Epidemiology
Etiology
Pathophysiology
Clinical features
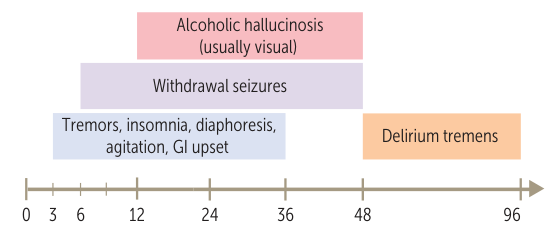
- Timeline is key for predicting severity and type of symptoms:
- 6-24 hours: Minor withdrawal. Symptoms include anxiety, insomnia, tremors, diaphoresis, palpitations, headache, and GI upset.
- 12-48 hours: Withdrawal seizures. Typically generalized tonic-clonic. Hallucinations (visual, auditory, or tactile) can also occur.
- 48-96 hours: Delirium Tremens (DT). A medical emergency. Hallmarked by disorientation and global confusion. Also includes severe agitation, hallucinations, fever, HTN, tachycardia, and diaphoresis. Mortality can be up to 5% even with treatment.
Similar features like serotonin syndrome, but without neuromuscular findings (especially prominent clonus and lower limb rigidity/hyperreflexia)
Diagnostics
Treatment
- First-line: benzodiazepines
- Shorter or intermediate-acting (e.g., oxazepam, lorazepam): Consider in patients with a slow metabolism (e.g., the elderly, those with liver failure).
- Longer acting (e.g., chlordiazepoxide, diazepam): preferred in all other patients
Mnemonic
Alcohol, barbiturates, and benzodiazepines all enhance GABA receptors, so their withdrawal syndromes share similar symptoms (seizures, tachycardia, and tremors).