Epidemiology
- Higher in White populations than in Black, Hispanic, or Asian populations
- Highest among individuals of Ashkenazi Jewish descent
- 15–35 years of age
Tip
Compared with Crohn disease, which is bimodal distribution with one peak at 15–35 years and another one at 55–70 years
Etiology
- Genetic predisposition (e.g., HLA-B27 association)
- Ethnicity (White populations, individuals of Ashkenazi Jewish descent)
- Protective factors: smoking
- The pathophysiology is not fully understood, as smoking has negative effects on other inflammatory diseases (e.g., Crohn disease).
Pathophysiology
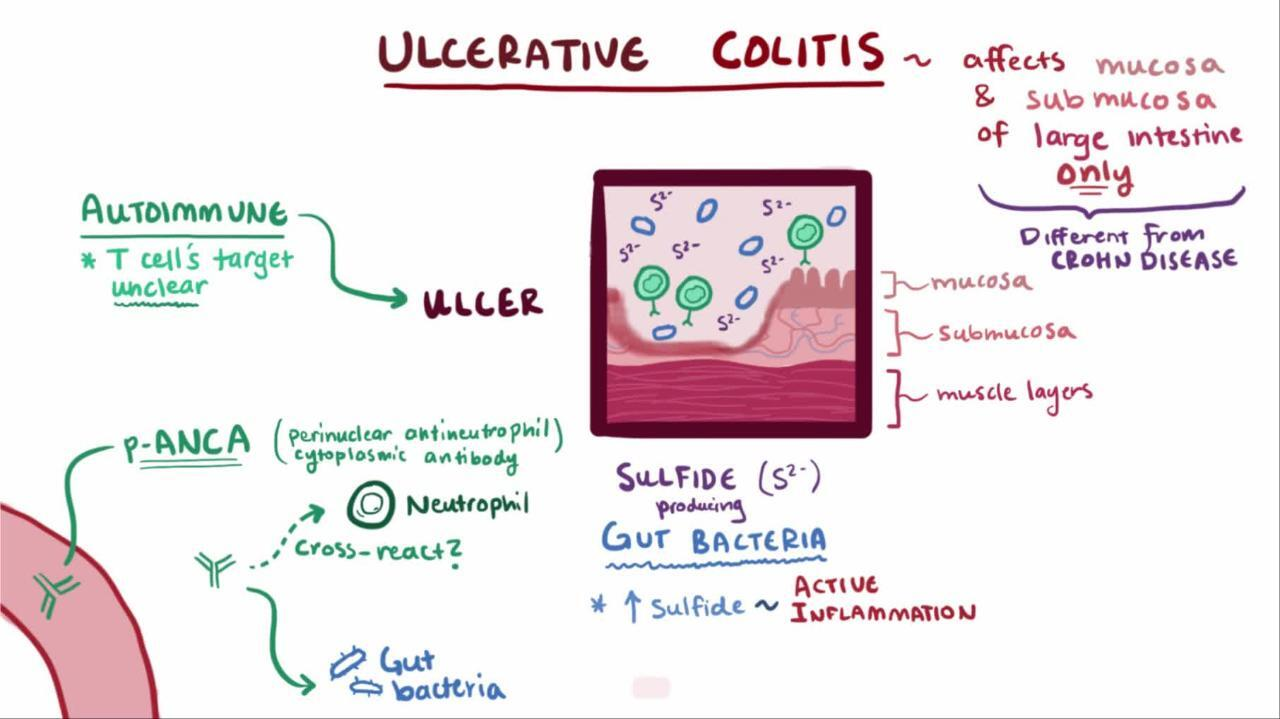
- Dysregulation of intestinal epithelium: increased permeability for luminal bacteria → activation of macrophages and dendritic cells → antigen presentation to macrophages and naive CD4+ cells
- Dysregulation of the immune system: upregulation of lymphatic cell activity (T cells, B cells, plasma cells) in bowel walls → enhanced immune reaction and cytotoxic effect on colonic epithelium → inflammation with local tissue damage (ulcerations, erosions, necrosis) in the submucosa and mucosa
- Autoantibodies (pANCA) against cells of the intestinal epithelium
- Pattern of involvement
- Ascending inflammation that begins in the rectum and spreads continuously proximally throughout the colon
- Inflammation is limited to the mucosa and submucosa.
