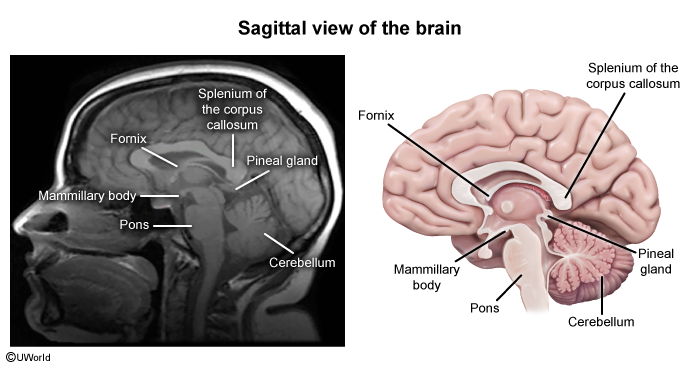
Sagittal section of the brain
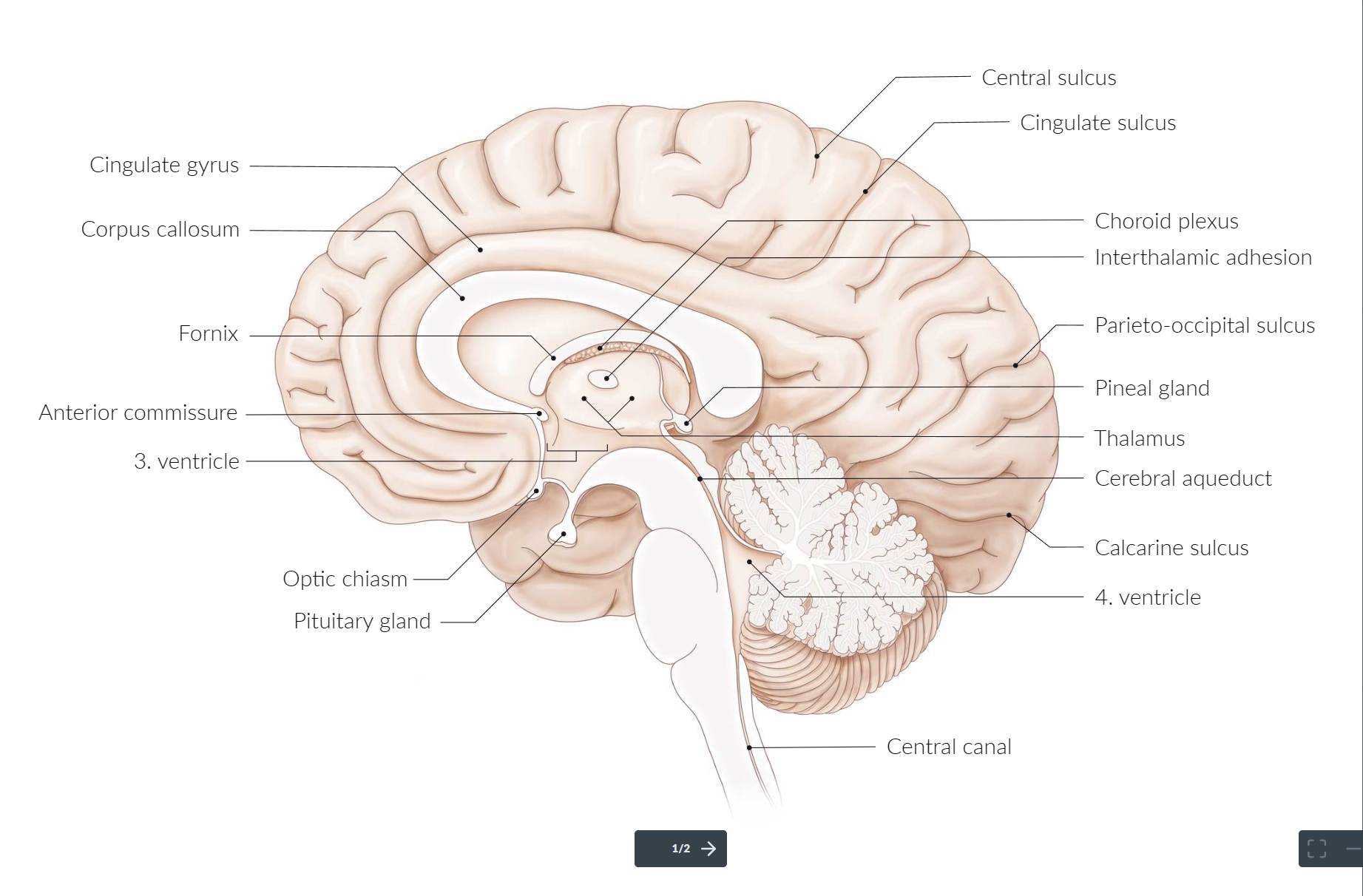
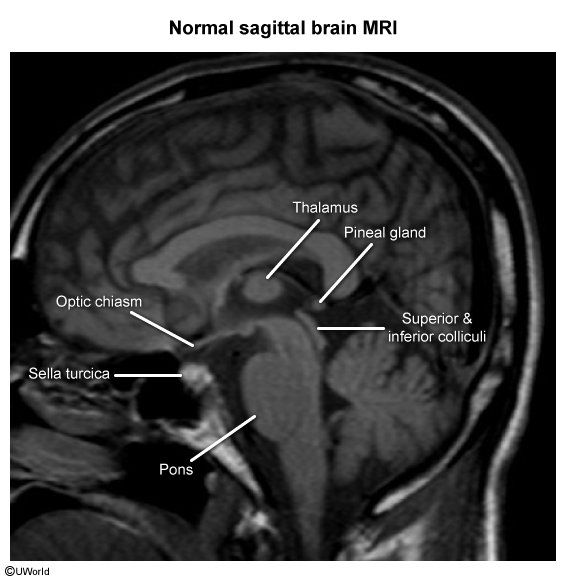
Cerebral cortex
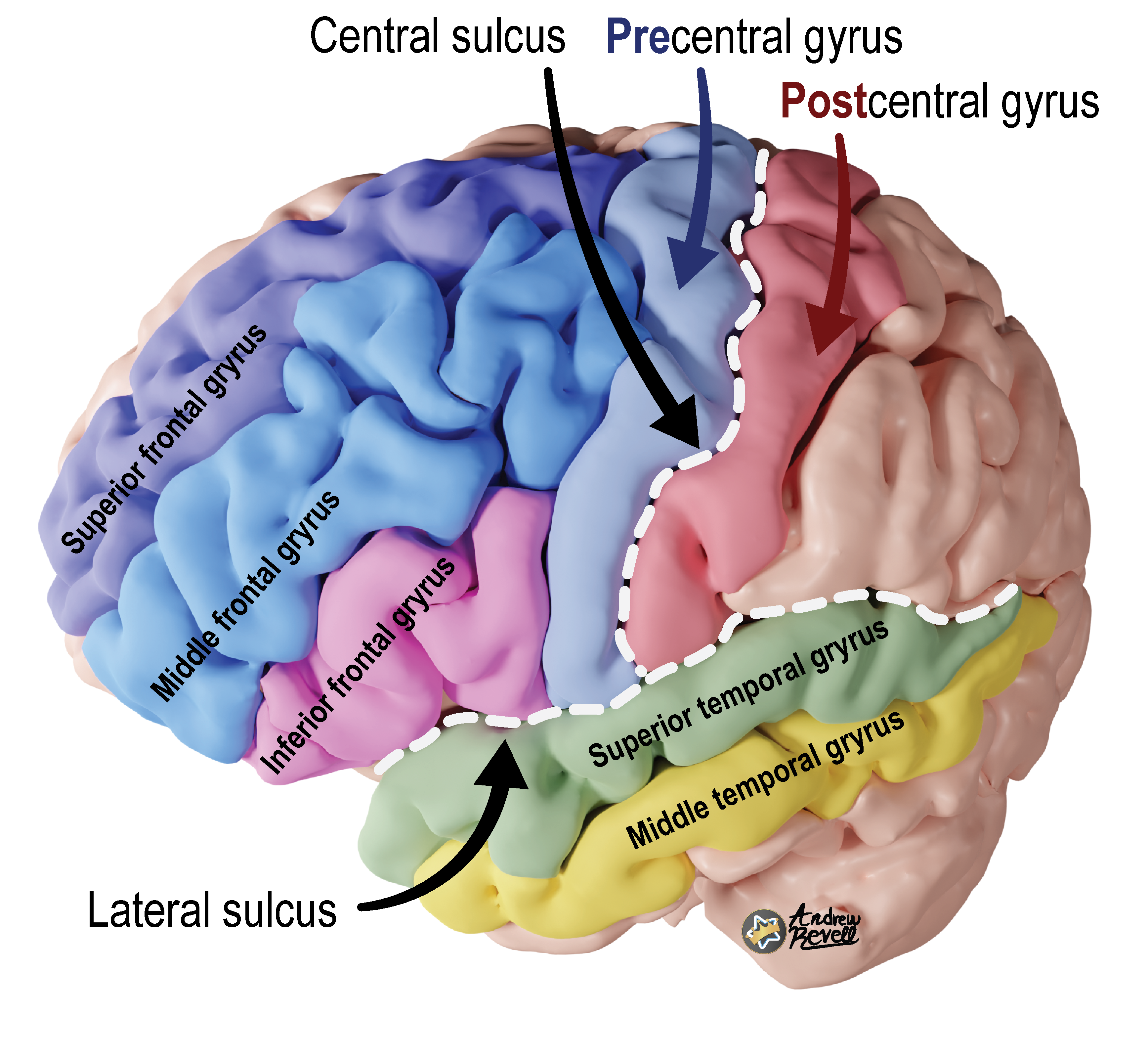
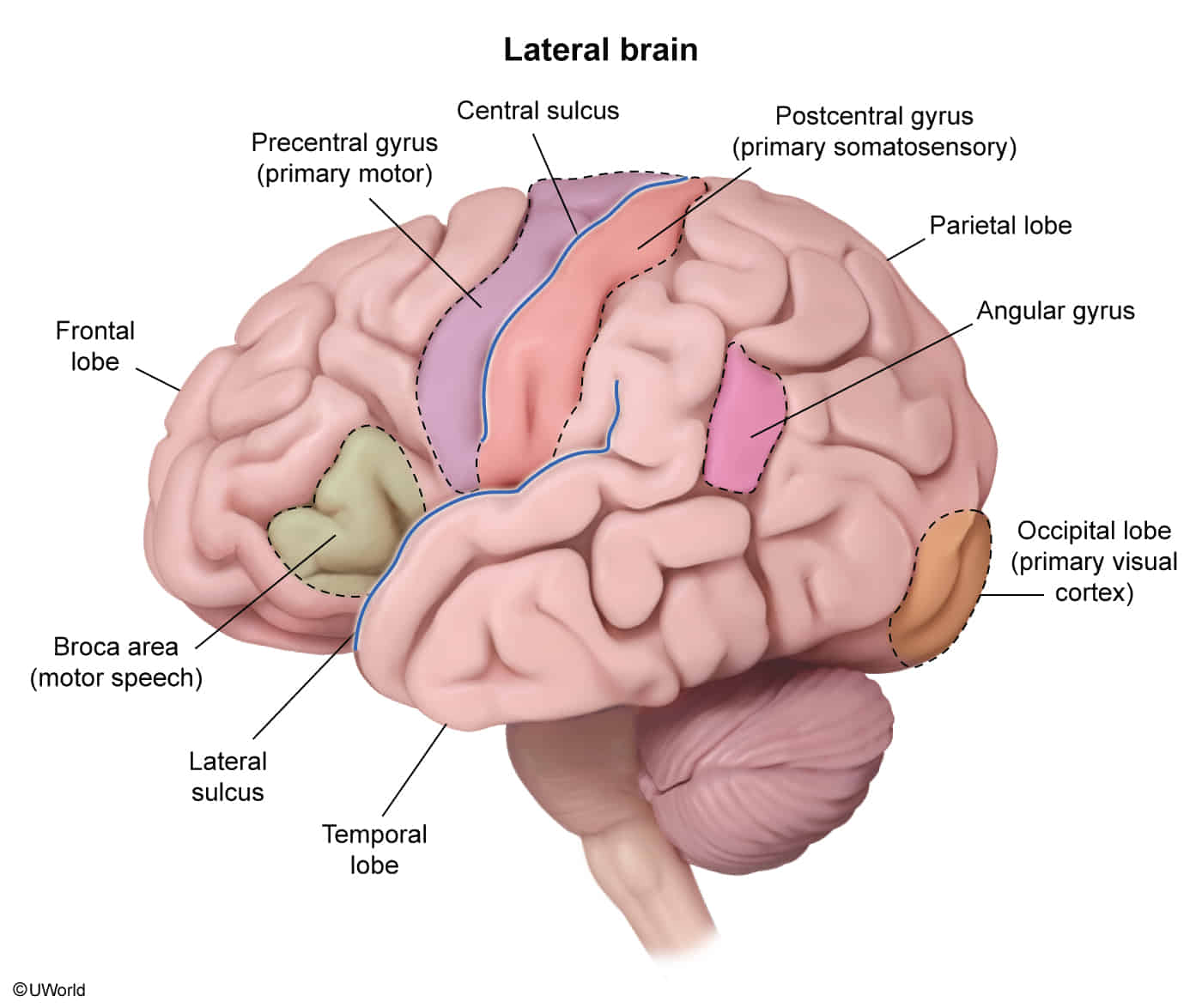
Frontal Lobe
- Key Functions:
- Prefrontal Cortex: Executive functions (planning, organization, problem-solving), personality, working memory, and social behavior.
- Primary Motor Cortex (Precentral Gyrus): Voluntary motor control of the contralateral body. Organized as a motor homunculus.
- Broca’s Area (Inferior Frontal Gyrus, usually Left): Motor control of speech production. t
- Frontal Eye Fields: Voluntary, conjugate eye movements to the contralateral side.
Mnemonic
- Pre = in front → you have to “plan” or initiate motor actions first (movement comes before sensation in voluntary actions).
- Post = behind → sensation comes post (after) the action, as feedback.
Parietal Lobe
- Key Functions:
- Primary Somatosensory Cortex (Postcentral Gyrus): Processes contralateral sensation (touch, pressure, pain, temperature, proprioception). Organized as a sensory homunculus.
- Inferior Parietal Lobule (Dominant Hemisphere, usually Left): Language comprehension (part of Wernicke’s area), calculations (Gerstmann syndrome).
- Inferior Parietal Lobule (Non-dominant Hemisphere, usually Right): Spatial awareness, navigation, and contralateral sensory integration.
- Lesion Presentation:
- Primary Somatosensory Cortex Lesion: Contralateral loss of sensation.
- Gerstmann Syndrome (Dominant Parietal Lobe): Acalculia, agraphia, finger agnosia, and left-right disorientation.
- Contralateral Hemineglect (Non-dominant Parietal Lobe): Patient ignores the contralateral side of their body and space.
Temporal Lobe
- Key Functions:
- Primary Auditory Cortex (Superior Temporal Gyrus): Processes auditory information.
- Wernicke’s Area (Superior Temporal Gyrus, usually Left): Language comprehension.
