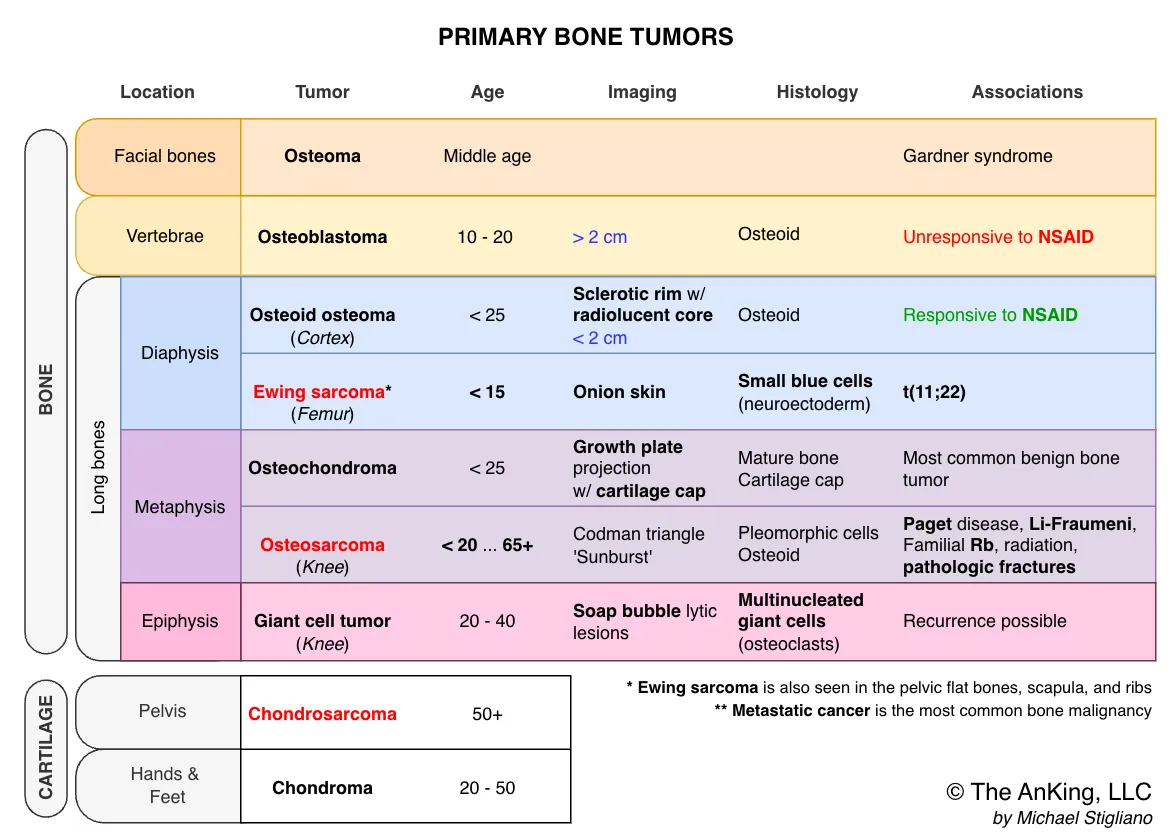
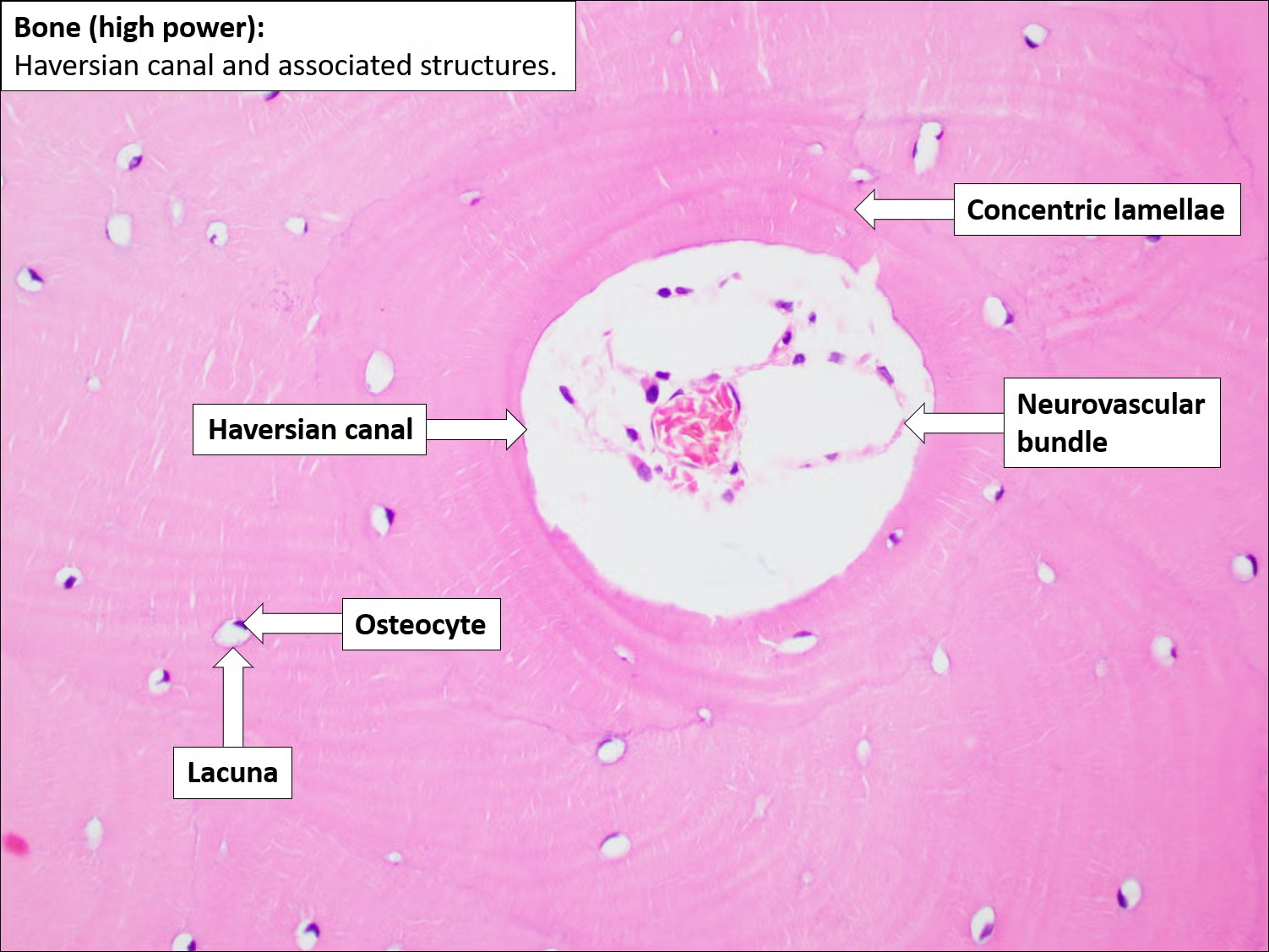
- Normal bone histology
Benign Bone Tumors
- Osteoma
- Patho/Etiology: A benign, slow-growing tumor composed of mature, normal-appearing compact bone.
- Clinical Presentation: Most commonly found in middle-aged adults. Typically presents as a solitary, asymptomatic lesion on the surface of facial bones or the skull (especially the frontal sinus).
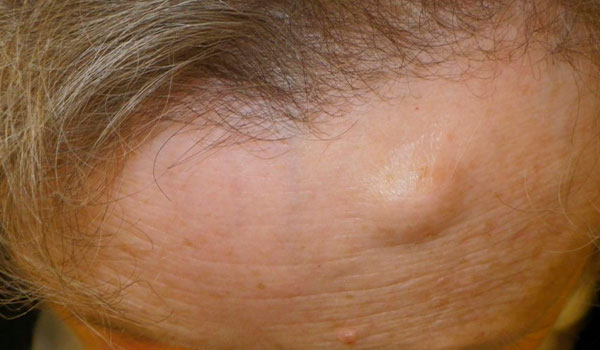
- Dx: X-ray shows a sharply circumscribed, round, radiodense (sclerotic) mass.