Crohn disease is characterized by transmural inflammation.
Unlike ulcerative colitis,
Tip
The rectum is always involved in ulcerative colitis.
Clinical features
- Intestinal symptoms
- Bloody diarrhea with mucus
- Fecal urgency
- Abdominal pain and cramps
- Tenesmus
- Extraintestinal symptoms of ulcerative colitis
- General: fatigue, fever
- Skeletal (most common extraintestinal manifestation of ulcerative colitis): osteoarthritis, ankylosing spondylitis, sacroiliitis
- Ocular: uveitis, episcleritis, iritis
- Biliary: primary sclerosing cholangitis (it is rare for patients with ulcerative colitis to develop PSC, but up to 90% of all patients with PSC will also have ulcerative colitis)
- Cutaneous
- Erythema nodosum
- Pyoderma gangrenosum
- Aphthous stomatitis
Tip
Diagnostics
Ileocolonoscopy
Recommended method for diagnosis and disease monitoring
Early stages
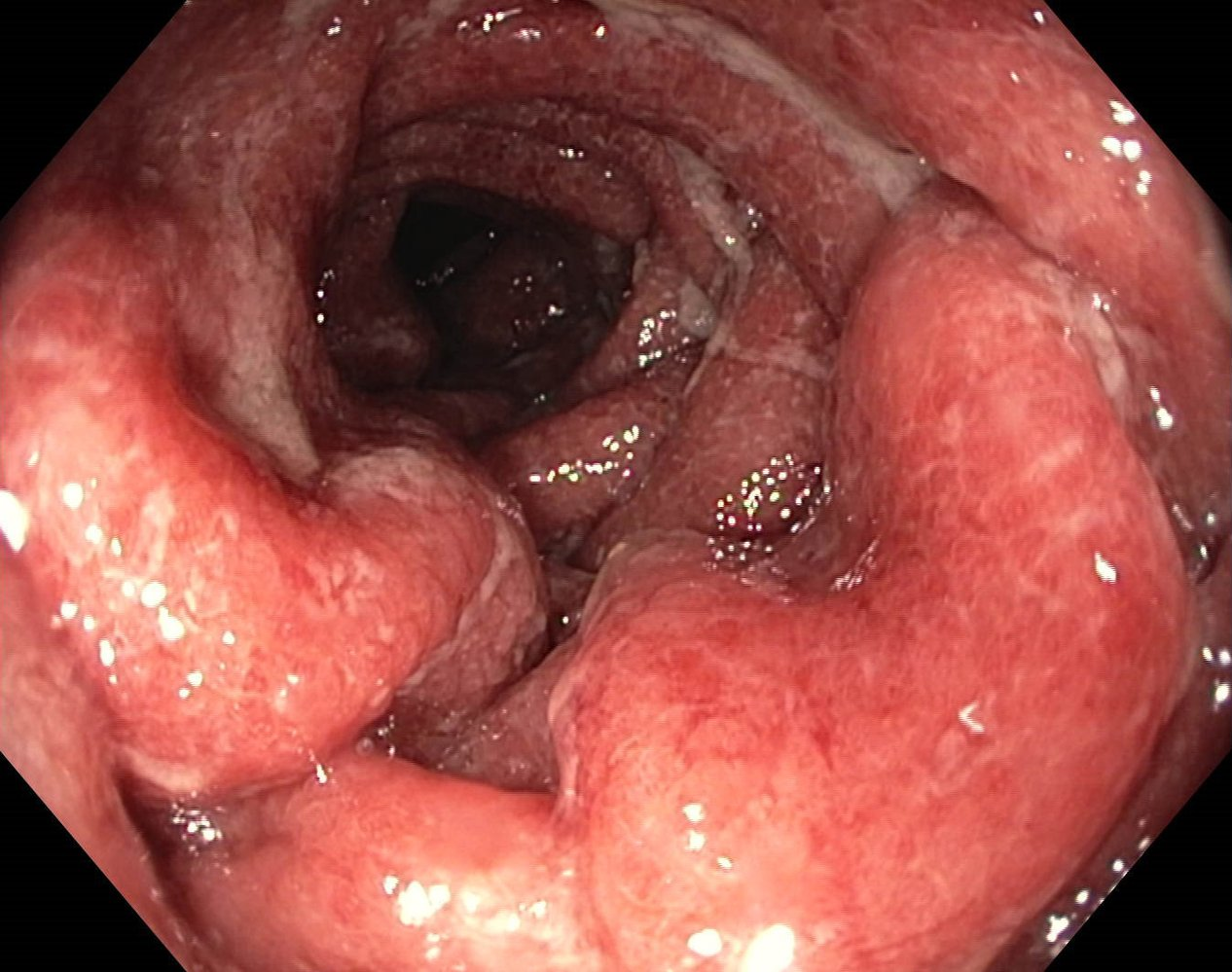
- Inflamed, erythematous, edematous mucosa

- Friable mucosa with bleeding on contact with endoscope
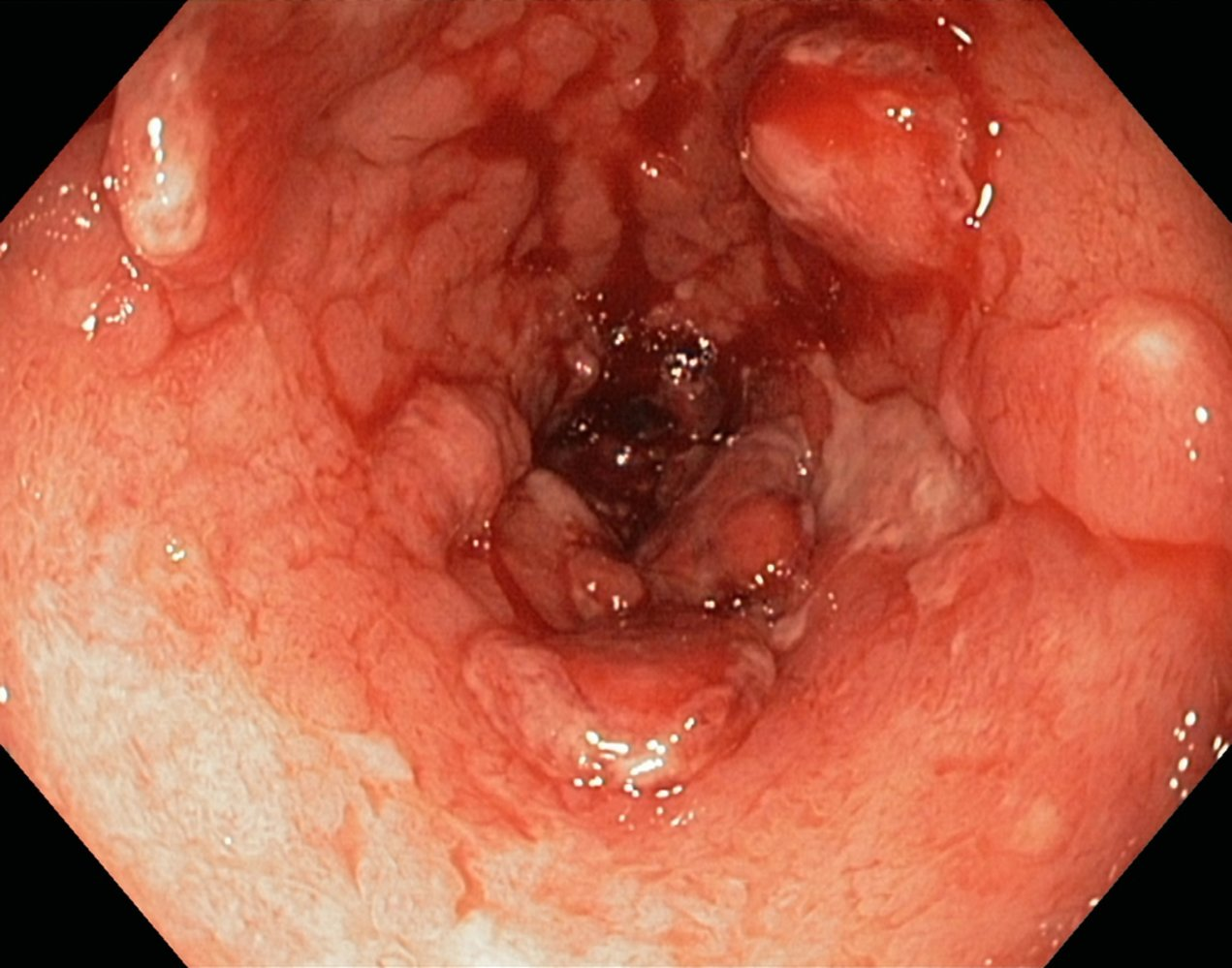 A fibrin-covered ulceration (blue overlay) and several pseudopolyps (indicated by dashed lines) are visible.
