Epidemiology
Etiology
Risk factors
- For contracting HPV infection
- Environmental risk factors
- Cigarette smoking and/or exposure to second-hand smoke (for squamous cell cancer types only)
- In-utero exposure to diethylstilbestrol (DES)
Pathophysiology
Overview of terminology
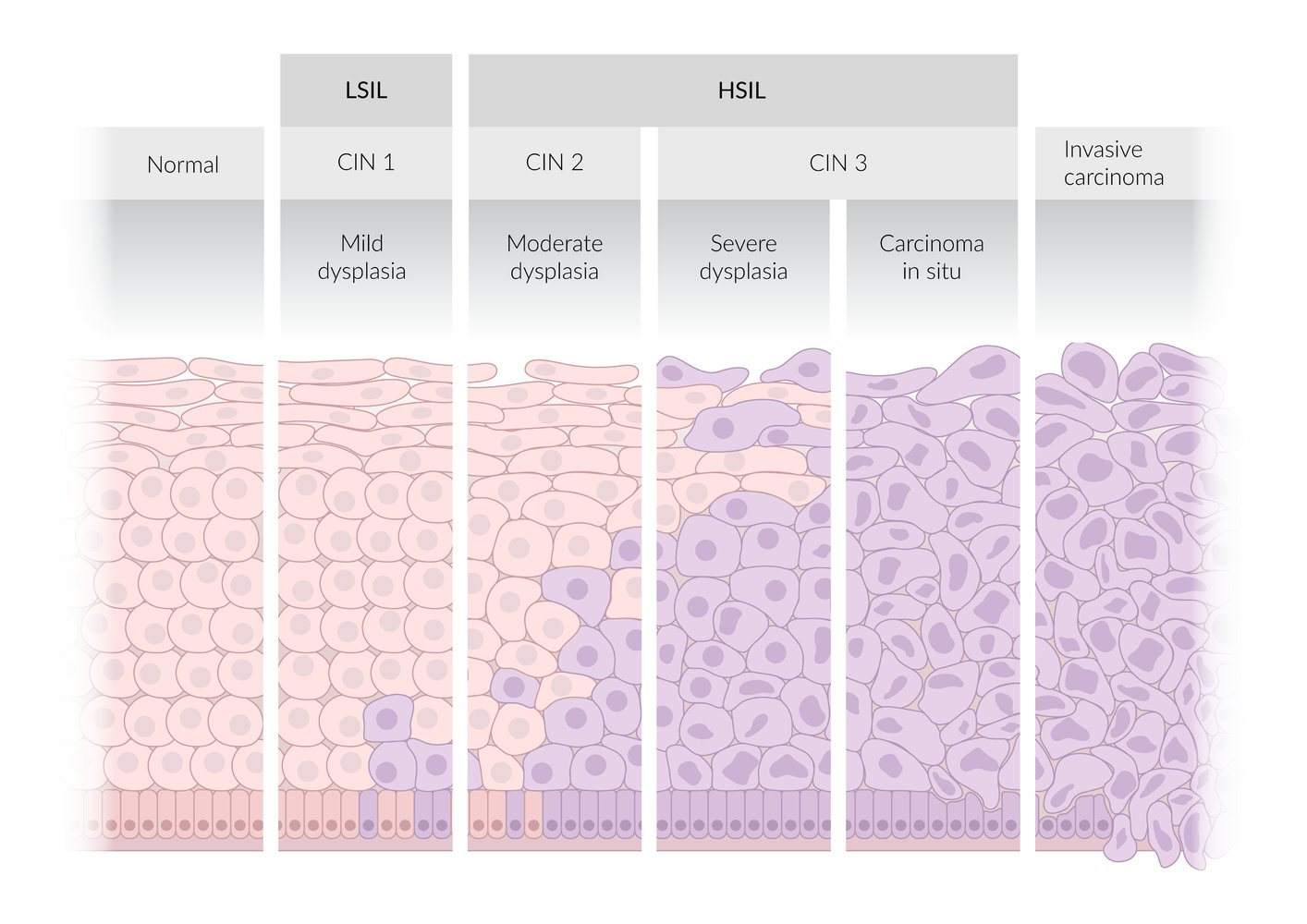
Two-tiered terminology (Bethesda system)
- High-grade squamous intraepithelial lesion (HSIL)
- Lesions with moderate to severe epithelial dysplasia that are most likely associated with persistent HPV infection
- HSIL lesions can progress to invasive cervical cancer (precancerous lesion).