- Mgmt: Asymptomatic lesions do not require treatment. Surgical excision is reserved for cases causing cosmetic issues or symptoms (e.g., sinus obstruction).
- Key Associations: The presence of multiple osteomas should raise strong suspicion for Gardner syndrome, a subtype of Familial Adenomatous Polyposis (FAP). This syndrome is characterized by:
- Multiple osteomas (especially in the skull, sinuses, and mandible)
- Thousands of colonic polyps (100% risk of progressing to colorectal cancer)
- Soft tissue tumors (e.g., epidermoid cysts, fibromas) and supernumerary teeth.
- Osteoblastoma
- Patho/Etiology: A benign, osteoid-producing tumor that is histologically similar to an osteoid osteoma but larger and more aggressive.
- Pain is due to compression of large tumor to nerves, thus it’s not responsive to NSAIDs.
- Clinical Presentation: Primarily affects males under 30. It commonly involves the posterior elements of the spine (vertebrae). The pain is typically a dull ache that is not relieved by NSAIDs.
- Dx: X-ray or CT shows a radiolucent nidus that is larger than 2 cm. It typically has less surrounding reactive sclerosis compared to an osteoid osteoma.
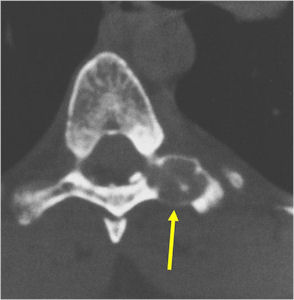
- Mgmt: Due to its size and tendency to be locally aggressive, the standard treatment is surgical resection or curettage.
- Key Differentiating Factor: The key way to distinguish it from an osteoid osteoma is its size (>2 cm), location (often spine), and pain that is unresponsive to NSAIDs.
- Patho/Etiology: A benign, osteoid-producing tumor that is histologically similar to an osteoid osteoma but larger and more aggressive.
- Osteoid Osteoma
- Patho/Etiology: Benign tumor derived from osteoblasts that produces a small, radiolucent nidus.
- Pain is due to high levels of prostaglandins E2 produced by small tumor cells, thus it’s responsive to NSAIDs.
- Clinical Presentation: Affects males < 25 years old. Characterized by nocturnal bone pain that is relieved by NSAIDs.
- Dx: X-ray shows a small (<1.5-2 cm) radiolucent nidus surrounded by a rim of reactive bone, often in the cortex of long bones like the femur or tibia.
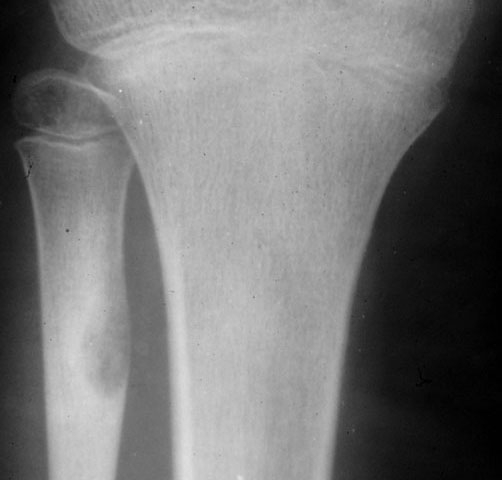
- Patho/Etiology: Benign tumor derived from osteoblasts that produces a small, radiolucent nidus.
- Osteochondroma
- Patho/Etiology: Most common benign bone tumor, characterized by a cartilage-capped bony projection arising from the external surface of a bone. It’s an outgrowth of the growth plate.
- Clinical Presentation: Most common in males < 25 years old. Usually found incidentally or as a painless mass near the metaphysis of long bones, especially the knee.
- Dx: X-ray shows a pedunculated or sessile growth pointing away from the joint.
