Purine Synthesis & Metabolism
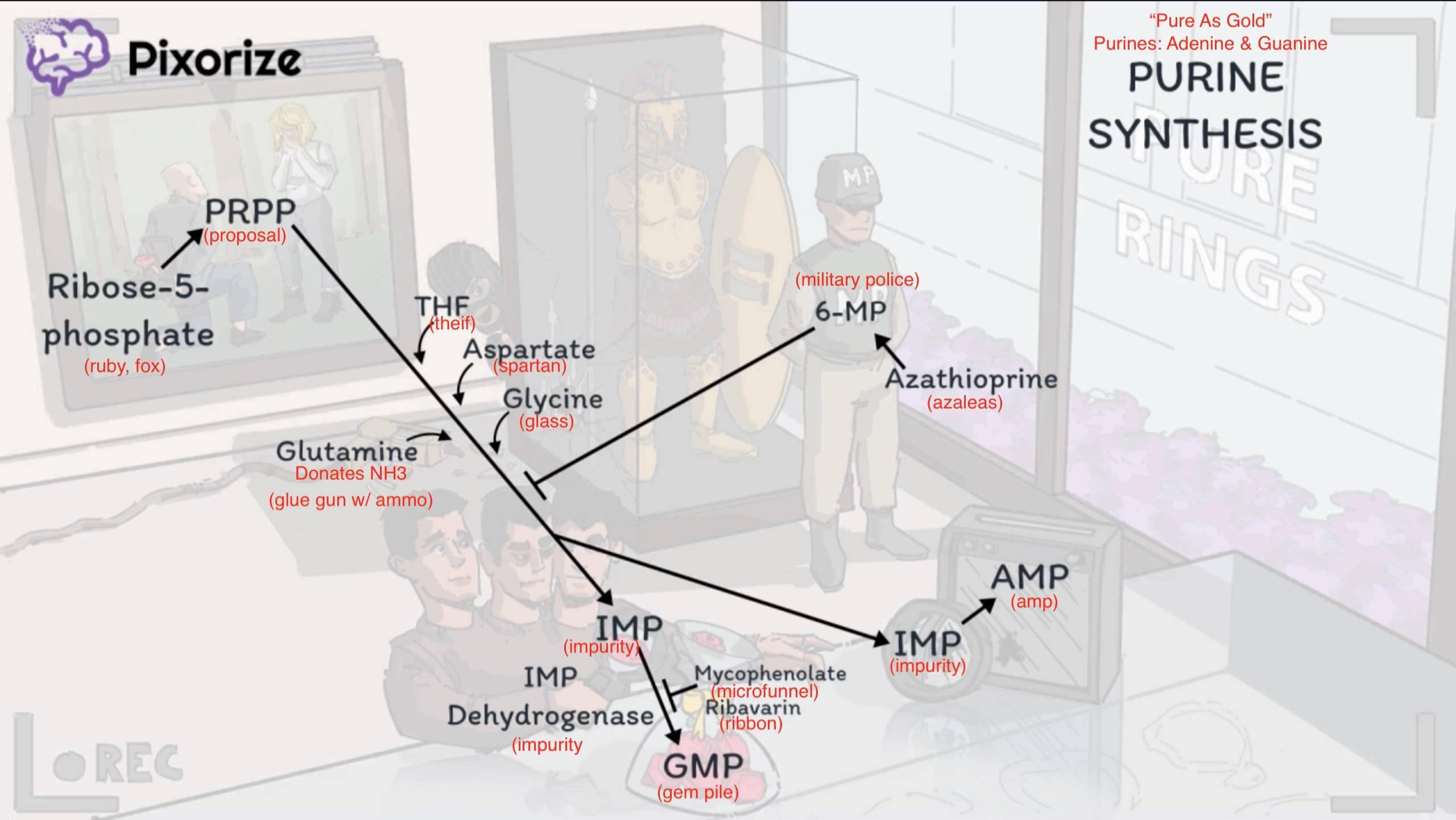
De Novo Purine Synthesis
- Goal: Synthesize purine nucleotides (AMP, GMP) from simple precursors.