- Hippocampus (Medial Temporal Lobe): Formation of new memories (consolidation).
- Amygdala (Medial Temporal Lobe): Processing of emotions, especially fear. t
- Lesion Presentation:
- Wernicke’s Aphasia (Receptive Aphasia): Fluent but nonsensical speech (“word salad”) with impaired comprehension. Patients are often unaware of their deficit.
- Bilateral Hippocampal Lesion: Anterograde amnesia (inability to form new memories).
- Klüver-Bucy Syndrome (Bilateral Amygdala Lesion): Hyperphagia, hypersexuality, hyperorality, and visual agnosia.
- Auditory hallucinations, seizures.
Occipital Lobe
- Key Functions:
- Primary Visual Cortex (banks of the calcarine sulcus): Processes primary visual information from the contralateral visual field.
- Lesion Presentation:
- Contralateral Homonymous Hemianopia: Loss of the same half of the visual field in both eyes.
- Macular Sparing: A lesion of the primary visual cortex may spare central vision due to dual blood supply from the MCA and PCA.
- Visual Agnosia: Inability to recognize objects despite intact vision.
Cerebral Blood Supply (High-Yield Vessels)
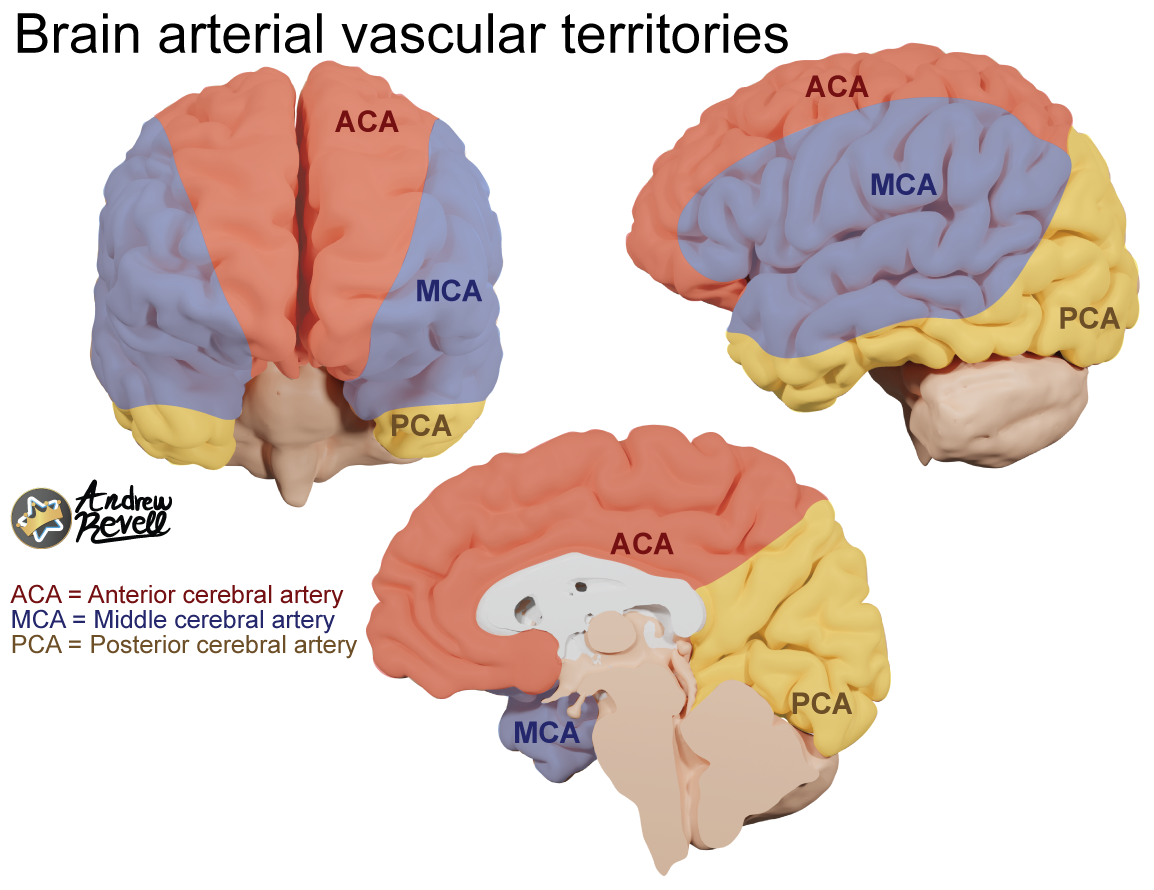
- Anterior Cerebral Artery (ACA):
- Supplies: Medial surfaces of the frontal and parietal lobes.
- Stroke Sx: Contralateral lower extremity motor and sensory deficits.
- Middle Cerebral Artery (MCA):
- Supplies: Lateral surfaces of all four lobes, including motor/sensory cortices for the upper limb and face, and language areas (Broca’s, Wernicke’s).
- Stroke Sx: Most common site of ischemic stroke. Contralateral face/upper extremity motor and sensory deficits, aphasia (if dominant hemisphere), hemineglect (if non-dominant).
- Posterior Cerebral Artery (PCA):
- Supplies: Occipital lobe, inferior temporal lobe, thalamus.
- Stroke Sx: Contralateral homonymous hemianopia with macular sparing.
Meninges and spaces
1. Anatomical Relationships and Size of Spaces
The meninges consist of three layers surrounding the brain and spinal cord:
- Dura mater (outermost, tough layer)
- Arachnoid mater (middle, web-like layer)
- Pia mater (innermost, delicate layer adherent to the brain surface)
Between these layers, there are spaces:
- Epidural space: Between the dura mater and the skull (or vertebral bones).
- In the cranial cavity, this space is a potential space because the dura is tightly adherent to the skull. Has Middle Meningeal Artery.
- In the spinal canal, the epidural space is a real space containing fat and venous plexuses.
- Thickness: In the spinal canal, approx. 1-3 mm, variable by location.
- Subdural space: Between dura mater and arachnoid mater.
- This is a potential space; normally the arachnoid and dura are in close contact. Has Bridging Veins.
- Thickness: Minimal under normal conditions, expands pathologically if bleeding occurs (subdural hematoma).
- Subarachnoid space: Between arachnoid mater and pia mater.
- This is a real space filled with cerebrospinal fluid (CSF), trabeculae, and blood vessels.
- Thickness: Variable depending on location; generally about 1-5 mm.
- This space extends around the brain and spinal cord.
2. Functions of Each Layer and Their Spaces
- Dura Mater
- Function: Provides a tough protective outer covering; dural septa compartmentalize brain regions (falx cerebri, tentorium cerebelli).
- In spinal cord, dura mater forms a protective covering and encloses the epidural space.
- Epidural Space
- In the spine: provides cushioning and a route for venous return.
- Clinical use: Site for epidural anesthesia.
- Arachnoid Mater
- Function: Thin, web-like membrane facilitating the passage of blood vessels.
- Its trabeculae extend to the pia mater.
- Subdural Space
- Normally a potential space; no major function.
- Clinical: Site where blood can accumulate during traumatic injury (subdural hematoma).
- Subarachnoid Space
- Function: Contains CSF, which cushions and nourishes the brain.
- Its trabeculae suspend the brain within the skull.
- Contains cerebral arteries and veins.
- Pia Mater
- Delicate membrane tightly adherent to the brain surface.
- Supports tiny blood vessels entering brain tissue.
- Participates in blood-brain barrier and nutrient exchange.