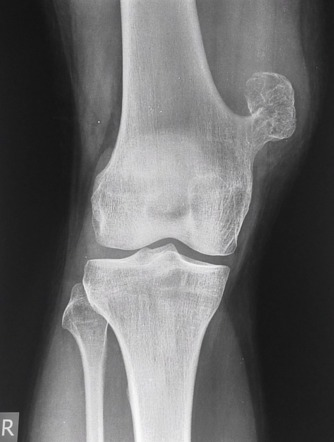
- Key Associations: Can rarely transform into chondrosarcoma.
- Giant Cell Tumor (Osteoclastoma)
- Patho/Etiology: Locally aggressive tumor containing multinucleated giant cells resembling osteoclasts.
- Clinical Presentation: Typically affects individuals 20-40 years old. Presents with pain and swelling, commonly around the knee.
- Dx: X-ray reveals a “soap bubble” appearance (lytic lesion) in the epiphysis of long bones.
- Mgmt: Surgical resection (curettage) is the standard treatment.
- Enchondroma
- Patho/Etiology: Benign cartilaginous tumor located in the medullary cavity of a bone.
- Clinical Presentation: Often found in patients aged 10-20. Commonly located in the small bones of the hands and feet.
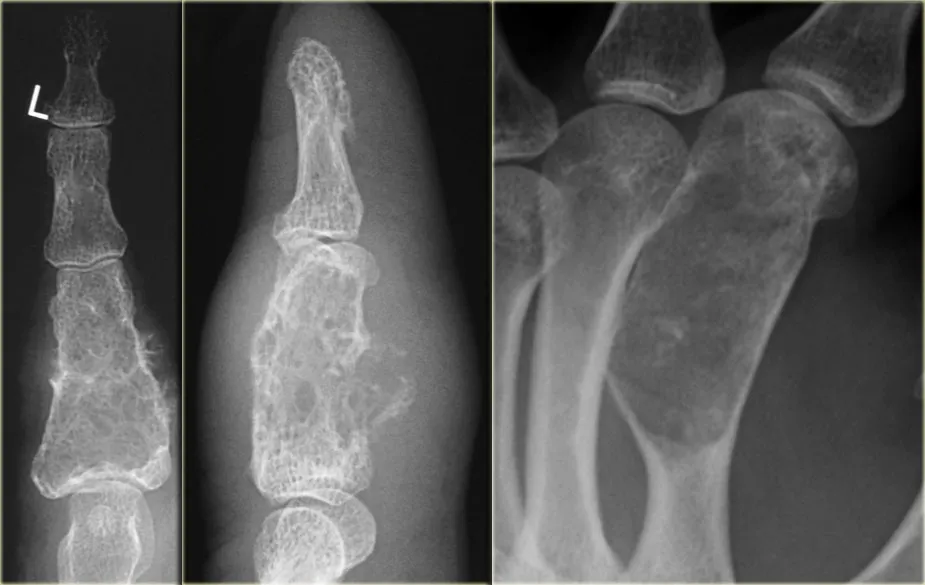
- Key Associations: Multiple enchondromas are seen in Ollier disease and Maffucci syndrome.
Malignant Bone Tumors
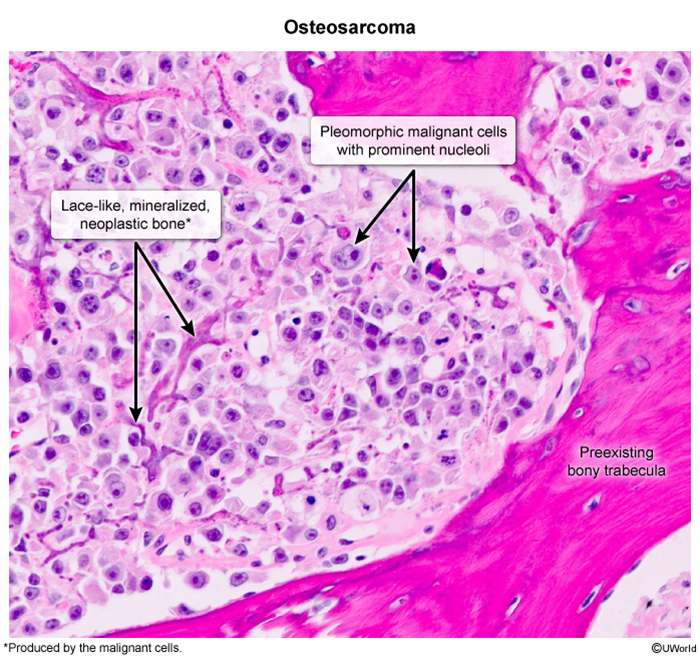
- Osteosarcoma
- Patho/Etiology: The most common primary malignant bone tumor, characterized by the production of osteoid (immature bone) by malignant cells.
