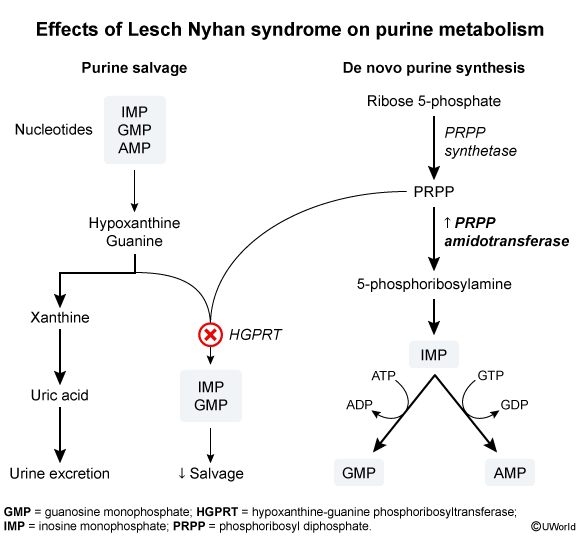
Definition: inherited genetic disorder characterized by impaired purine salvage pathway, resulting in an overproduction of uric acid
Epidemiology
Etiology
Pathophysiology
Purine Salvage Pathway
- Goal: Recycle free purine bases to reform nucleotides, conserving energy.
- Key Enzymes:
- HGPRT (Hypoxanthine-guanine phosphoribosyltransferase):
- Converts Hypoxanthine → IMP.
- Converts Guanine → GMP.
- APRT (Adenine phosphoribosyltransferase):
- Converts Adenine → AMP.
- Lesch-Nyhan Syndrome: X-linked recessive deficiency of HGPRT.
- Patho: Inability to salvage hypoxanthine and guanine leads to their degradation, causing excess uric acid production. Also leads to ↑ de novo purine synthesis due to ↑ PRPP levels.
- Presentation (HGPRT):
Link to original
Clinical features
- Usually asymptomatic for the first 6 months of life
- Orange sand-like sodium urate crystals can be found in the diapers of infants with hyperuricemia.
- See Uric acid stones
- Developmental delay and cognitive impairment
- Pyramidal and extrapyramidal symptoms (e.g., dystonia, spasticity)
- Gouty arthritis, urate nephropathy
- Due to the accumulation of uric acid in peripheral tissues
- Aggression, self-injurious behavior
- E.g., finger chewing, lip biting, headbanging
- Renal failure
Diagnostics
- Hyperuricemia
- ↓ HGPRT activity
- ↑ Phosphoribosyl pyrophosphate amidotransferase (converts PRPP to GMP and AMP)
- Macrocytosis (megaloblastic anemia may occur)
Treatment
- Reduce uric acid levels:
- Allopurinol (first-line)
- Febuxostat (second-line)
- Low-purine diet