- Low-grade squamous intraepithelial lesion (LSIL)
- Lesions with mild epithelial dysplasia that are typically associated with transient HPV infections
- Correlates with CIN1
Three-tiered terminology
- Cervical intraepithelial neoplasia (CIN) is characterized by epithelial dysplasia that begins at the basal layer of the squamocolumnar junction and extends outward.
- Based on the degree of dysplasia, lesions are classified as CIN1 (mild), CIN2 (moderate), or CIN3 (severe).
Current standard
The current standard for reporting cervical histopathology and cytopathology to ensure optimal management is a combination of the two-tier and three-tier system (i.e., the two-tiered nomenclature with an additional qualifier using the intraepithelial neoplasia nomenclature).
- LSIL correlates with CIN1.
- HSIL correlates with CIN3 and CIN2.
- HSIL should be specified as HSIL (CIN2), HSIL (CIN3), or HSIL unspecified.
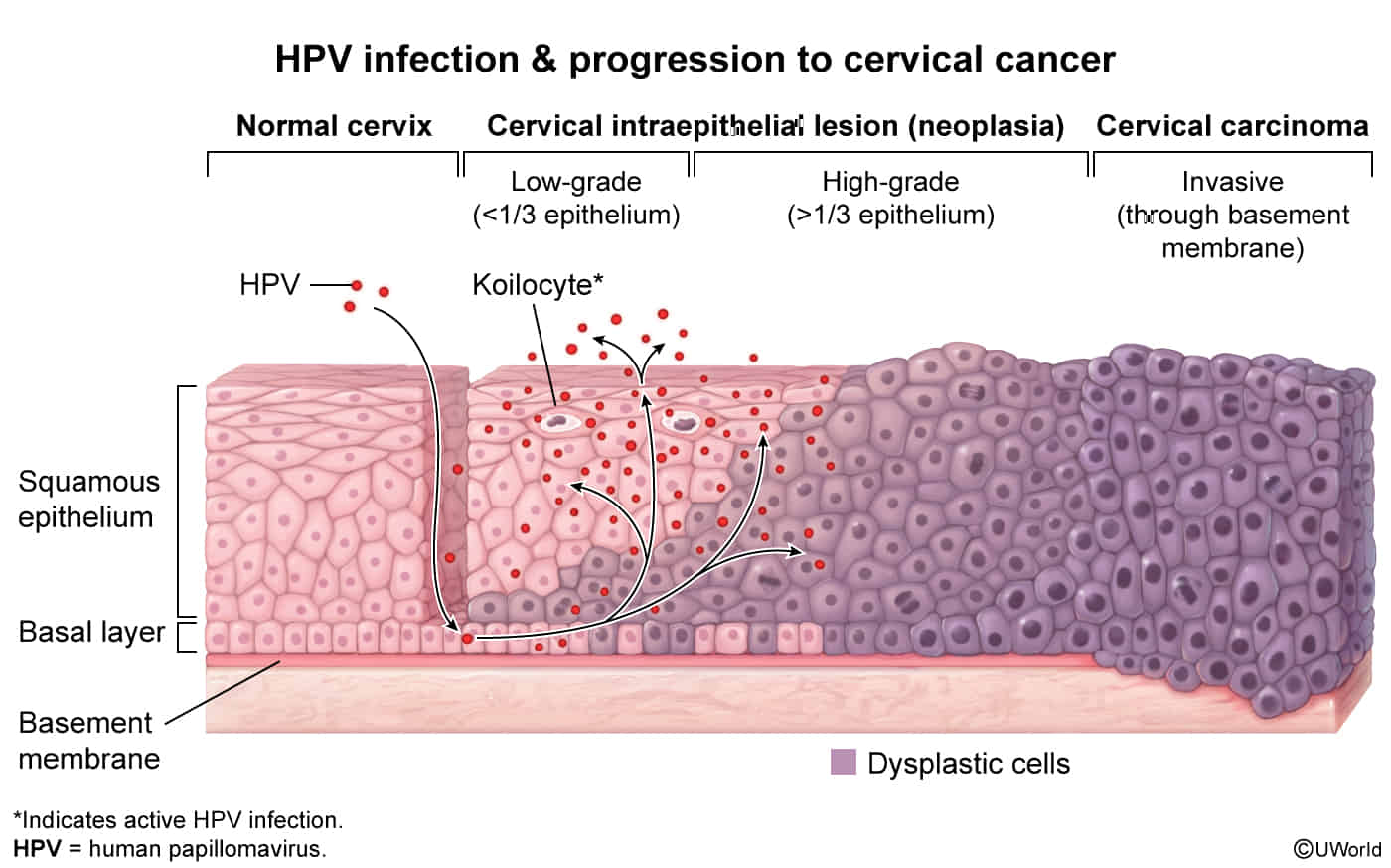
Normal cervix
- Ectocervix: Lined by non-keratinized stratified squamous epithelium, continuous with the vaginal epithelium.