3. Clinical Relevance
| Space | Clinical Points |
|---|---|
| Epidural Space | - In spinal epidural analgesia/anesthesia - Epidural hematomas (cranial) occurring between dura and skull are arterial and rapid |
| Subdural Space | - Subdural hematomas from bridging vein tearing; venous, slower onset - Potential space expands with blood accumulation |
| Subarachnoid Space | - Site of CSF flow; lumbar puncture accesses this space - Subarachnoid hemorrhage (from ruptured aneurysm) is life-threatening |
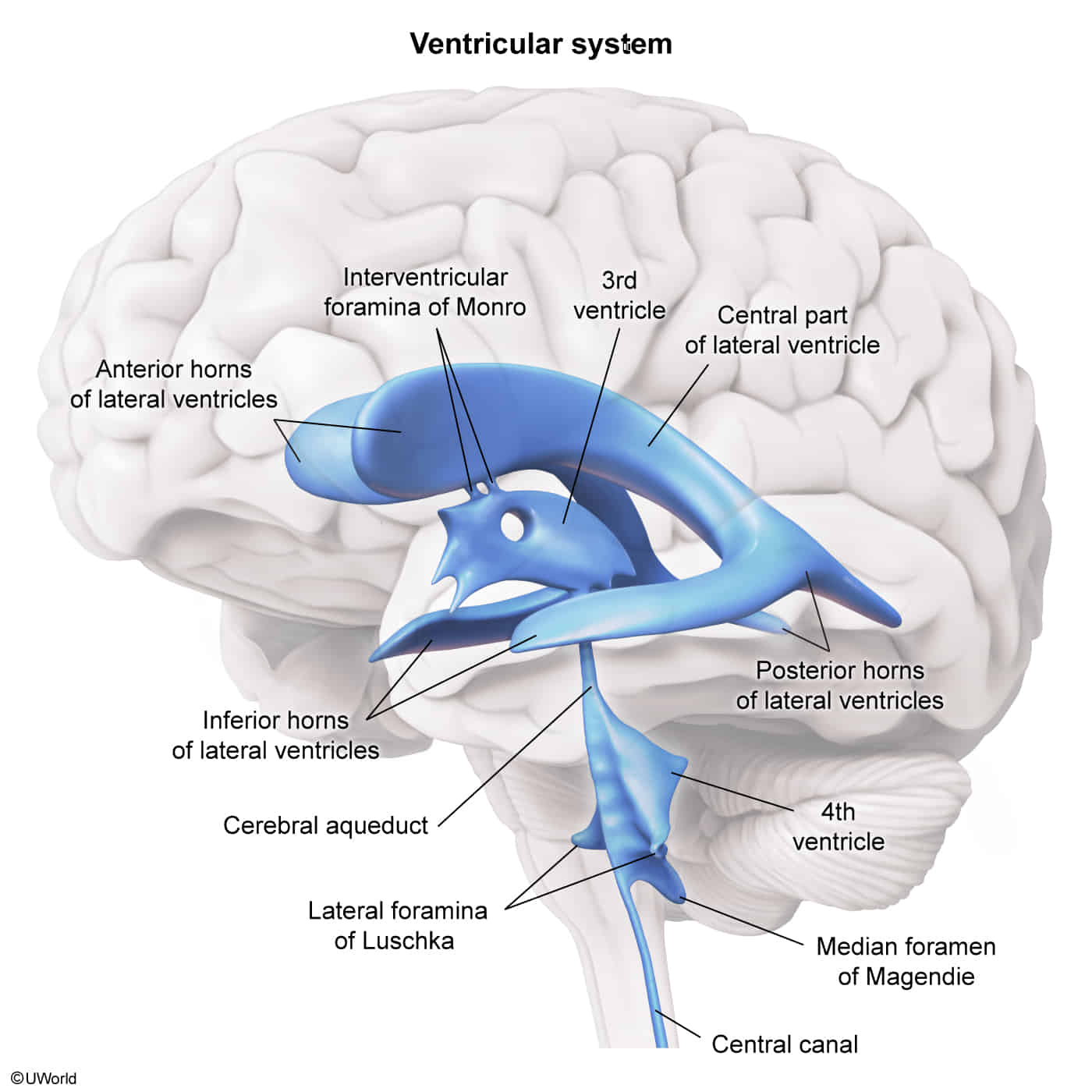
Ventricular system
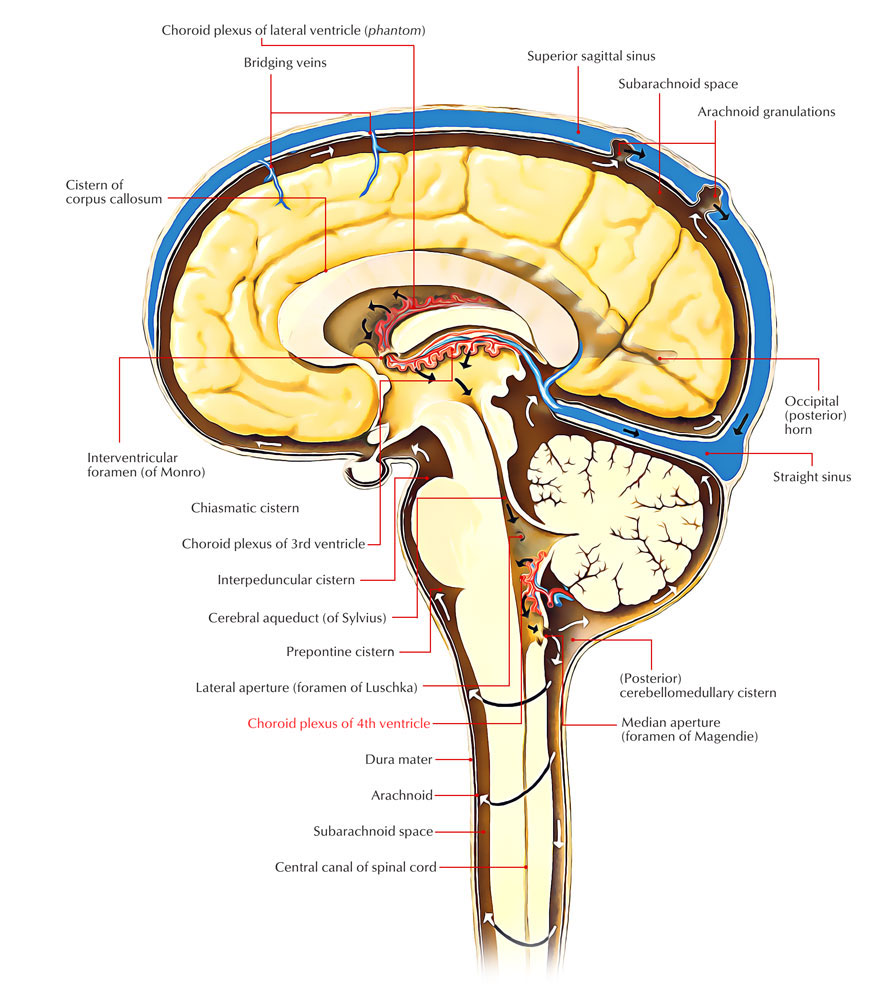 CSF flow: CSF production: produced by choroid plexuses in the lateral, third, and fourth ventricles by filtration of plasma → lateral ventricles → third ventricle (via interventricular foramina) → fourth ventricle (via cerebral aqueduct) → diffusion and active transfer into the subarachnoid space (via foramina of Luschka and Magendie) → reabsorption in the arachnoid granulations (a group of projections of the arachnoid mater into the dural sinuses) → drainage into the dural venous sinuses → internal jugular veins, ultimately heart
CSF flow: CSF production: produced by choroid plexuses in the lateral, third, and fourth ventricles by filtration of plasma → lateral ventricles → third ventricle (via interventricular foramina) → fourth ventricle (via cerebral aqueduct) → diffusion and active transfer into the