- Precursors: Ribose-5-phosphate (from HMP shunt), Glycine, Aspartate, Glutamine, CO2, THF.
- Key Pathway Steps:
- Ribose-5-Phosphate → PRPP (5-phosphoribosyl-1-pyrophosphate) via PRPP synthetase.
- PRPP → IMP (Inosine monophosphate) via multiple steps. This is the first purine base formed.
- Rate-limiting enzyme: Glutamine-PRPP amidotransferase.
- IMP is a branch point and is converted to either:
- AMP (requires GTP for energy)
- GMP (requires ATP for energy, catalyzed by IMP Dehydrogenase)

Purine Salvage Pathway
- Goal: Recycle free purine bases to reform nucleotides, conserving energy.
- Key Enzymes:
- HGPRT (Hypoxanthine-guanine phosphoribosyltransferase):
- Converts Hypoxanthine → IMP.
- Converts Guanine → GMP.
- APRT (Adenine phosphoribosyltransferase):
- Converts Adenine → AMP.
- HGPRT (Hypoxanthine-guanine phosphoribosyltransferase):
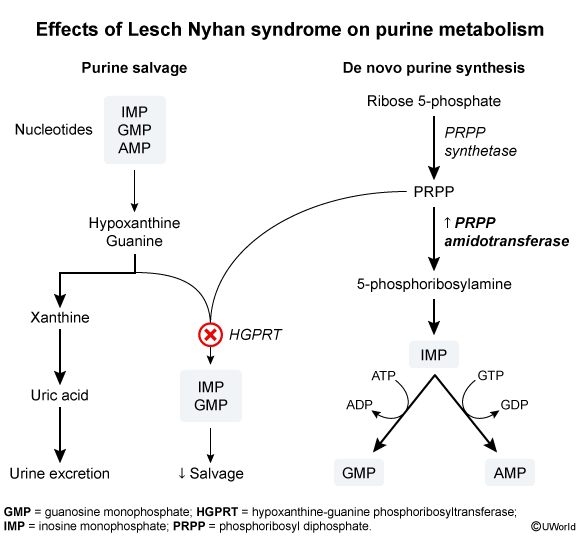
- Lesch-Nyhan Syndrome: X-linked recessive deficiency of HGPRT.
- Patho: Inability to salvage hypoxanthine and guanine leads to their degradation, causing excess uric acid production. Also leads to ↑ de novo purine synthesis due to ↑ PRPP levels.
- Presentation (HGPRT):
Purine Degradation
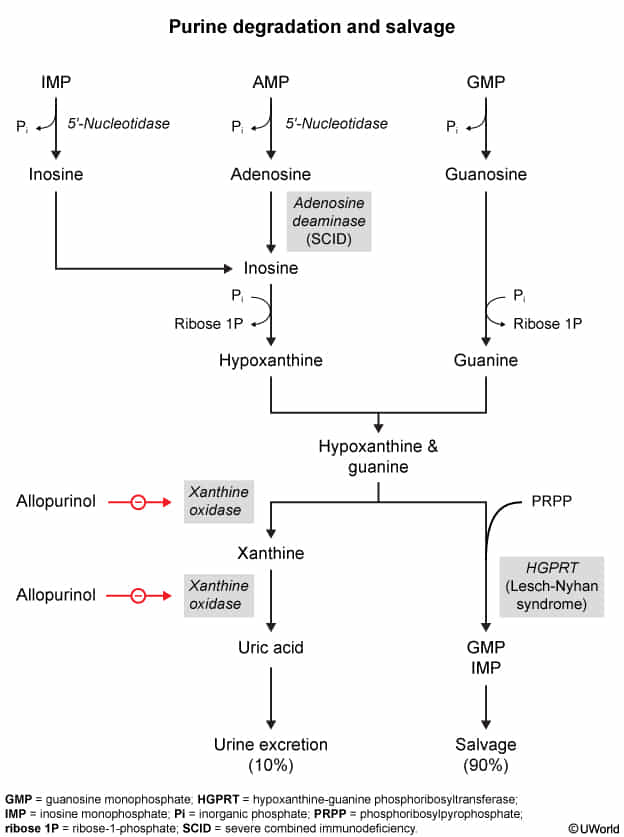
- Goal: Degrade purines into uric acid for excretion.
