- Pericardial Effusion: Accumulation of excess fluid in the pericardial sac. Normally, the sac contains 15-50 mL of fluid. The clinical impact depends more on the rate of accumulation than the total volume. Slow-growing effusions can become very large before causing symptoms.
- Cardiac Tamponade: A medical emergency that occurs when pericardial fluid accumulates under high pressure, compressing the heart. This compression restricts ventricular diastolic filling, leading to decreased stroke volume and cardiac output, resulting in obstructive shock.
Epidemiology
Etiology
- Hemopericardium: accumulation of blood in pericardial space
- Cardiac wall rupture (e.g., complication of myocardial infarction)
- Chest trauma (traumatic cardiac tamponade)
- Aortic dissection
- Serous or serosanguinous pericardial effusion
- Idiopathic
- Pericarditis (especially viral, but also fungal, tuberculous or bacterial)
- Malignancy (e.g. metastatic spread of noncardiac tumors)
- Postpericardiotomy syndrome
- Uremia
- Autoimmune disorders
Pathophysiology
Clinical features
- Pericardial Effusion: Often asymptomatic. May have symptoms related to the underlying cause or vague complaints like dyspnea, cough, or chest discomfort that improves when leaning forward.
- Cardiac Tamponade: Patients present with signs of cardiogenic or obstructive shock, including dyspnea, tachycardia, dizziness, or syncope. Key classic findings include:
- Beck’s Triad: Hypotension, distended neck veins (↑ JVP), and muffled or distant heart sounds. This triad is specific but not always present.
- Pulsus Paradoxus: An exaggerated drop in systolic blood pressure (>10 mmHg) during inspiration. This is a key finding suggesting tamponade.
- Kussmaul’s Sign: A paradoxical rise in JVP on inspiration, may sometimes be seen.
Diagnostics
ECG
- Low voltage complexes and electrical alternans in larger effusions
- Electrical alternans: consecutive QRS complexes that alternate in height due to the swinging motion of the heart when surrounded by large amounts of pericardial fluid
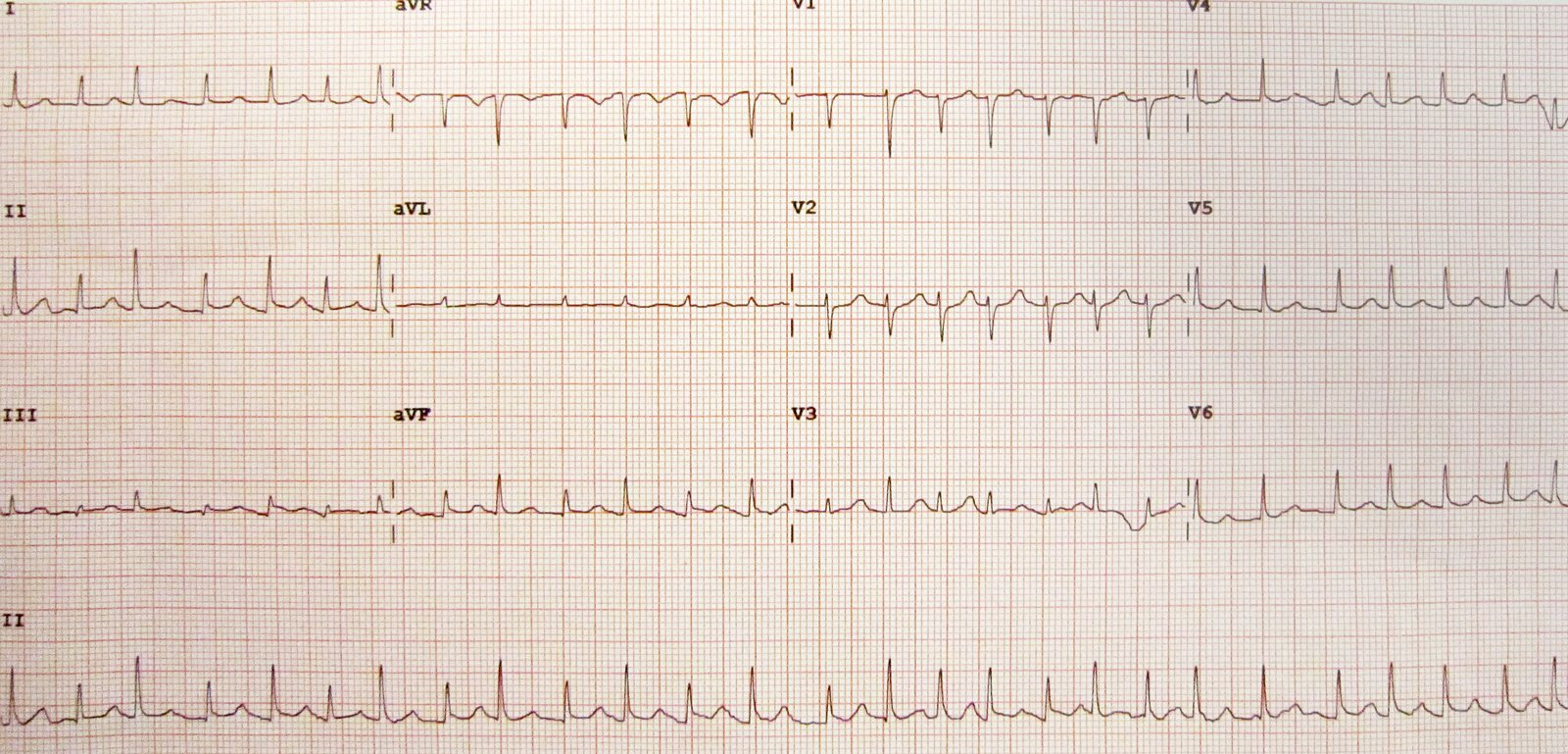
- Electrical alternans: consecutive QRS complexes that alternate in height due to the swinging motion of the heart when surrounded by large amounts of pericardial fluid
Tip
Don’t confuse this with pulse alternans (beat-to-beat variation in pulse amplitude (ie, systolic blood pressure)), which is most commonly seen in patients with severe LV systolic dysfunction (possibly related to the effect of the Frank-Starling mechanism on the failing ventricle)
Treatment
- Effusion (Hemodynamically Stable):
- Tx underlying cause (e.g., hemodialysis for uremia, NSAIDs/colchicine for viral pericarditis).
- Serial echocardiograms. Avoid diuretics (can lower filling pressures).
- Cardiac Tamponade (Unstable - Obstructive Shock):
- Initial/Stabilize: IVF bolus (increases right-sided filling pressures to overcome intrapericardial pressure). Strictly avoid vasodilators and diuretics.
- First-line Definitive: Urgent Pericardiocentesis (echo-guided preferred, or subxiphoid approach if crashing/peri-arrest).
- Refractory/Recurrent: Pericardial window (subxiphoid pericardiotomy)
- Surgical removal of part of the pericardium to allow pericardial fluid to drain into the pleural or peritoneal cavity
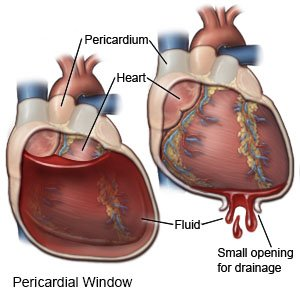
- Highly indicated for recurrent malignant effusions or uremic effusions refractory to dialysis. t Emergent thoracotomy indicated for penetrating chest trauma.
- Surgical removal of part of the pericardium to allow pericardial fluid to drain into the pleural or peritoneal cavity