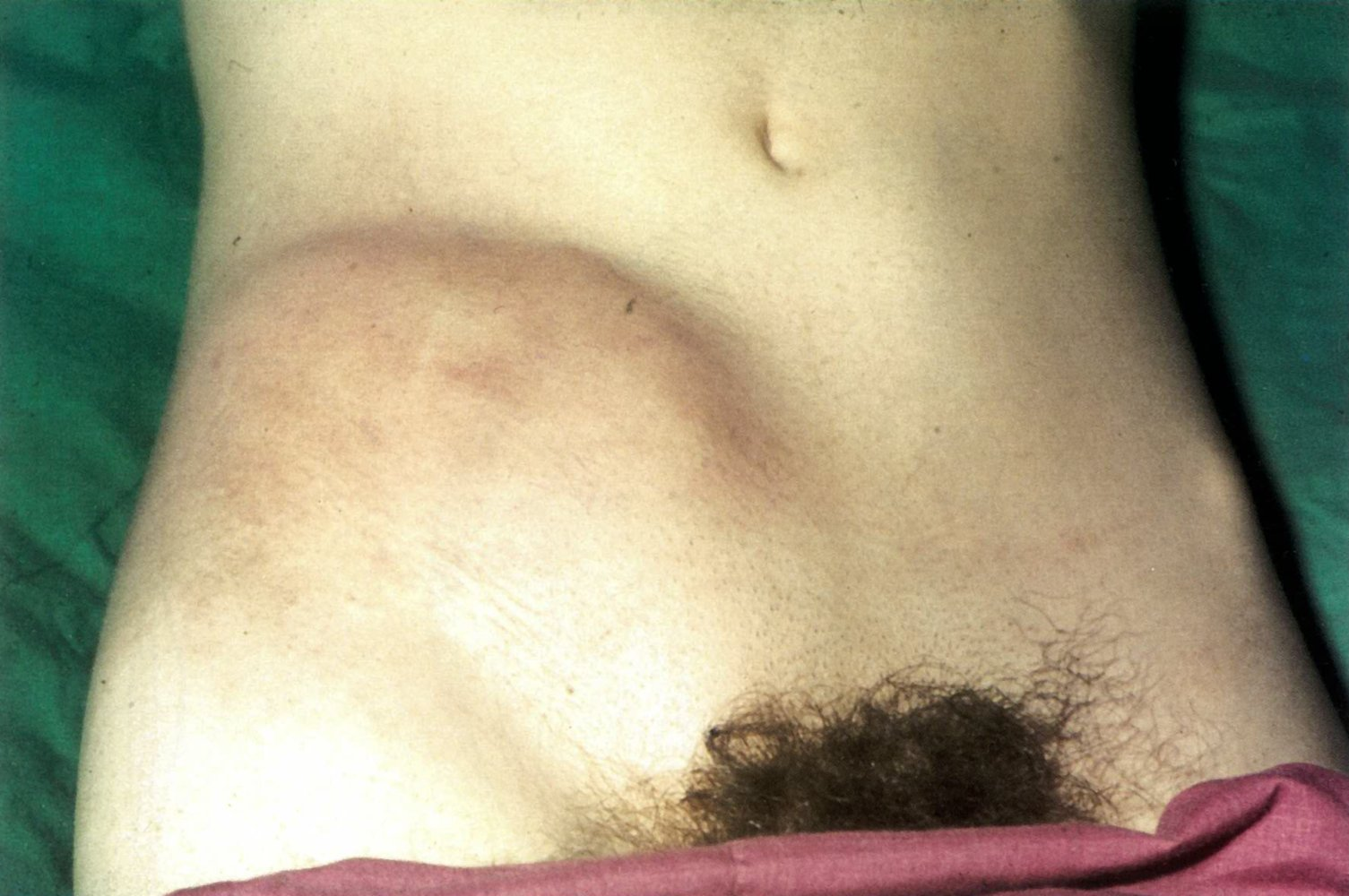
- Malabsorption can lead to deficiencies of Vitamin B12, iron, and fat-soluble vitamins.
- Since ulcerative colitis does not affect the small intestine, absorption of nutrients is not impaired. However, loss of appetite, poor tolerance of or avoidance of certain foods, and adjustment of diet without medical consultation can lead to malnutrition already in nonsevere disease.