subarachnoid space (via foramina of Luschka and Magendie) → reabsorption in the arachnoid granulations (a group of projections of the arachnoid mater into the dural sinuses) → drainage into the dural venous sinuses → internal jugular veins, ultimately heart
Cerebellum
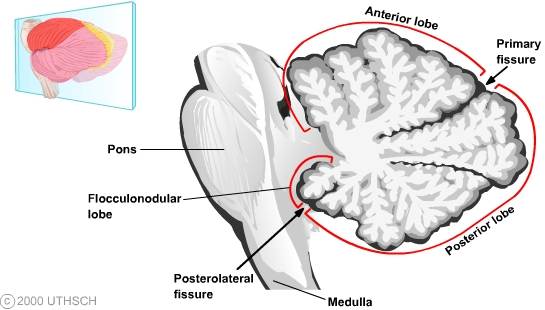 ↑ cross-section view
↓ view from posterior
↑ cross-section view
↓ view from posterior
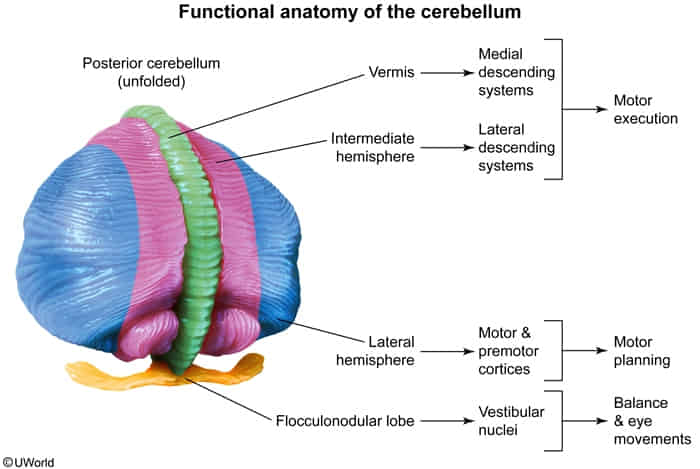
- Function
- Control of balance and ocular movements
- Planning of movements that are about to occur
- Coordination of complex and sequential movements
- Maintenance of muscle tone
Vasculature of the cerebellum
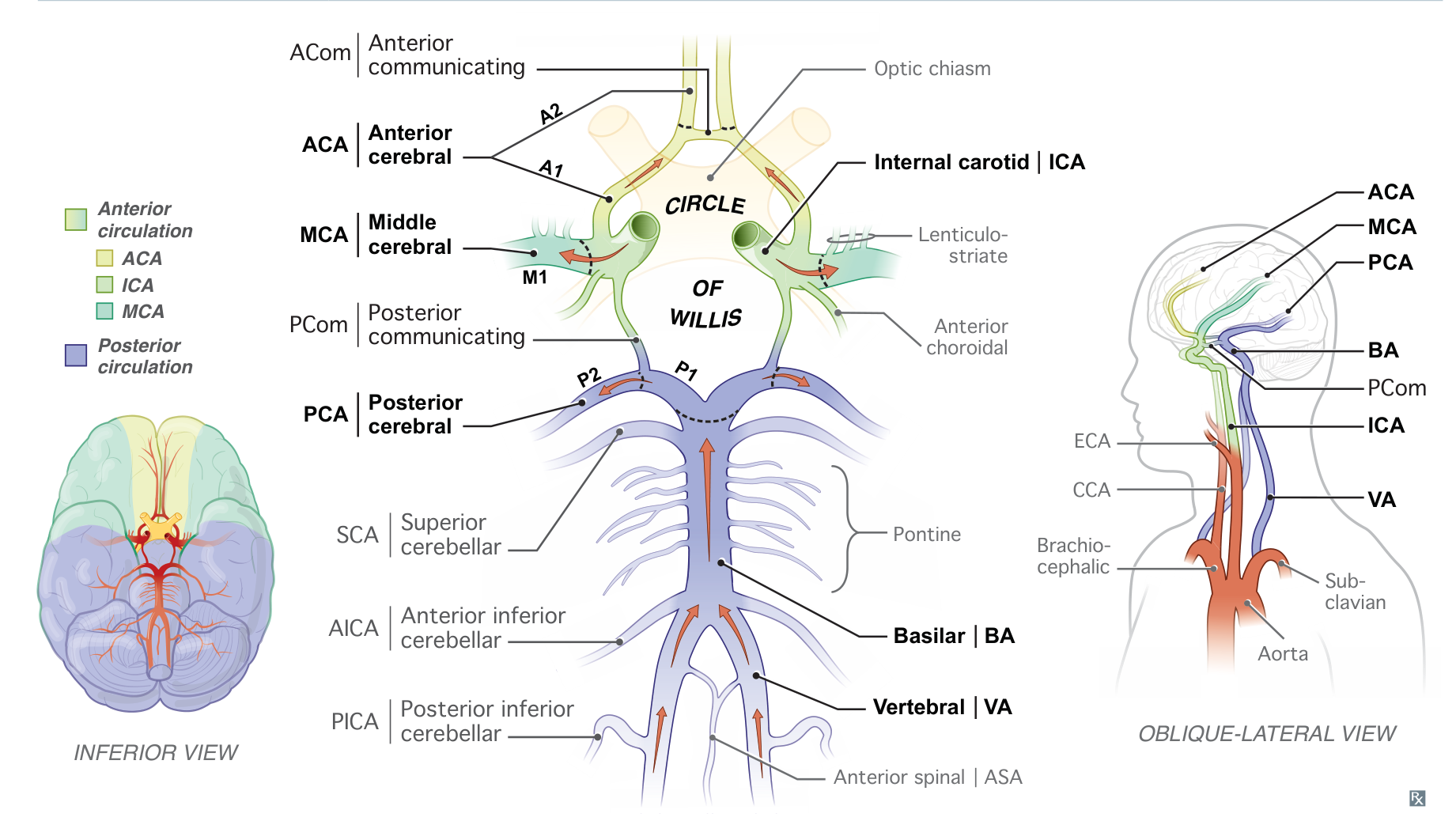
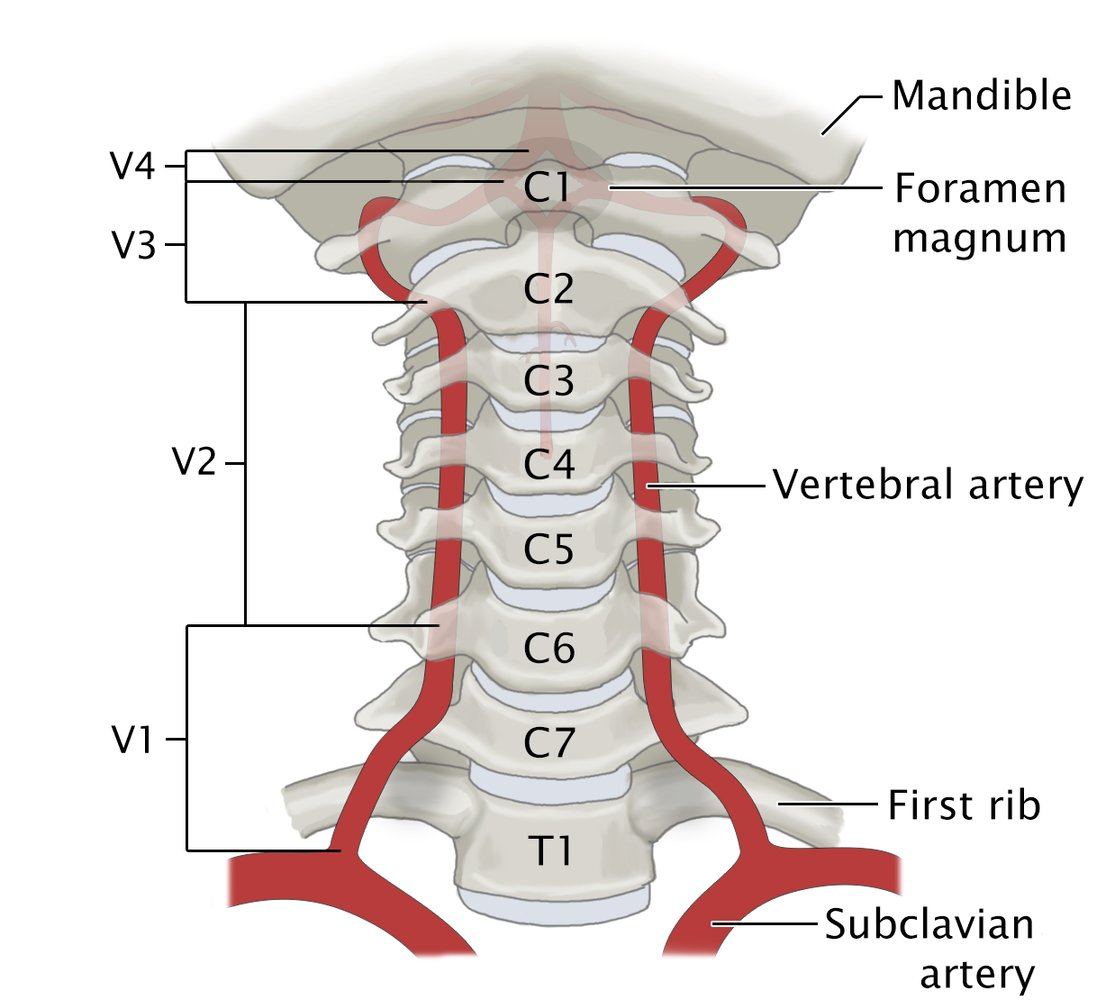
- Basilar artery
- Superior cerebellar artery (SCA) → superior surface of the cerebellum
- Also supplies the superior and middle cerebellar peduncles and the midbrain
- Anterior inferior cerebellar artery (AICA)→ anterior surface of the cerebellum
- Also supplies the middle cerebellar peduncle and inferolateral pons
- Superior cerebellar artery (SCA) → superior surface of the cerebellum
- Vertebral artery
- Posterior inferior cerebellar artery (PICA)→ posterior surface of the cerebellum
- Also supplies the inferior cerebellar peduncles and the inferolateral medulla
- Posterior inferior cerebellar artery (PICA)→ posterior surface of the cerebellum
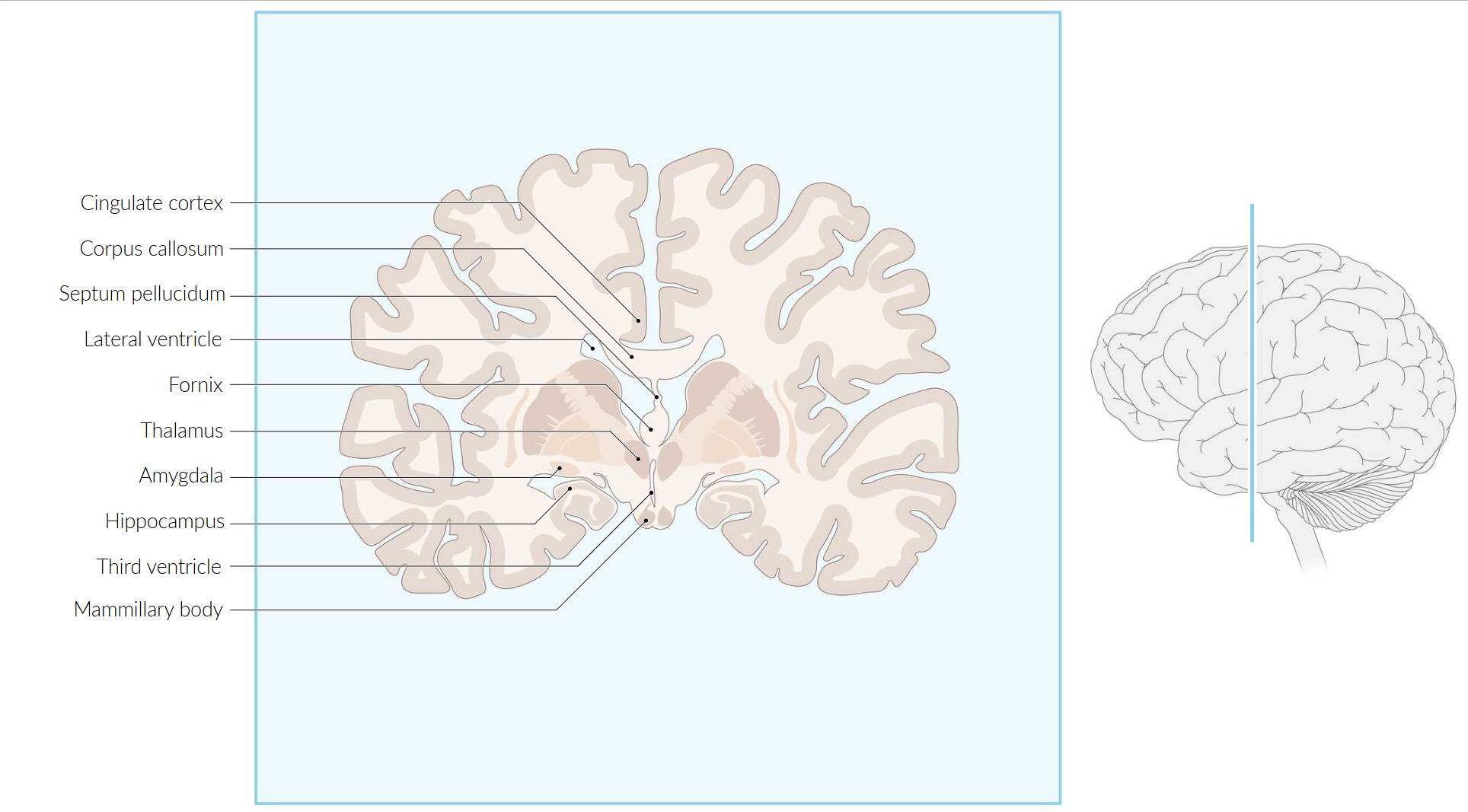