- Key Pathway Steps:
- AMP → Adenosine → Inosine (via Adenosine Deaminase - ADA).
- Inosine → Hypoxanthine.
- GMP → Guanine.
- Hypoxanthine → Xanthine (via Xanthine Oxidase).
- Guanine → Xanthine.
- Xanthine → Uric Acid (via Xanthine Oxidase).
- Clinical Correlation: Gout
- Patho: Hyperuricemia leading to monosodium urate crystal deposition in joints.
- Causes of Hyperuricemia: ↑ purine production (Lesch-Nyhan, tumor lysis syndrome), or ↓ uric acid excretion (renal failure, thiazide/loop diuretics).
- Tx:
- Acute: NSAIDs, Colchicine, Glucocorticoids.
- Chronic: Allopurinol, Febuxostat (inhibit Xanthine Oxidase).
High-Yield Pharmacology
- 6-Mercaptopurine (6-MP) and its prodrug Azathioprine: Inhibit de novo purine synthesis.
- Mycophenolate & Ribavirin: Inhibit IMP Dehydrogenase, blocking the conversion of IMP to GMP. Particularly affects lymphocytes.
- Allopurinol & Febuxostat: Inhibit Xanthine Oxidase, decreasing uric acid production. Used to treat chronic gout.
- Drug Interaction: When given with 6-MP/Azathioprine, allopurinol increases their toxicity (both are metabolized by xanthine oxidase). Dose of 6-MP/Azathioprine must be reduced.
Pyrimidine synthesis

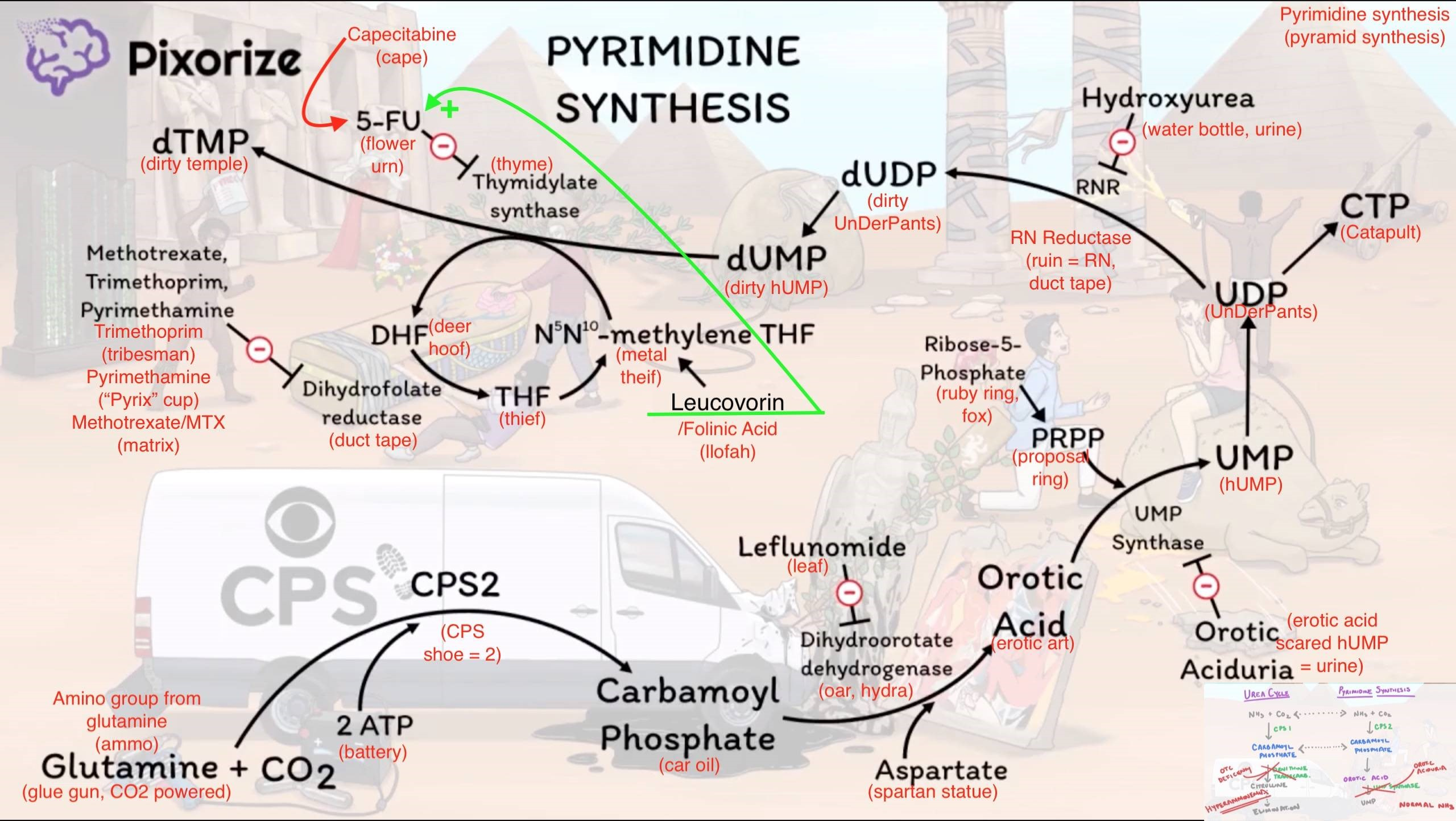
- Building Blocks: Glutamine + CO2 + Aspartate.