- Fistulas (e.g., enterocutaneous, enterovesical), strictures leading to bowel obstruction, and abscesses are common.
- Extraintestinal Manifestations:
- Musculoskeletal: Arthritis (peripheral or axial, including ankylosing spondylitis). This is the most common extraintestinal complication.
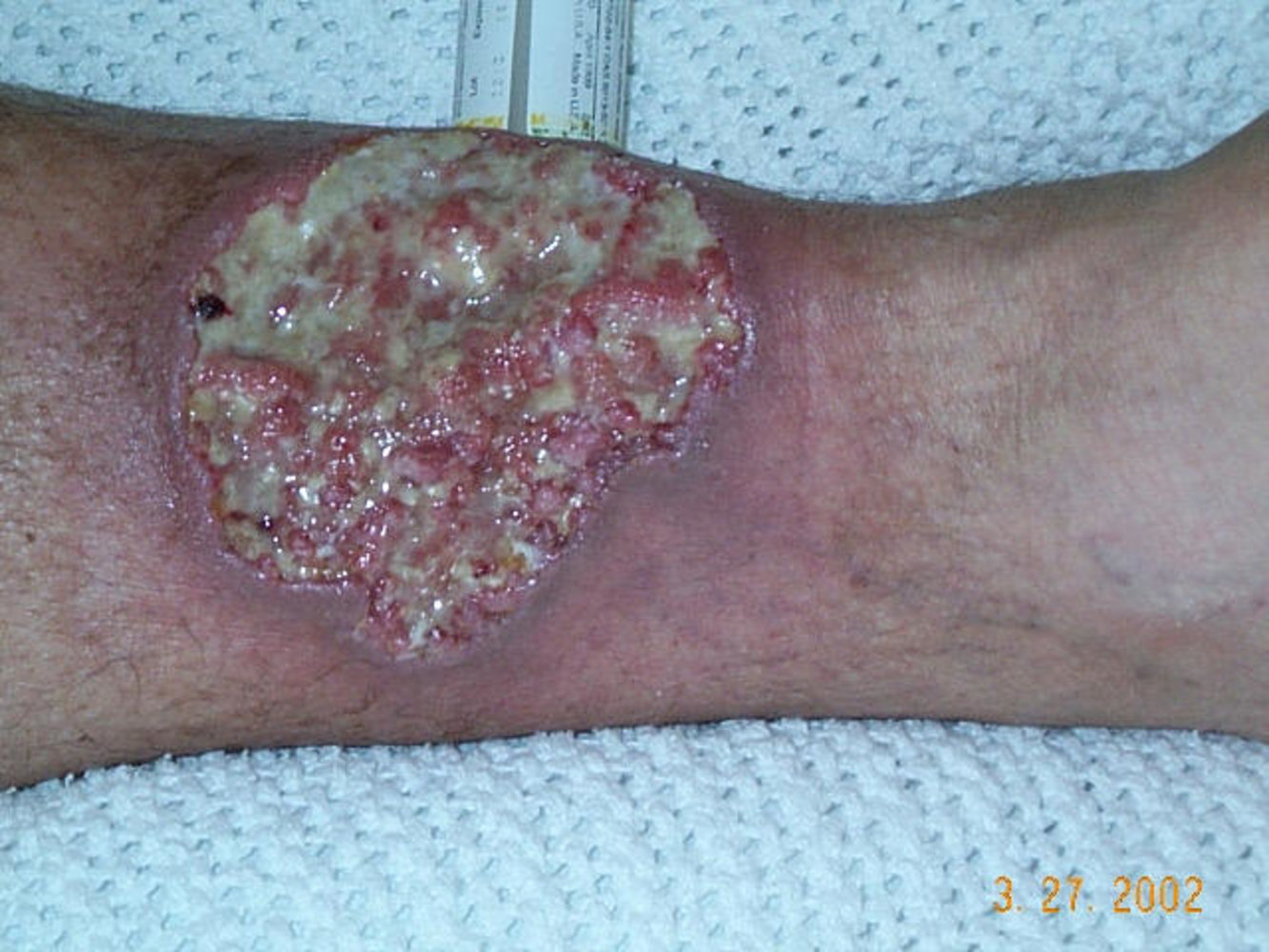
- Skin: Erythema nodosum (painful red nodules on shins) and pyoderma gangrenosum (deep, ulcerative lesions).