- Endocervix: Lined by simple columnar epithelium, which is mucus-secreting.
- Squamocolumnar Junction (SCJ): The sharp boundary where the squamous and columnar epithelia meet.
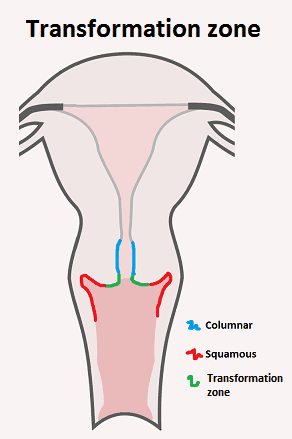
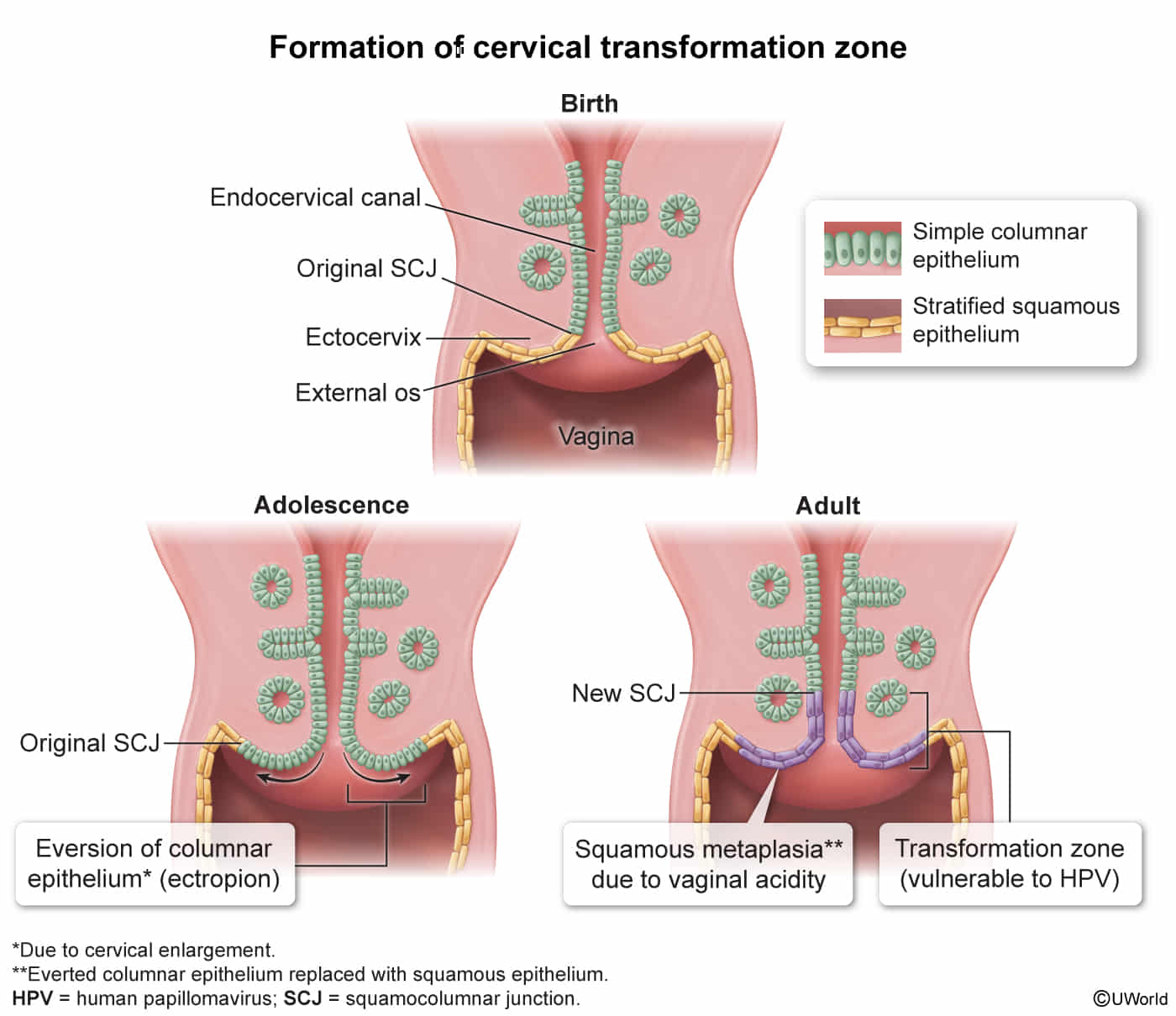
- Transformation Zone (TZ):
- A dynamic area on the ectocervix where columnar epithelium (ectropion) is gradually replaced by squamous epithelium through squamous metaplasia.