- Pyrimidine ring is made first, then attached to PRPP.
- Rate-Limiting Enzyme: Carbamoyl Phosphate Synthetase II (CPS II) in the cytosol. t
- Activated by: ATP, PRPP
- Inhibited by: UTP
- Key Conversions & Drug Targets:
- Leflunomide inhibits Dihydroorotate Dehydrogenase.
- Hydroxyurea inhibits Ribonucleotide Reductase (UDP → dUDP).
- 5-Fluorouracil (5-FU) inhibits Thymidylate Synthase (dUMP → dTMP).
- Methotrexate, Trimethoprim, Pyrimethamine inhibit Dihydrofolate Reductase (DHFR), blocking THF regeneration needed for thymidylate synthesis.
- High-Yield Disease: Orotic Aciduria
- Defect: UMP Synthase deficiency.
- Sx: Megaloblastic anemia (unresponsive to B12/folate), failure to thrive, ↑ orotic acid in urine.
- Key Differentiator: NO hyperammonemia (vs. Ornithine Transcarbamylase deficiency).
- Tx: Uridine supplementation.
Folate acid pathway
Folate Pathway: The Basics
Folate (Vitamin B9) is converted to Tetrahydrofolate (THF), an essential coenzyme for:
- Purine synthesis (Adenine, Guanine)
- Thymidine synthesis (via N5,N10-methylene THF and thymidylate synthase)
- Amino acid metabolism
Key Enzymes & Inhibitors:
- Dihydropteroate Synthase (Bacteria only)
- Dihydrofolate Reductase (DHFR)
- Drug: Trimethoprim (TMP) (Primarily bacterial DHFR)
- MoA: Inhibits bacterial DHFR ⟹ THF.