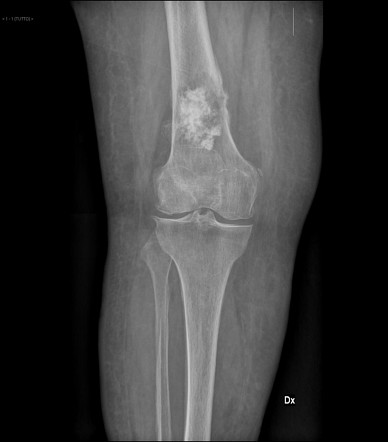
- Clinical Presentation: Bimodal age distribution, with a peak in adolescents (10-25 years) and another in older adults, often secondary to conditions like Paget disease. Presents with pain and a palpable mass, commonly in the metaphysis of long bones around the knee (distal femur, proximal tibia).
- Dx: X-ray findings include a “sunburst” pattern (periosteal reaction) and Codman’s triangle (lifting of the periosteum). Histology shows pleomorphic malignant cells producing osteoid.
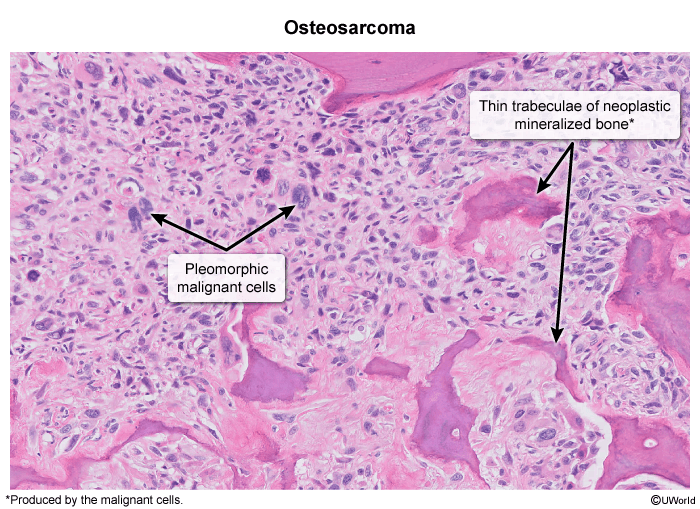
- Key Associations: Associated with mutations in RB1 (retinoblastoma) and TP53 (Li-Fraumeni syndrome).
- Mgmt: Treatment involves neoadjuvant chemotherapy followed by surgery and adjuvant chemotherapy.
- Ewing Sarcoma
- Patho/Etiology: An aggressive small blue cell tumor.
- Clinical Presentation: Primarily affects children and young adults, typically under 15 years old, with a predilection for Caucasian males. Can present with systemic symptoms like fever and weight loss, mimicking an infection.
- Dx: Found in the diaphysis of long bones (like the femur), pelvis, and scapula. X-ray classically shows an “onion skin” periosteal reaction. Histology reveals small, round, blue cells.
- Key Associations: Associated with a characteristic t(11;22) translocation.
- Mgmt: Requires a combination of chemotherapy, surgery, and/or radiation.
