Epidemiology
Etiology
- Pathogen
- Group A β‑hemolytic streptococci (Streptococcus pyogenes) produce erythrogenic exotoxin A, B, or C
- These exotoxins cause the rash of scarlet fever via a delayed-type skin reaction.
- Route of transmission: aerosol
Pathophysiology
Clinical features
Exanthem phase
- Rash manifests 12–48 hours after fever onset.
- Fine, erythematous, sandpaper‑like texture
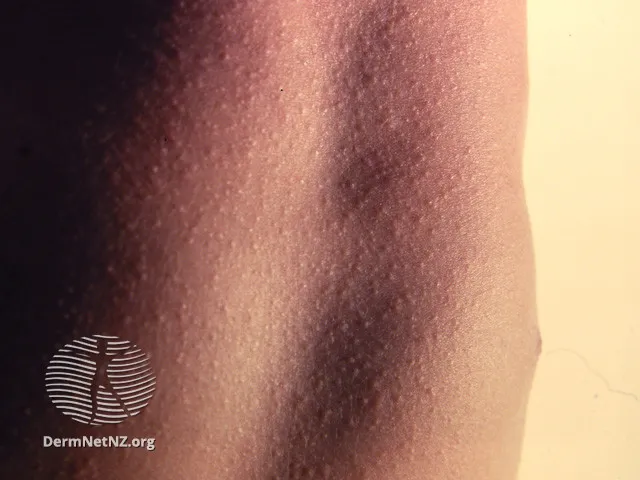
- Blanches with pressure, but nonblanching petechiae may also be present
- Begins on neck or trunk and spreads rapidly across the body (except for the palms and soles)
- Characteristic features include:
- Flushed cheeks with perioral pallor

- Strawberry tongue: bright red tongue color with papillary hyperplasia, which may initially be covered with a white coating
- Pastia lines
- A characteristic sign of scarlet fever
- Linear, petechial appearance
- Most pronounced in the groin, underarm, and elbow creases (i.e., flexural areas)
Diagnostics
| Feature | Scarlet Fever | Acute Rheumatic Fever |
|---|
| Timing | Concurrent with active GAS infection | Delayed (2–4 weeks post-infection) |
| Pathophysiology | Toxin-mediated (SPEs) | Immune-mediated (molecular mimicry) |
| Rash | ”Sandpaper” texture, diffuse, punctate | Erythema marginatum (serpiginous, clear centers) |
| Key Finding | Strawberry tongue, Pastia’s lines | Migratory polyarthritis, carditis, chorea |
| Treatment Goal | Eradicate active infection, prevent ARF | Reduce inflammation, prevent recurrence with long-term prophylaxis |
Childhood exanthems
| Disease | Pathogen | Classic Presentation & Buzzwords |
|---|
| Measles | Measles virus | 4 C’s (Cough, Coryza, Conjunctivitis, Koplik spots).
Rash: Face → Body (Confluent).
Assoc: Vitamin A deficiency. |
| Rubella | Rubella virus | Post-auricular LAD.
Rash: Face → Body (spares 3 days, non-confluent).
Assoc: Congenital (PDA, cataracts, deaf), Adult arthritis. |
| Roseola | HHV-6 | High fever breaks → Rash appears.
Rash: Trunk → Face.
Assoc: Febrile seizures. |
| Fifth Disease | Parvovirus B19 | ”Slapped Cheek” → Lacy/Reticular body rash.
Assoc: Aplastic crisis (Sickle Cell), Hydrops fetalis. |
| Varicella | VZV | ”Dewdrop on a rose petal”.
Lesions in different stages of healing. t
Rash: Trunk → Extremities. |
| Scarlet Fever | Strep pyogenes | Sandpaper rash, Strawberry tongue, Circumoral pallor.
