Epidemiology
Etiology
- A myeloproliferative neoplasm characterized by the overproduction of all three hematopoietic cell lines, most prominently red blood cells (erythrocytosis).
- Caused by a mutation in the JAK2 gene (V617F substitution) in >95% of cases. This leads to constitutive activation of the JAK2 kinase, causing uncontrolled cell production independent of erythropoietin (EPO).
- The JAK2 (Janus kinase 2) oncogene codes for a non-receptor tyrosine kinase in hematopoietic progenitor cells. JAK2 is essential for the regulation of erythropoiesis, thrombopoiesis (megakaryopoiesis), and granulopoiesis.
Pathophysiology
Clinical features
- Typically presents in patients >60 years old.
- Symptoms are due to hyperviscosity and sludging of blood:
- Constitutional: Headache, dizziness, fatigue, vertigo, tinnitus, visual disturbances.
- Thrombosis: Major cause of morbidity/mortality. Can lead to MI, stroke, DVT/PE, or Budd-Chiari syndrome (hepatic vein thrombosis).
- Bleeding: Epistaxis, gum bleeding due to dysfunctional platelets.
- Pruritus: Classic aquagenic pruritus (intense itching after a warm bath/shower) due to histamine release from increased basophils.
- Also seen in Systemic mastocytosis
- Physical Exam:
- Plethora (ruddy complexion), splenomegaly (in ~75% of patients), hepatomegaly.
- Erythromelalgia: Severe burning pain and redness in hands/feet due to microvascular thrombi.
Diagnostics
- CBC: ↑ Hct (males >49%, females >48%), ↑ Hb (males >16.5 g/dL, females >16.0 g/dL), often with leukocytosis and thrombocytosis.
- JAK2 mutation analysis: Positive for V617F or exon 12 mutation.
- Serum EPO level: Suppressed/low. This is a key finding that differentiates it from secondary polycythemia.
- Bone Marrow Biopsy: Hypercellularity with panmyelosis (trilineage growth).
- WHO Diagnostic Criteria: Diagnosis requires either 3 major criteria, or the first 2 major and the 1 minor criterion.
- Major: 1) Elevated Hb/Hct, 2) Bone marrow hypercellularity, 3) Presence of JAK2 mutation.
- Minor: Subnormal serum EPO level.
Tip
Erythrocytosis associated with normal oxygen saturation and decreased serum EPO levels is strongly suggestive of polycythemia vera.
Differential diagnostics
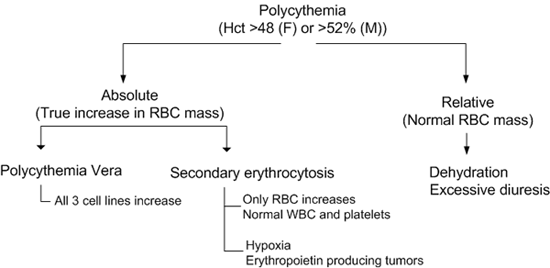
- Absolute versus relative erythrocytosis: Hemoglobin and hematocrit levels cannot accurately differentiate these conditions. Direct measurement of the RBC mass is necessary. An increased total RBC mass indicates an absolute erythrocytosis; a normal RBC mass indicates a relative erythrocytosis.
- Estimated using ⁵¹Cr-tagged red blood cell, similar to Mark and recapture method
- Primary versus secondary erythrocytosis: Serum erythropoietin levels can be used to differentiate primary from secondary erythrocytosis. Primary erythrocytosis is associated with low erythropoietin levels and is caused by myeloproliferative disorders such as polycythemia vera. Secondary erythrocytosis is characterized by increased erythropoietin levels due to chronic hypoxia from high altitudes, smoking, or chronic obstructive pulmonary disease; or abnormal secretion by neoplastic or otherwise diseased tissues.
- Hypoxic versus other causes of secondary erythrocytosis: Measurement of the arterial oxygen saturation (SaO2) is important to exclude hypoxemia as a cause of the erythrocytosis. SaO2 < 92% (PaO2 < 65 mm Hg) can cause secondary polycythemia. SaO2 (measured as a percentage) should not be confused with PaO2 (measured as a partial pressure in mm Hg).
Treatment
- Goal: Reduce thrombosis risk by keeping Hct <45%.
- First-line:
- Phlebotomy: Mainstay of treatment to reduce RBC mass.
- Low-dose Aspirin: Reduces risk of thrombosis.
- For high-risk patients (age >60 or history of thrombosis):
- Hydroxyurea: Myelosuppressive agent to lower cell counts.
- Ruxolitinib (JAK inhibitor): For patients intolerant or refractory to hydroxyurea.