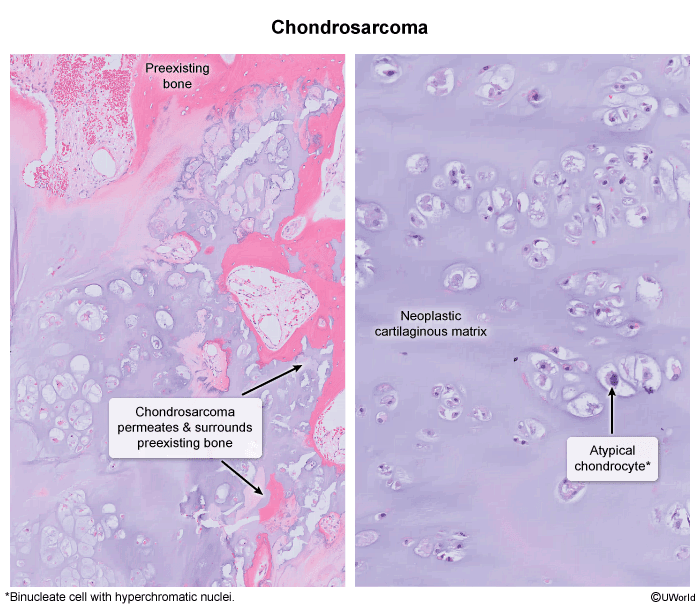
- Chondrosarcoma
- Patho/Etiology: A malignant tumor of cartilage-producing cells.
- Clinical Presentation: Typically seen in older adults (30-60 years). Commonly arises in the central skeleton, including the pelvis, ribs, and proximal long bones.
- Dx: X-ray may show a mass with “popcorn” or “ring and arc” calcifications within the medullary cavity.
- Mgmt: Tends to be resistant to chemotherapy and radiation; wide surgical excision is the primary treatment.
Bone Cysts and Cyst-like Lesions
-
Unicameral (Simple) Bone Cyst (UBC)
- Patho/Etiology: A true, fluid-filled cyst with a thin fibrous lining. It is considered a developmental lesion, not a true neoplasm.
- Clinical Presentation: Most common in children and adolescents (ages 5-15). Usually asymptomatic until a pathologic fracture occurs. Classic location is the metaphysis of long bones, especially the proximal humerus and proximal femur.
- Dx: X-ray shows a central, well-defined lytic lesion that spans the entire diameter of the bone. A pathognomonic finding after a fracture is the “fallen leaf” sign, where a bone fragment floats to the bottom of the fluid-filled cyst.
- Mgmt: Often managed with observation. For persistent or symptomatic cysts (especially after fracture), treatment involves aspiration and injection of corticosteroids or curettage with bone grafting.
-
Aneurysmal Bone Cyst (ABC)
- Patho/Etiology: A benign but rapidly growing, destructive lesion composed of blood-filled spaces. It is associated with a specific gene translocation (USP6). Can arise de novo or secondary to another bone tumor.
- Clinical Presentation: Typically affects adolescents and young adults (ages 10-20). Presents with pain and swelling. Commonly located in the metaphysis of long bones or the posterior elements of the spine.
- Dx: X-ray shows an eccentric (off-center), expansile, lytic “soap bubble” lesion with a thin shell of reactive bone. MRI or CT is key and will demonstrate fluid-fluid levels from layering of red blood cells.
- Mgmt: Treatment requires surgical intervention, typically curettage and bone grafting.
-
Fibrous Dysplasia
- Patho/Etiology: A developmental defect in which normal bone is replaced by immature, disorganized fibro-osseous tissue due to a GNAS gene mutation.
- Clinical Presentation: Can be monostotic (affecting one bone) or polyostotic (multiple bones). Pain, swelling, or pathologic fracture are common presentations.
- Dx: X-ray shows a hazy, “ground-glass” lytic lesion with poorly defined borders. A severe bowing deformity of the proximal femur, known as a “shepherd’s crook” deformity, is classic.
- Key Associations: The polyostotic form is a key component of McCune-Albright Syndrome, defined by the triad of:
- Polyostotic fibrous dysplasia
- Café-au-lait spots (with irregular, “coast of Maine” borders)
- Precocious puberty or other endocrinopathies.