Limbic system
- Function: involved in emotional and behavioral responses, motivation, memory, olfaction, and autonomic nervous system function
- Functions (The 5 F’s)
- Feeding (and other homeostatic functions like thirst, temperature regulation)
- Feeling (emotion, fear, pleasure)
- Fighting (and fleeing; aggression, response to threats)
- Forgetting (memory formation and retrieval)
- Fornication (sexual behavior)
- A popular mnemonic is HOME: Homeostasis, Olfaction, Memory, and Emotion.
- Key Structures & Primary Roles
- Hippocampus: Crucial for the formation of new long-term memories (consolidation). Involved in spatial navigation. Damage leads to anterograde amnesia (inability to form new memories).
- Amygdala: The emotional center, especially for fear, anxiety, and aggression. It attaches emotional significance to memories.
- Hypothalamus: Regulates the autonomic nervous system and the endocrine system via the pituitary gland. It controls basic drives like hunger, thirst, body temperature, and sexual arousal.
- Thalamus: Specifically the anterior and dorsomedial nuclei, which serve as relay stations connecting other limbic structures.
- Cingulate Gyrus: Involved in processing emotion, learning, and memory. It plays a role in linking behavioral outcomes to motivation.
- Mammillary Bodies: Part of the hypothalamus, crucial for recollective memory. Damage is a key feature of Wernicke-Korsakoff syndrome.