- Use: UTIs, PJP (synergistic with SMX = TMP-SMX/Co-trimoxazole).
- AEs: Megaloblastic anemia, leukopenia, hyperkalemia. (Leucovorin can reduce bone marrow effects).
- Drug: Methotrexate (MTX) (Human DHFR)
- MoA: Inhibits human DHFR ⟹ THF ⟹ DNA/RNA synthesis.
- Use: Cancer, rheumatoid arthritis, psoriasis, ectopic pregnancy, immunosuppression.
- AEs: Myelosuppression (dose-limiting), mucositis, hepatotoxicity, pulmonary fibrosis, nephrotoxicity, teratogenic.
- Leucovorin (Folinic Acid) Rescue: Bypasses DHFR block in normal cells to reduce MTX toxicity.
- Leucovorin is 5-formyl-tetrahydrofolate. This means its core pteridine ring structure is already in the fully reduced (tetrahydro) state, the same state that DHFR aims to achieve.
- Drug: Pyrimethamine (Protozoal DHFR)
- MoA: Inhibits protozoal DHFR.
- Use: Toxoplasmosis (with sulfadiazine), malaria.
- AEs: Megaloblastic anemia. (Leucovorin can reduce bone marrow effects).
- Drug: Trimethoprim (TMP) (Primarily bacterial DHFR)
- Thymidylate Synthase (Requires N5,N10-methylene THF from folate pathway)
- Drug: 5-Fluorouracil (5-FU)
- MoA: Pyrimidine analog; active metabolite FdUMP forms a complex with thymidylate synthase and N5,N10-methylene THF, inhibiting dTMP (“thymineless death”).
- Use: Solid tumors (e.g., colorectal, breast, pancreatic).
- AEs: Myelosuppression, mucositis/diarrhea, hand-foot syndrome, photosensitivity.
- Leucovorin (Folinic Acid) Potentiation: Enhances 5-FU efficacy by stabilizing the inhibitory complex (different role than with MTX).
- Note: DPD deficiency increases 5-FU toxicity.
- Drug: 5-Fluorouracil (5-FU)
| Drug | Target Enzyme/Process | Primary Use(s) | Key Adverse Effects | Leucovorin Interaction |
|---|---|---|---|---|
| Sulfonamides | Bacterial Dihydropteroate Synthase | UTIs, PJP (bacterial infections) | Hypersensitivity, photosensitivity, crystalluria, G6PD hemolysis | N/A |
| Trimethoprim | Bacterial Dihydrofolate Reductase (DHFR) | UTIs, PJP (bacterial infections, with SMX) | Megaloblastic anemia, leukopenia, hyperkalemia | Rescue (bone marrow) |
| Methotrexate | Human Dihydrofolate Reductase (DHFR) | Cancer, autoimmune disease, ectopic pregnancy | Myelosuppression, mucositis, hepatotoxicity, teratogenic | Rescue (reduces toxicity) |
| Pyrimethamine | Protozoal Dihydrofolate Reductase (DHFR) | Toxoplasmosis, malaria | Megaloblastic anemia | Rescue (bone marrow) |
| 5-Fluorouracil | Thymidylate Synthase (via FdUMP & N5,N10-methylene THF complex) | Solid tumors (e.g., colorectal cancer) | Myelosuppression, mucositis, diarrhea, hand-foot syndrome | Potentiation (increases efficacy) |
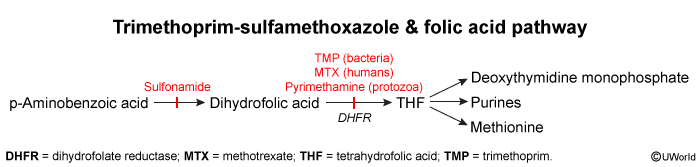
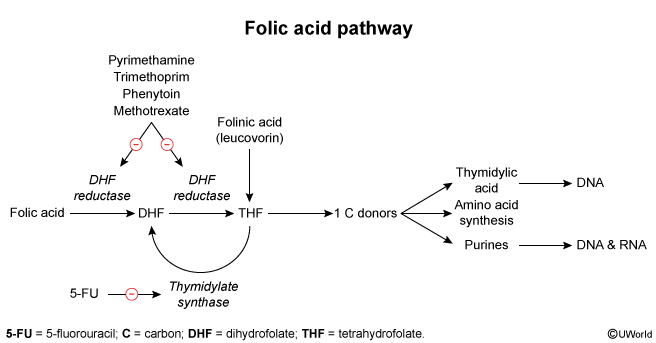 Para-aminobenzoic acid (PABA) is a folic acid precursor in prokaryotes. Sulfonamide antibiotics are chemical analogues of PABA that inhibit the enzyme dihydropteroate synthetase, preventing bacterial conversion of PABA to folic acid. Humans lack the ability to convert PABA to folic acid and require dietary folate.