A fibrin-covered ulceration (blue overlay) and several pseudopolyps (indicated by dashed lines) are visible.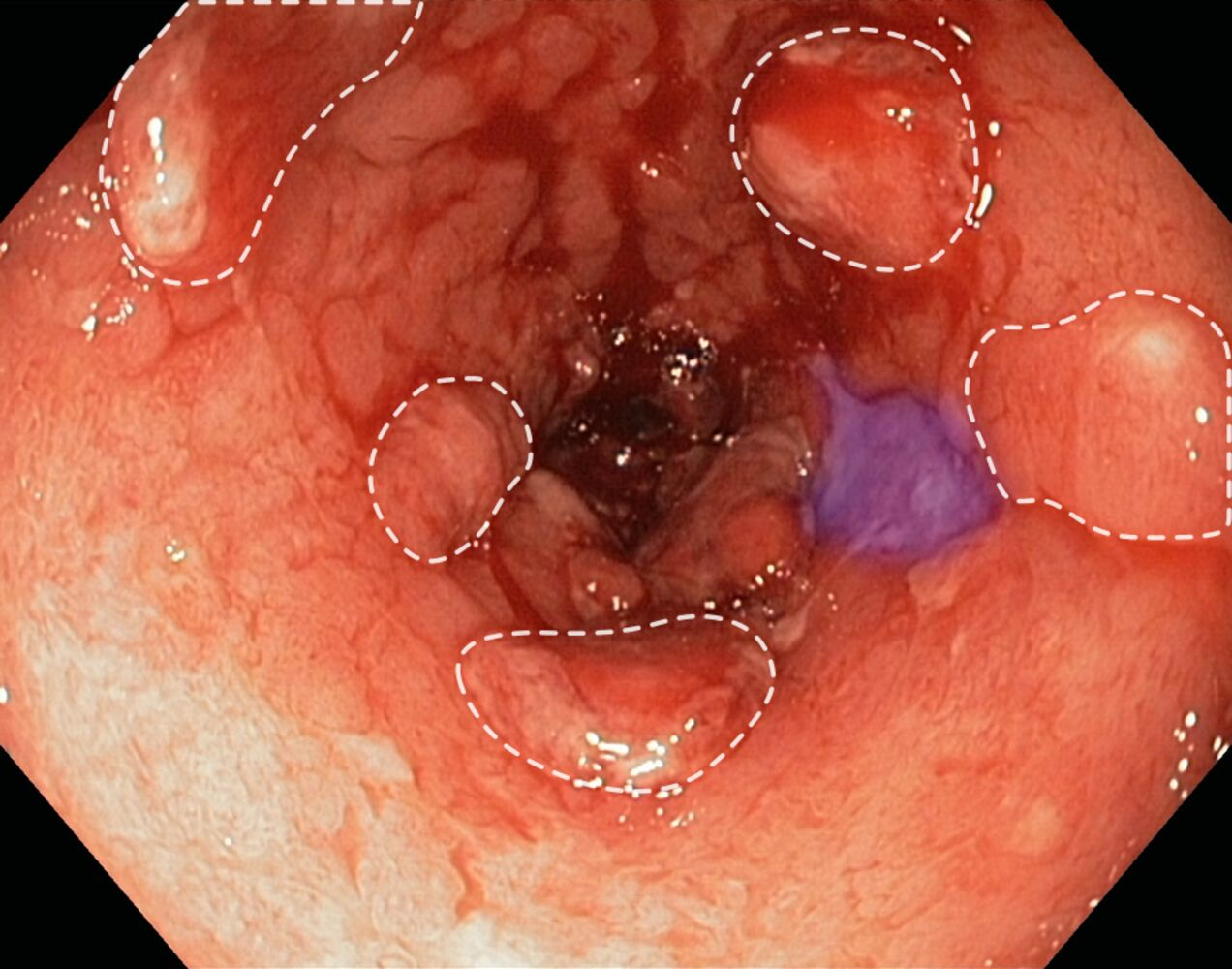
- Fibrin-covered ulcers
Chronic disease
- Loss of haustra
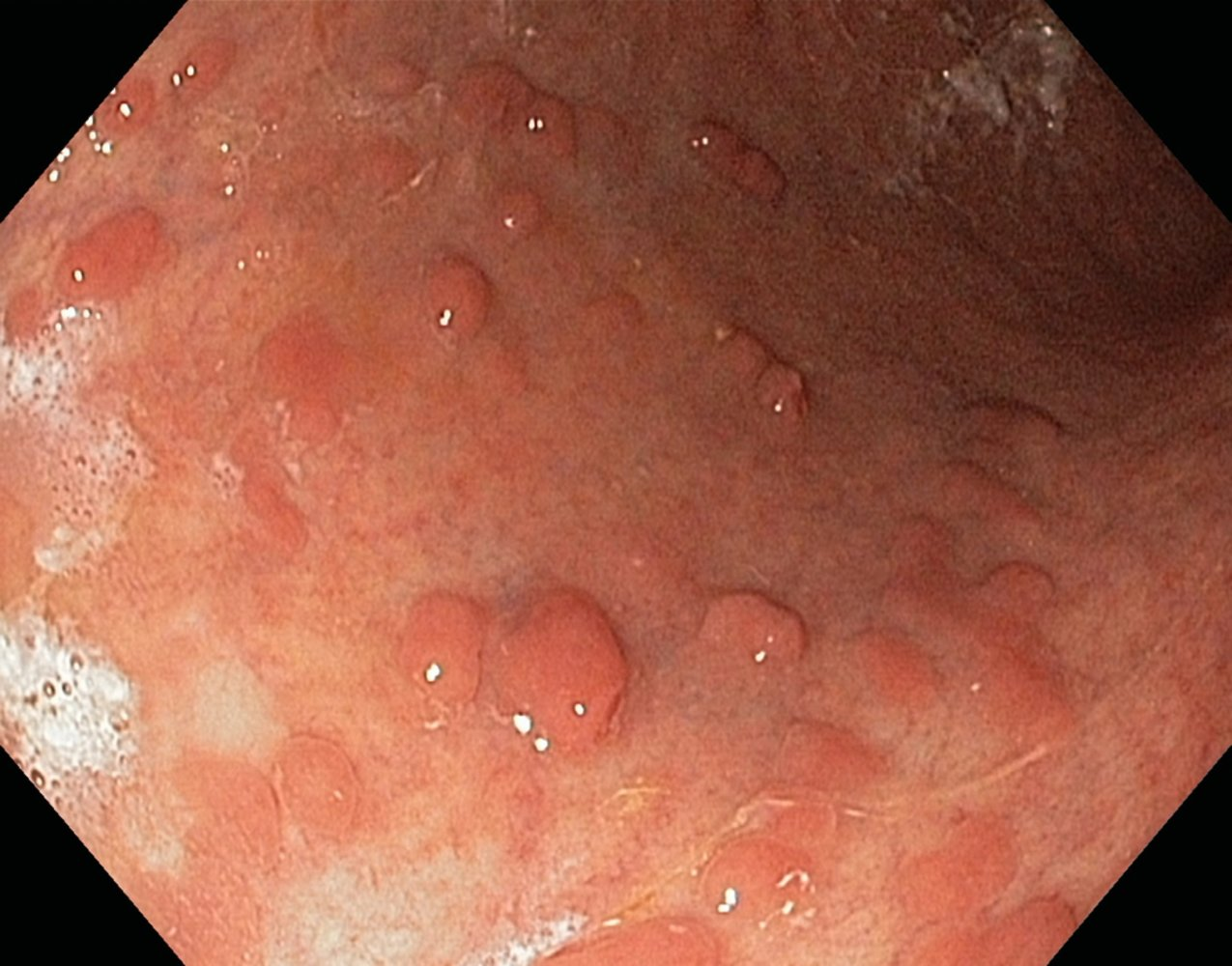
- Pseudopolyps
- Raised areas of normal mucosal tissue that result from repeated cycles of ulceration and healing
- Ulceration → formation of granulation tissue → deposition of granulation tissue → epithelialization
Imaging
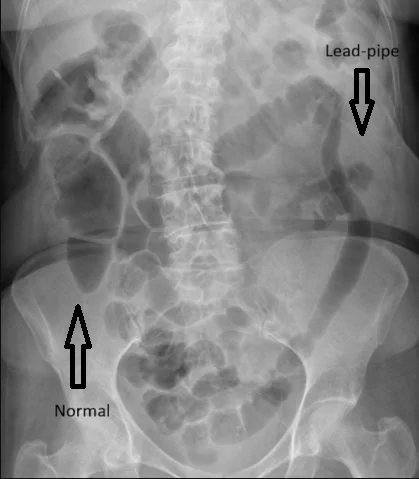
- Barium enema (less common now): Shows loss of haustra, resulting in a “lead pipe” appearance.
Treatment
Ulcerative Colitis (UC) Treatment
| Feature | Ulcerative Colitis (UC) | Crohn Disease (CD) |
|---|---|---|
| Surgery | Curative (Proctocolectomy) | Non-Curative (Recurrence common) |
| Surgical Goal | Remove colon (cancer/Sx risk) | Bowel-sparing (Strictureplasty) |
| Mild Induction | 5-ASAs (Mesalamine) | Budesonide (ileitis) or Antibiotics (perianal) |