- Septal Nuclei: Associated with pleasure, reward, and reinforcement.
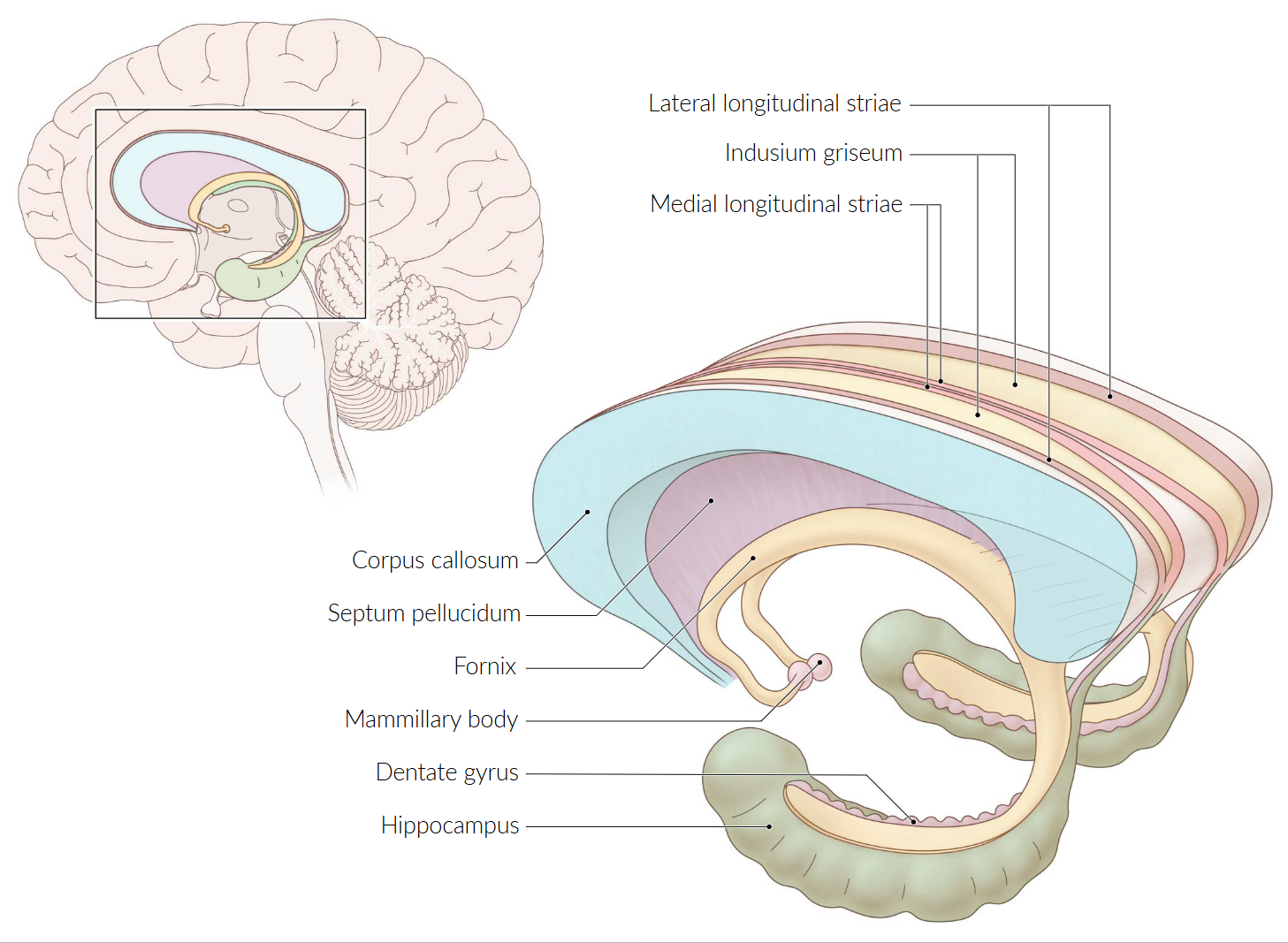
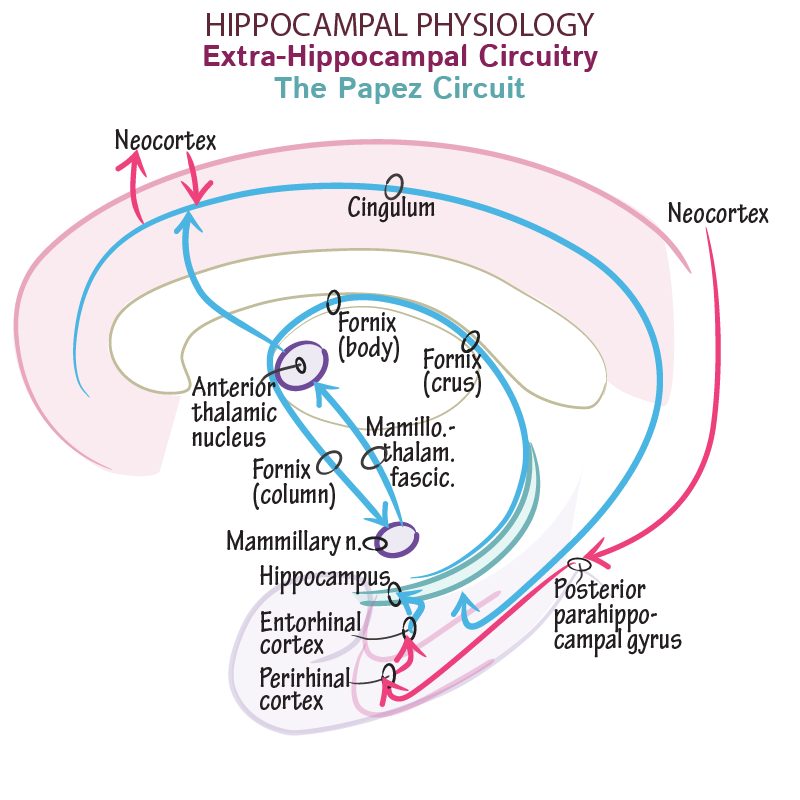
- Papez Circuit
- A historical but still useful model for understanding memory consolidation.
- Pathway: Hippocampus → Fornix → Mammillary Bodies → Mammillothalamic Tract → Anterior Nucleus of the Thalamus → Cingulate Gyrus → Entorhinal Cortex → Hippocampus.
- Lesions anywhere in this circuit can cause memory deficits.
- High-Yield Clinical Correlations
- Klüver-Bucy Syndrome
- Patho/Etiology: Caused by bilateral lesions of the amygdala, most commonly due to HSV-1 encephalitis. Other causes include stroke, trauma, and neurodegenerative diseases.
- Clinical Presentation: Characterized by a constellation of symptoms including:
- Hyperorality: Tendency to put objects in the mouth.
- Hypersexuality: Disinhibited sexual behavior.
- Placidity: Decreased emotional reactivity, loss of fear/anger (docility).
- Visual Agnosia: Inability to recognize familiar objects or people.
- Amnesia: Memory loss.
- Wernicke-Korsakoff Syndrome
- Temporal Lobe Epilepsy: The hippocampus and amygdala are common seizure foci, leading to seizures that may feature olfactory hallucinations (e.g., burning rubber), emotional changes (fear), and autonomic symptoms.
- Schizophrenia: The mesolimbic pathway (connecting the ventral tegmental area to the limbic system) is implicated. Excess dopaminergic activity in this pathway is thought to cause the “positive” symptoms (hallucinations, delusions).
- Alzheimer Disease: Early and severe atrophy of the hippocampus is a hallmark, explaining why memory loss is an early and prominent symptom.