Para-aminobenzoic acid (PABA) is a folic acid precursor in prokaryotes. Sulfonamide antibiotics are chemical analogues of PABA that inhibit the enzyme dihydropteroate synthetase, preventing bacterial conversion of PABA to folic acid. Humans lack the ability to convert PABA to folic acid and require dietary folate.
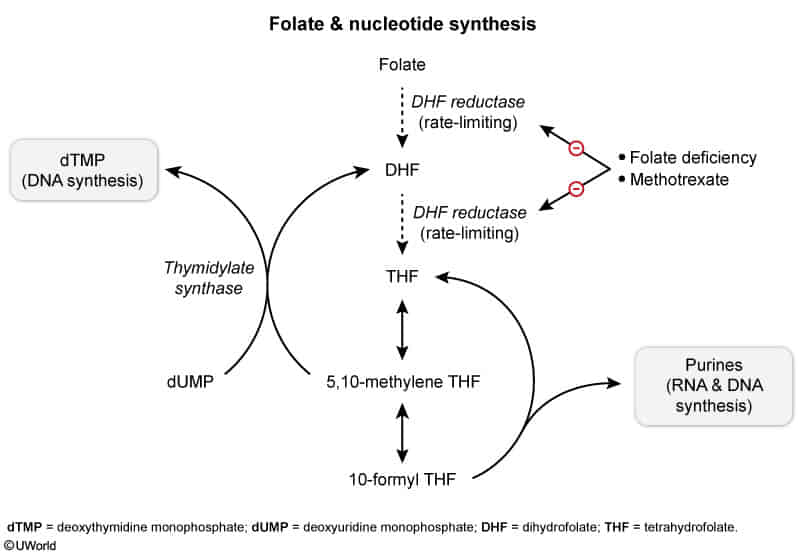 The enzyme thymidylate synthase is responsible for converting deoxyuridine monophosphate (dUMP) to deoxythymidine monophosphate (dTMP). Although most enzymes involved in one-carbon metabolism maintain folate in its active tetrahydrofolate form, thymidylate synthase is unique in that it oxidizes 5,10-methylenetetrahydrofolate to dihydrofolate. This makes de novo thymidine synthesis particularly susceptible to folate-deficient conditions because tetrahydrofolate must be continuously regenerated by dihydrofolate reductase.
The enzyme thymidylate synthase is responsible for converting deoxyuridine monophosphate (dUMP) to deoxythymidine monophosphate (dTMP). Although most enzymes involved in one-carbon metabolism maintain folate in its active tetrahydrofolate form, thymidylate synthase is unique in that it oxidizes 5,10-methylenetetrahydrofolate to dihydrofolate. This makes de novo thymidine synthesis particularly susceptible to folate-deficient conditions because tetrahydrofolate must be continuously regenerated by dihydrofolate reductase.