- This process is hormonally influenced and most active during puberty and first pregnancy.
- The TZ is the most common site for HPV infection and subsequent cervical dysplasia (CIN) and carcinoma.
- This is the critical area to sample during a Pap smear.
Clinical features
Diagnostics
Differential diagnostics
| Feature | Cervical Cancer | Endometrial Cancer |
|---|---|---|
| Pathophysiology | HPV 16, 18 (E6 inhibits p53, E7 inhibits Rb). Arises at the transformation zone. | Unopposed estrogen leads to endometrial hyperplasia. |
| Classic Patient | Younger, multiple sexual partners, smoker, immunosuppressed (HIV). | Older, obese, nulliparous, diabetic. Postmenopausal. |
| Key Presentation | Postcoital bleeding. Often asymptomatic until advanced. | Postmenopausal bleeding. |
| Screening | Pap test +/- HPV co-testing. | None for asymptomatic women. |
| Diagnosis | Colposcopy with directed biopsy. | Endometrial biopsy. TVUS shows thickened stripe (>4mm). |
| Histology | Squamous Cell Carcinoma (most common). | Endometrioid adenocarcinoma (most common). |
| Major Risk Factors | - Multiple sexual partners - Immunosuppression - Smoking | - Obesity - Nulliparity - Unopposed estrogen therapy - Tamoxifen |
| Primary Treatment | Hysterectomy or chemoradiation (stage-dependent). | Total Hysterectomy + BSO. |
| Prevention | HPV vaccine. | Progestins (in combined OCPs/HRT), weight control. |
Pathology
- Invasive cervical carcinoma is characterized by invasion of the tumor beyond the basement membrane of the cervical epithelium.
- HSIL and invasive cervical carcinoma most commonly arise from metaplastic squamous cell epithelium in the cervical transformation zone
Squamous cell carcinoma (∼ 80% of cases)
- Subtypes include large cell keratinizing, large cell nonkeratinizing, and papillary squamous cell carcinoma.
- Irregular cell morphology
- Hyperchromatic cells with nonspherical nuclei, mitotic activity, and prominent nucleoli
- Loss of basal membrane
Tip
- Staging (Simplified FIGO)
- Stage I: Confined strictly to the cervix.
- Stage II: Invades beyond the uterus, but not to the pelvic wall or lower third of the vagina.
- Stage IIB is clinically important as it involves parametrial invasion.
- Stage III: Tumor extends to the pelvic wall, and/or involves the lower third of the vagina, and/or causes hydronephrosis.
- Stage IV: Extends beyond the true pelvis or involves mucosa of bladder/rectum (IVA) or has distant metastases (IVB).
Treatment
Pre-Invasive (CIN / HSIL)
- CIN 1: Observe (most regress).
- CIN 2, 3 (HSIL): Excisional procedures are standard.
- Loop Electrosurgical Excision Procedure (LEEP): Most common method.
- An electrically heated wire loop removes the transformation zone and lesion. Provides a tissue specimen for histology to rule out invasive cancer.
- Cold Knife Conization (CKC): If lesion extends into endocervical canal or for adenocarcinoma in situ (AIS).
- Loop Electrosurgical Excision Procedure (LEEP): Most common method.
Early-Stage Invasive Cancer (FIGO Stage IA - IIA1)
- Stage IA1: Cone biopsy or simple hysterectomy.
- Stage IA2 - IIA1 (< 4cm):
- Option 1: Radical hysterectomy + pelvic lymph node dissection (LND).
- Option 2: Primary chemoradiation (equally effective).
- Fertility Sparing (select cases): Radical trachelectomy + LND.
Locally Advanced Cancer (FIGO Stage IB2 - IVA)
- Standard of Care: Definitive chemoradiation.
- External beam radiation (EBRT) + brachytherapy.
- Concurrent cisplatin-based chemotherapy (radiosensitizer).
- Surgery is NOT the primary treatment.
- Due to high rates of positive margins and nodal metastasis.
Metastatic (Stage IVB) or Recurrent Disease
- Goal: Palliative.
- Treatment: Systemic therapy.
- First Line: Carboplatin + Paclitaxel +/- Bevacizumab (anti-VEGF).
- Immunotherapy: Add Pembrolizumab (anti-PD-1) for PD-L1 positive tumors.