Cutaneous mycoses are fungal infections of the keratinized tissues of the body: the skin, hair, and nails. They are broadly divided into dermatophytoses and infections caused by other fungi like Malassezia or Candida spp.
Dermatophytoses (Tinea/Ringworm)
- Patho/Etiology: Caused by dermatophytes (molds) classified into three genera: Trichophyton, Epidermophyton, and Microsporum. These fungi infect and digest keratin. Transmission can be human-to-human, animal-to-human, or soil-to-human.
- Clinical Presentation: Manifestations are named based on the affected body site (“tinea” + location).
- Tinea corporis (body): Presents as an pruritic, erythematous, annular (ring-shaped) lesion with a raised, scaly border and central clearing. Often seen in wrestlers.
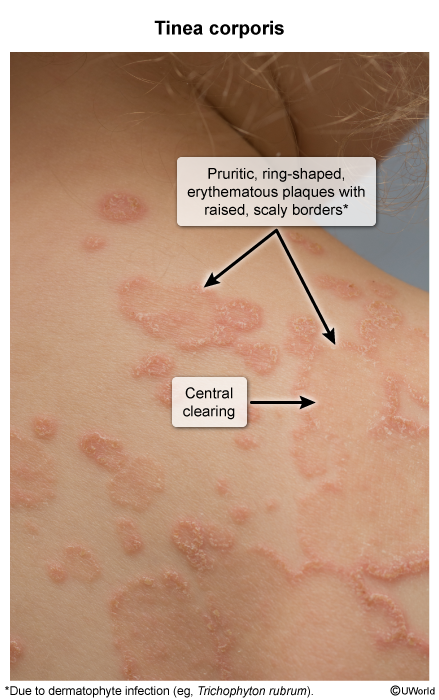
- Tinea pedis (foot; “Athlete’s Foot”): Typically involves interdigital spaces (maceration, scaling) or a “moccasin” distribution with scaling on the soles.
- Tinea cruris (groin; “Jock Itch”): Erythematous, scaly rash on the upper inner thighs and groin; typically spares the scrotum.
- Tinea capitis (scalp): Common in children, presenting with scaling, alopecia (hair loss), and often posterior cervical or occipital lymphadenopathy.
- Tinea unguium (nail; Onychomycosis): Results in thickened, discolored, and brittle nails.
- Tinea corporis (body): Presents as an pruritic, erythematous, annular (ring-shaped) lesion with a raised, scaly border and central clearing. Often seen in wrestlers.
- Dx:
- KOH preparation of skin or nail scrapings reveals septate hyphae.
- Wood’s lamp: Some Microsporum species may fluoresce.
- Mgmt:
- Topical antifungals (e.g., azoles like clotrimazole, terbinafine) are first-line for most tinea infections (corporis, cruris, pedis). t
- Oral/systemic therapy (e.g., terbinafine, griseofulvin) is required for tinea capitis and onychomycosis.
Pityriasis Versicolor (Tinea Versicolor)
Tip
Pityriasis Versicolor isn’t a true “tinea” infection, because
- Different Organism: Pityriasis versicolor is caused by Malassezia (a yeast), whereas true tinea is caused by dermatophytes (molds).
- Normal Flora vs. Pathogen: It’s an overgrowth of normal skin flora (Malassezia), not an infection by an external pathogen like dermatophytes.
- Not Contagious: Since the yeast is already part of everyone’s skin microbiome, the condition is not contagious. True tinea infections are contagious.
- Patho/Etiology: Not a true dermatophyte infection. Caused by the overgrowth of Malassezia spp. (e.g., M. furfur), a dimorphic fungus that is a normal component of skin flora. It’s more common in hot, humid weather. The fungus produces azelaic acid, which inhibits tyrosinase, leading to altered skin pigmentation.
- Clinical Presentation: Multiple, well-demarcated, hypo- or hyperpigmented macules, most often on the trunk and upper arms. Lesions have a fine scale and are typically asymptomatic, though mild pruritus can occur. The hypopigmented patches become more apparent after sun exposure as the affected skin does not tan.
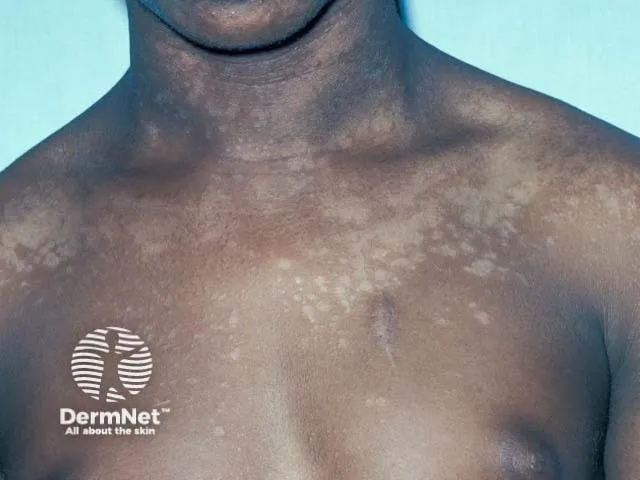
- Dx:
- KOH preparation shows a classic “spaghetti and meatballs” appearance, representing hyphae and yeast cells.
- Wood’s lamp examination may show a yellow-green fluorescence.
- Mgmt:
- Topical agents are first-line, including selenium sulfide shampoo or topical antifungals (e.g., ketoconazole).
- Oral antifungals (e.g., fluconazole, itraconazole) are used for widespread or recurrent cases. Recurrence is common.
Cutaneous Candidiasis
- Patho/Etiology: Infection with Candida species, most commonly C. albicans, which is part of the normal flora. It is an opportunistic pathogen, with overgrowth favored by heat, moisture, and immunosuppression (e.g., diabetes, steroid use).
- Clinical Presentation:
- Intertrigo: Occurs in moist skin folds (axillae, groin, under breasts), presenting as erythematous, macerated plaques with characteristic satellite lesions (pustules or papules).
- Diaper dermatitis: A common cause of diaper rash.
- Chronic Mucocutaneous Candidiasis (CMC): A rare immunodeficiency disorder characterized by persistent noninvasive Candida infections of the skin, nails, and mucous membranes due to T-cell dysfunction.
- Dx:
- Clinical appearance is often sufficient.
- KOH preparation reveals budding yeasts and pseudohyphae.
- Mgmt:
- Keep area dry and use topical antifungals (e.g., nystatin, clotrimazole).
- Oral fluconazole may be used for extensive or resistant cases.