| Maintenance | 5-ASAs, Anti-TNF, Tofacitinib | Azathioprine, Methotrexate, Anti-TNF |
| Acute Flare | Systemic Steroids | Systemic Steroids |
| Complications | Toxic Megacolon | Fistulas, Strictures, Abscesses |
- Goal: Induce and maintain remission; surgery (proctocolectomy) is curative.
- Mild: 5-ASAs (Mesalamine, Sulfasalazine). Use topical formulations for distal disease.
- Acute Flare: Corticosteroids (Prednisone) to induce remission.
- Severe/Maintenance: Biologics (Infliximab, Vedolizumab) or Thiopurines (Azathioprine).
- Surgery: Curative. Total proctocolectomy with J-pouch.
- Indications: Toxic megacolon, perforation, carcinoma, refractory disease.
Crohn Disease (CD) Treatment
- Goal: Induce and maintain remission; surgery is not curative and reserved for complications.
- Mild-to-Moderate Disease:
- Induction: Corticosteroids are first-line for flares (Budesonide preferred for ileocecal disease to limit systemic effects).
- Maintenance: May not require therapy if remission is stable. Use Azathioprine/6-MP for recurrent disease.
- Moderate-to-Severe Disease:
- Induction: Biologics (e.g., Infliximab, Adalimumab) are often used early, with or without corticosteroids.
- Maintenance: Biologics and/or immunomodulators are the standard.
- Fistulizing Disease:
- Tx: Anti-TNF biologics (e.g., Infliximab) are the most effective treatment. t
Key Drug Classes
- 5-ASA (Mesalamine): Mainstay for mild-moderate UC. Less effective in CD.
- Corticosteroids (Prednisone, Budesonide): For acute flares only (induction). Not for maintenance.
- Immunomodulators (Azathioprine, Methotrexate): Steroid-sparing agents for maintenance in both UC & CD.
- Biologics (Anti-TNF, etc.): For moderate-to-severe or refractory disease in both UC & CD. Crucial for fistulizing Crohn’s.
Complications
- ↑ Risk of cancer
- chronic inflammation → hyperplasia → non-polypoid dysplasia → neoplasia
- Toxic megacolon
- Fulminant colitis
- Gastrointestinal bleeding (both acute and chronic)
- Perforation