- Ocular: Uveitis, episcleritis, and conjunctivitis.
- Other: Aphthous ulcers (mouth sores), gallstones, and calcium oxalate kidney stones due to fat malabsorption.
Tip
Anemia in CD may result from chronic disease, iron deficiency, and/or vitamin B12 deficiency.
Diagnostics
Endoscopy
- Indication: all patients with suspected CD
- Assesses the distribution and severity of the disease
- Aids differentiation of CD from other diseases (e.g., ulcerative colitis)
- Monitors disease activity (e.g., active disease, remission)
- Can be used therapeutically (e.g., stricture dilatation)
- Supportive findings
- Skip lesions: segmental and/or discontinuous pattern of involvement (interspersed with normal tissue)
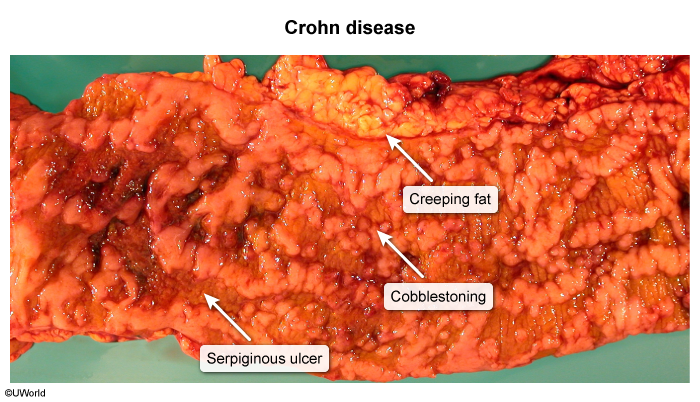
- Linear and/or serpiginous ulcerations
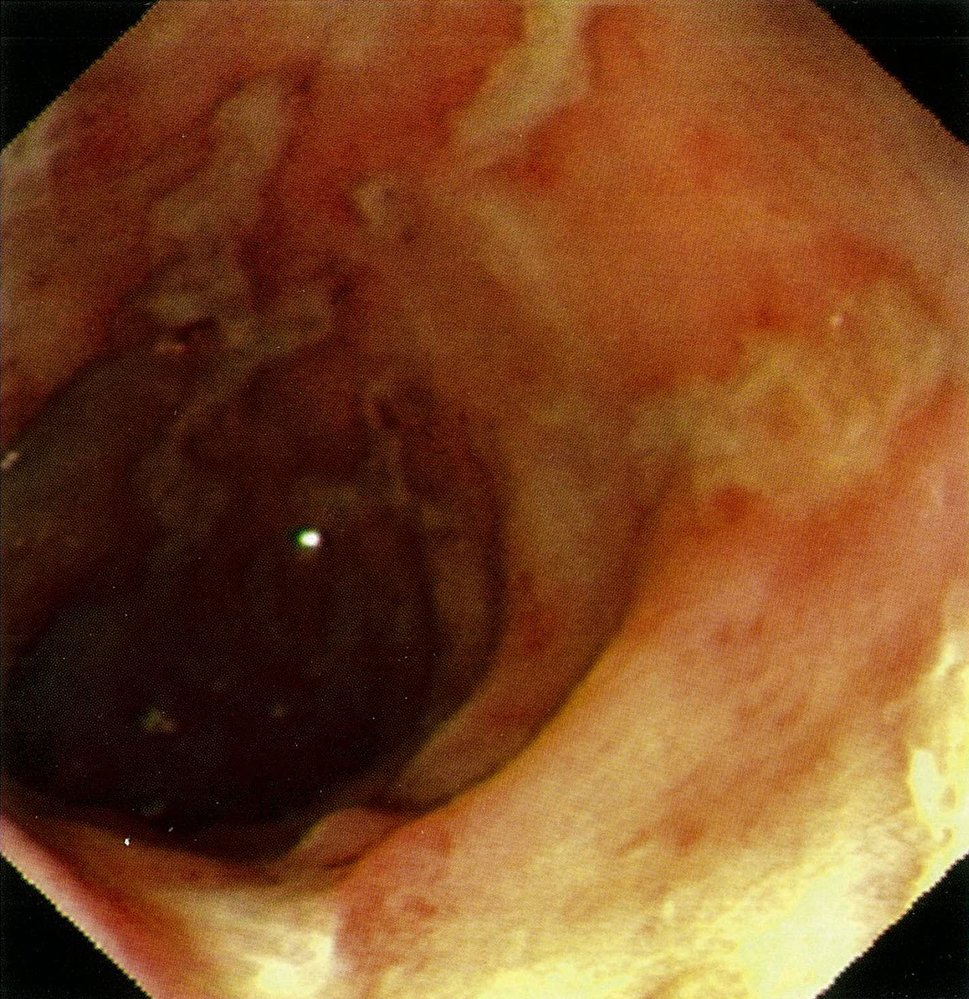
- Small aphthous ulcerations
- Cobblestone sign: inflamed edematous sections interspersed with deep ulcerations that resemble cobblestones
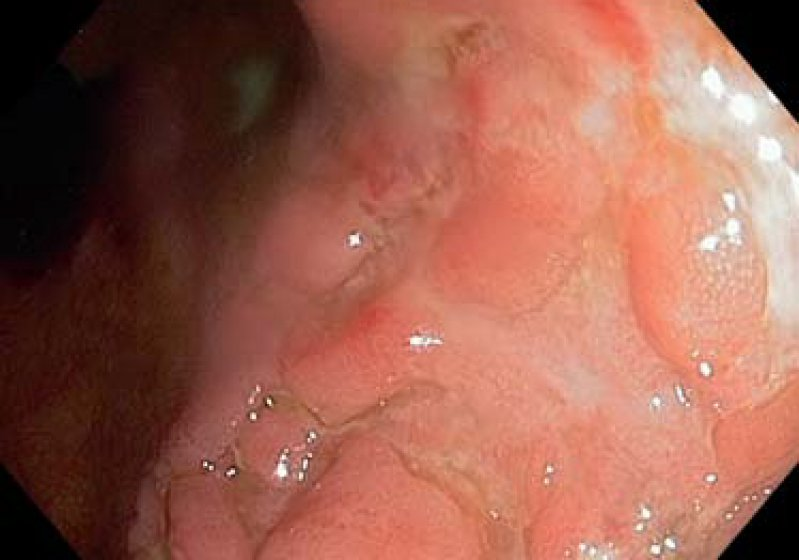
- Erythema, fissures, strictures, and fistulas
Imaging
- Cross-sectional enterography (MRE, CTE): preferred imaging modality for CD
- Edematous thickening of the intestinal wall
