Pharmacodynamics
- Antiinflammatory and immunosuppressive
- Inhibit Phospholipase A2: Blocks production of arachidonic acid derivatives (prostaglandins, leukotrienes).
- Inhibit NF-κB: Prevents transcription of proinflammatory cytokines (e.g., IL-2, TNF-α).
- Induces apoptosis of T-lymphocytes.
- Hematologic Effects (High Yield)
- Neutrophilia: Caused by demargination of neutrophils from the vessel wall (decreased adhesion molecules). Note: This increases total WBC count but does not indicate infection.
- Lymphopenia & Eosinopenia: Caused by sequestration in lymph nodes and apoptosis. “Corticosteroids cause eosinophils to vanish.” t
- Insulin resistant and increased blood glucose
- Increased Glucose Production: Glucocorticoids stimulate the liver to produce more glucose (gluconeogenesis) by increasing the expression of key enzymes. They also enhance the effects of hormones like glucagon, further boosting glucose production.
- Reduced Glucose Uptake: They impair insulin signaling in tissues like muscle and fat, making them less responsive to insulin, reducing glucose uptake from the blood. Glucocorticoids can also directly inhibit insulin secretion from the pancreas.
- Altered Fat Metabolism: Glucocorticoids promote fat breakdown (lipolysis), increasing free fatty acids in the blood, which contributes to insulin resistance. Chronic exposure can also increase abdominal fat (visceral adiposity), linked to insulin resistance.
- Other:
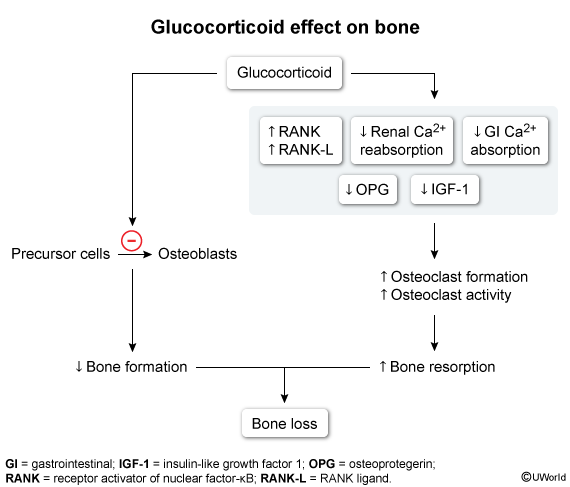
- ↑ Bone resorption: Inhibits osteoblast activity and decreases intestinal Ca2+ absorption, leading to osteoporosis.
- Mineralocorticoid effects (variable): Some glucocorticoids (e.g., hydrocortisone, prednisone) can bind to mineralocorticoid receptors, causing Na+ and water retention, and K+ excretion.
- CNS effects: Can cause insomnia, anxiety, psychosis (“steroid psychosis”).
Adverse effects
- Cushingoid appearance (moon facies, truncal obesity)
- Hyperglycemia (↑ gluconeogenesis)
- Osteoporosis & Avascular necrosis (femoral head)
- HPA axis suppression (requires tapering)
- Immunosuppression (↑ infection risk, impaired healing)
- Hypertension & Hypokalemia (mineralocorticoid effect)
- Gastritis/Peptic Ulcers (esp. with NSAIDs)
- Psychosis/Insomnia
- Cataracts & Glaucoma
- Proximal myopathy & skin striae/atrophy
Metabolism, electrolytes and endocrine system
- Hyperglycemia and ↑ insulin resistance → glucocorticoid-induced diabetes
Other
Drugs
Mnemonic
长米的中坡可短了
- 短效:可的松,氢化可的松
- 中效:泼尼松,泼尼松龙,甲泼尼松龙,曲安西龙
- 长效:地塞米松,倍他米松
Short-Acting (Biological Half-life: 8-12 hours)
- Drugs:
- Hydrocortisone (Cortisol)
- Cortisone
- Key Features:
- Have both glucocorticoid and mineralocorticoid effects.
- Best for replacement therapy in adrenal insufficiency (e.g., Addison’s disease) due to their shorter duration, which mimics the natural diurnal cortisol rhythm.
Intermediate-Acting (Biological Half-life: 12-36 hours)
- Drugs:
- Prednisone
- Prednisolone
- Methylprednisolone
- Triamcinolone
- Key Features:
- Most commonly prescribed group for a wide range of inflammatory and autoimmune conditions.
- Offer potent anti-inflammatory effects with lower mineralocorticoid activity compared to short-acting agents (especially methylprednisolone and triamcinolone).
- Prednisone is a prodrug, converted to its active form, prednisolone, in the liver.
Long-Acting (Biological Half-life: 36-72 hours)
- Drugs:
- Dexamethasone
- Betamethasone
- Key Features:
- Highest glucocorticoid potency with virtually no mineralocorticoid effect.
- Used for conditions requiring potent, long-lasting anti-inflammatory or immunosuppressive effects (e.g., severe asthma exacerbations, cerebral edema, certain cancers).
- High risk of hypothalamic-pituitary-adrenal (HPA) axis suppression, making them less ideal for long-term daily use but suitable for short-term, high-dose therapy.