- Klüver-Bucy Syndrome
Thalamus
The thalamus is a pair of large, egg-shaped gray matter structures in the diencephalon. It acts as the primary relay and processing center for almost all sensory and motor information en route to the cerebral cortex.
Key Thalamic Nuclei & Pathways
- Ventral Posterolateral (VPL) Nucleus
- Input: Spinothalamic tract and Dorsal Column-Medial Lemniscus (DCML).
- Senses: Vibration, pain, pressure, proprioception, light touch, and temperature from the body.
- Output: Primary somatosensory cortex.
- Ventral Posteromedial (VPM) Nucleus
- Input: Trigeminal and gustatory pathways.
- Senses: Face sensation and taste.
- Output: Primary somatosensory cortex.
- Mnemonic: VPM for Makeup (on the face).
- Lateral Geniculate Nucleus (LGN)
- Input: Optic nerve (CN II).
- Senses: Vision.
- Output: Primary visual cortex in the occipital lobe.
- Mnemonic: LGN for Light.
- Medial Geniculate Nucleus (MGN)
- Input: Inferior colliculus of the tectum.
- Senses: Hearing.
- Output: Auditory cortex of the temporal lobe.
- Mnemonic: MGN for Music.
- Ventral Lateral (VL) Nucleus
- Input: Basal ganglia (globus pallidus) and cerebellum.
- Function: Motor coordination.
- Output: Motor cortex.
- Anterior Nuclei
- Input: Mammillary bodies via the mammillothalamic tract.
- Function: Part of the Papez circuit of the limbic system, involved in memory and emotion.
- Output: Cingulate gyrus.
Tip
前运动,后感觉,外管四肢,内管面部
Clinical Correlations
- Thalamic Stroke
- Etiology: Most commonly due to occlusion of branches of the Posterior Cerebral Artery (PCA).
- Presentation: Typically results in contralateral sensory loss (face, arm, and leg). May also cause aphasia (dominant hemisphere) or hemineglect (non-dominant hemisphere).
- Artery of Percheron: A rare variant where a single artery supplies both thalami. Occlusion leads to bilateral thalamic infarction, presenting with altered mental status, memory impairment, and vertical gaze palsy.
- Dejerine-Roussy Syndrome (Thalamic Pain Syndrome)
- Pathophysiology: Occurs weeks to months after a thalamic stroke, usually involving the VPL/VPM nuclei.
- Clinical Presentation: Characterized by contralateral neuropathic pain (allodynia, hyperalgesia). Patients describe severe, burning pain in response to stimuli that are not normally painful.
- Wernicke-Korsakoff Syndrome
- Pathophysiology: Caused by thiamine (B1) deficiency, often seen in chronic alcohol use. Leads to damage to the mammillary bodies and the dorsomedial nucleus of the thalamus.
- Clinical Presentation: Characterized by confusion, ataxia, ophthalmoplegia (Wernicke encephalopathy), and anterograde/retrograde amnesia with confabulation (Korsakoff syndrome).
Key Associations
- Papez Circuit: A neural circuit for the control of emotional expression and memory formation (Hippocampus → Mammillary Bodies → Anterior Thalamic Nuclei → Cingulate Gyrus → Hippocampus).
- Reticular Nucleus: A unique GABAergic nucleus that forms a thin sheet around the rest of the thalamus. It does not project to the cortex but instead modulates the activity of other thalamic nuclei, acting as a “gatekeeper” for information flow.
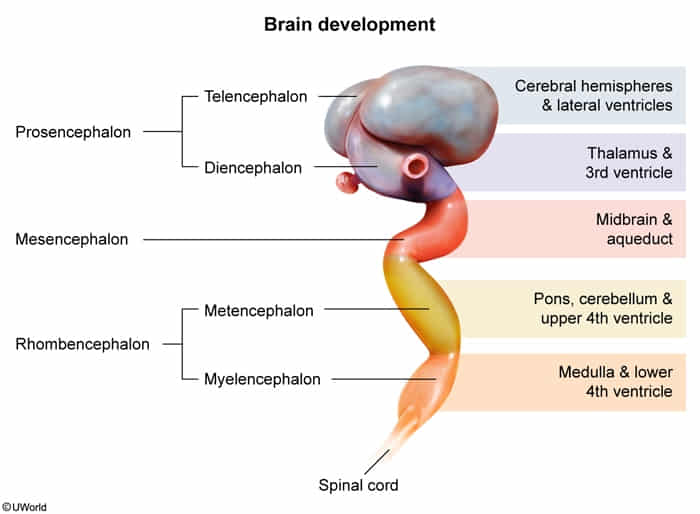
Embryology of the brain
Mnemonic
- Primary brain vesicles
- Please = Prosencephalon (forebrain)
- Make = Mesencephalon (midbrain)
- Room = Rhombencephalon (hindbrain)
- Secondary brain vesicles
- Tell = Telencephalon
- Di = Diencephalon
- Mes = Mesencephalon
- Met = Metencephalon
- My = Myelencephalon
- Primary Vesicles (Week 4)
- Arise from the rostral end of the neural tube.
- Prosencephalon (Forebrain)
- Mesencephalon (Midbrain)
- Rhombencephalon (Hindbrain)
- Secondary Vesicles (Week 5) & Adult Derivatives
- Prosencephalon divides into:
- Telencephalon
- Adult Structures: Cerebral hemispheres, basal ganglia, hippocampus, amygdala
- Ventricle: Lateral ventricles
- Diencephalon
- Adult Structures: Thalamus, Hypothalamus, Epithalamus (pineal gland), Subthalamus
- Ventricle: Third ventricle
- Telencephalon
- Mesencephalon remains undivided:
- Adult Structures: Midbrain (tectum, tegmentum, cerebral peduncles)
- Ventricle: Cerebral aqueduct (of Sylvius)
- Rhombencephalon divides into:
- Metencephalon
- Adult Structures: Pons, Cerebellum
- Ventricle: Upper part of the Fourth ventricle
- Myelencephalon
- Adult Structures: Medulla oblongata
- Ventricle: Lower part of the Fourth ventricle
- Metencephalon
- Prosencephalon divides into:
Brain malformations
- Holoprosencephaly
- Pathophysiology: Failure of forebrain (prosencephalon) to divide into two hemispheres.
- Key Associations: Trisomy 13, mutations in Sonic hedgehog (SHH) gene.
- Clinical Pearl: Associated with midline facial defects (e.g., cyclopia, single nostril, cleft lip/palate). Severity of facial defects predicts severity of brain malformation.
- Lissencephaly (“Smooth Brain”)
- Pathophysiology: Defective neuronal migration, leading to absent gyri (agyria).
- Clinical Features: Severe intellectual disability, microcephaly, intractable seizures.
- Imaging: Smooth cerebral surface, often with an “hourglass” or “figure-8” appearance on axial MRI.
Dominant and non-dominant cortex
- Lateralization
- Left Hemisphere: Dominant (Language) in >95% of right-handers and ~70% of left-handers.
- Right Hemisphere: Non-dominant (Spatial) in most people.
- Dominant Hemisphere (Usually Left)
- Functions: Language, Logic, Math, Praxis.
- Lesions:
- Aphasia: Problems with speech/comprehension (Broca, Wernicke).
- Gerstmann Syndrome (Angular Gyrus/Parietal):
- Agraphia (can’t write).
- Acalculia (can’t do math).
- Finger Agnosia.
- L-R Disorientation.
- Non-Dominant Hemisphere (Usually Right)
- Functions: Spatial attention, Facial recognition, Prosody (emotion in voice).
- Lesions:
- Hemispatial Neglect (Parietal): Ignores contralateral side (usually Left). t
- Constructional Apraxia: Unable to copy drawings/objects.
- Aprosodia: Monotone speech.