Assoc: Strep throat, Desquamation (palms/soles). |
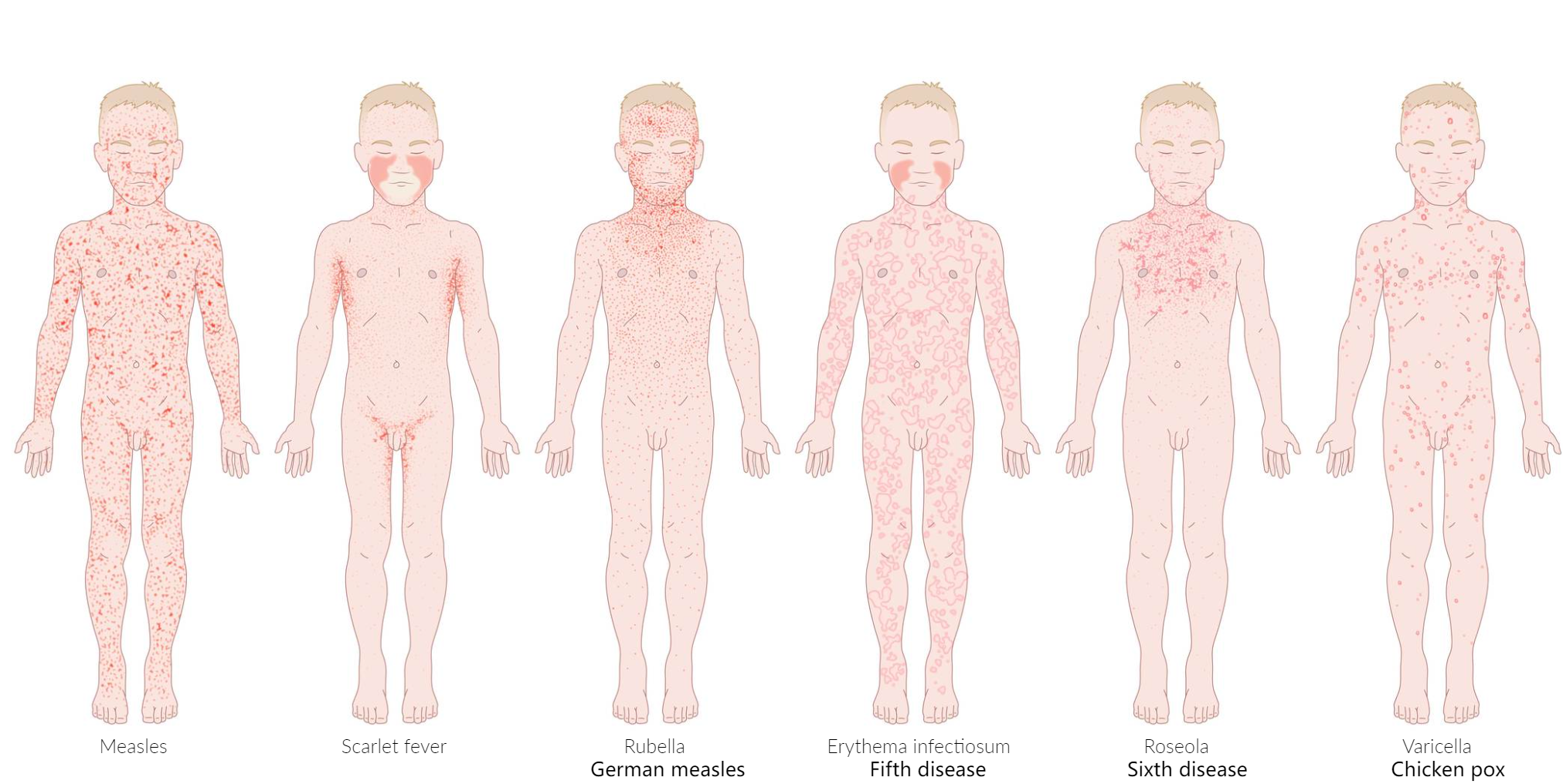
Fever-rash relationship
- Measles (Rubeola): Fever first (with cough, coryza, conjunctivitis) → Rash appears 3-5 days later, spreading from head to toe.
- Rubella (German Measles): Low-grade fever → Rash appears 1-2 days later, spreading quickly from head to toe.
- Scarlet Fever: Fever and sore throat begin together → “Sandpaper” rash appears 1-2 days later.
- Erythema Infectiosum (Fifth): Low-grade fever/prodrome resolves → “Slapped cheek” rash appears days later.
- Roseola Infantum (Sixth): High fever for 3-5 days → Fever breaks → Rash appears after the fever is gone.
- Varicella (Chickenpox): Fever and vesicular rash appear at the same time (lesions in various stages).
Link to original
Treatment
- Initiate one of the recommended antibiotic regimens for acute GAS pharyngitis, e.g.:
- Oral penicillin V or amoxicillin
- Nonsevere penicillin reaction: oral cephalosporins (e.g., cephalexin)
- Severe penicillin reaction: oral macrolides (e.g., azithromycin) or clindamycin