- Creeping fat: excessive mesenteric fat around the affected segments of bowel
- Possibly in response to intestinal bacteria translocation
Laboratory studies
- To monitor disease activity
- Fecal calprotectin and/or fecal lactoferrin: proteins associated with neutrophil activation
- Used as noninvasive markers of intestinal inflammation to monitor disease activity and response to therapy
- Also used to differentiate IBD from irritable bowel syndrome
- Inflammatory markers: CRP, ESR
- Fecal calprotectin and/or fecal lactoferrin: proteins associated with neutrophil activation
Treatment
Treatment
Ulcerative Colitis (UC) Treatment
Feature Ulcerative Colitis (UC) Crohn Disease (CD) Surgery Curative (Proctocolectomy) Non-Curative (Recurrence common) Surgical Goal Remove colon (cancer/Sx risk) Bowel-sparing (Strictureplasty) Mild Induction 5-ASAs (Mesalamine) Budesonide (ileitis) or Antibiotics (perianal) Maintenance 5-ASAs, Anti-TNF, Tofacitinib Azathioprine, Methotrexate, Anti-TNF Acute Flare Systemic Steroids Systemic Steroids Complications Toxic Megacolon Fistulas, Strictures, Abscesses
- Goal: Induce and maintain remission; surgery (proctocolectomy) is curative.
- Mild: 5-ASAs (Mesalamine, Sulfasalazine). Use topical formulations for distal disease.
- Acute Flare: Corticosteroids (Prednisone) to induce remission.
- Severe/Maintenance: Biologics (Infliximab, Vedolizumab) or Thiopurines (Azathioprine).
- Surgery: Curative. Total proctocolectomy with J-pouch.
- Indications: Toxic megacolon, perforation, carcinoma, refractory disease.
Crohn Disease (CD) Treatment
- Goal: Induce and maintain remission; surgery is not curative and reserved for complications.
- Mild-to-Moderate Disease:
- Induction: Corticosteroids are first-line for flares (Budesonide preferred for ileocecal disease to limit systemic effects).
- Maintenance: May not require therapy if remission is stable. Use Azathioprine/6-MP for recurrent disease.
- Moderate-to-Severe Disease:
- Induction: Biologics (e.g., Infliximab, Adalimumab) are often used early, with or without corticosteroids.
- Maintenance: Biologics and/or immunomodulators are the standard.
- Fistulizing Disease:
- Tx: Anti-TNF biologics (e.g., Infliximab) are the most effective treatment. t
Key Drug Classes
- 5-ASA (Mesalamine): Mainstay for mild-moderate UC. Less effective in CD.
- Corticosteroids (Prednisone, Budesonide): For acute flares only (induction). Not for maintenance.
- Immunomodulators (Azathioprine, Methotrexate): Steroid-sparing agents for maintenance in both UC & CD.
- Biologics (Anti-TNF, etc.): For moderate-to-severe or refractory disease in both UC & CD. Crucial for fistulizing Crohn’s.
Link to original
Complications
Fistulizing CD
- Occur in one-third of patients with CD
- Typically involve the perianal region
Other intestinal complications
- Colorectal cancer (especially in the case of pancolitis)
- Short bowel syndrome and associated issues after surgery
- Stenosis/strictures → bowel obstruction/(sub)ileus
- Occur as a result of bowel wall edema, fibrosis, and hypertrophy (thickening) of the muscularis mucosae, which narrows the intestinal lumen
- Intestinal perforation → peritonitis
- Primary sclerosing cholangitis
- Impaired bile acid reabsorption
- Cholesterol gallstones
.jpg)
- Bile acid diarrhea
- Bile acid malabsorption → steatorrhea and deficiencies in fat-soluble vitamins
- Cholesterol gallstones
- Abscess formation/phlegmons
Systemic complications
- Signs of malabsorption syndrome
- Weight loss
- Failure to thrive and growth failure in children
- Anemia
- Iron deficiency anemia
- Caused by intestinal blood loss
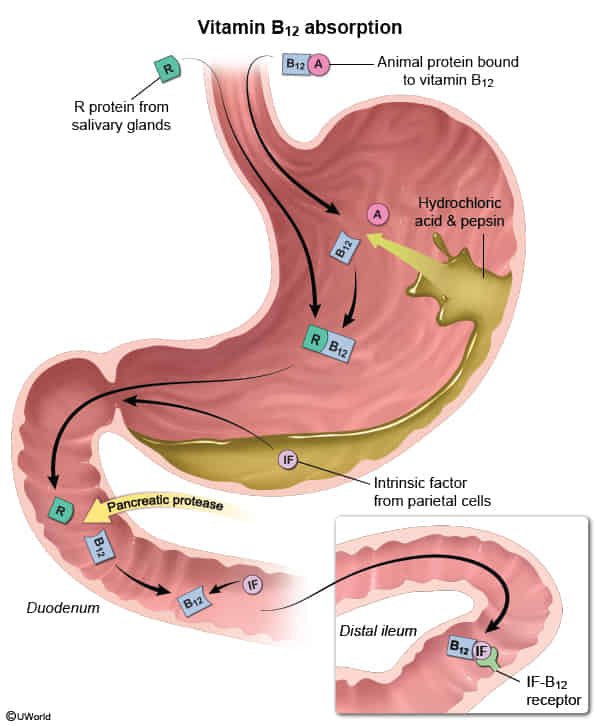
- Megaloblastic anemia (vitamin B12 deficiency due to impaired absorption in the chronically inflamed ileum)
- Iron deficiency anemia
- Osteoporosis