See also Lipid-lowering agents
Key Points
- TG
- Energy reserve
- Synthesized in liver and adipocytes
- Stored in adipocytes
- Cholesterol
- Incorporated in all cell membranes in the lipid bilayer: increases membrane fluidity and stability
- Precursor for synthesis of:
- Steroid hormones (e.g., androgens, estrogens, mineralocorticoids, glucocorticoids)
- Bile acids
- Vitamin D
- Transport in blood via lipoproteins
- From the intestine to the liver: together with TAGs in chylomicrons
- From the liver to peripheral tissues: via VLDL and LDL
- From peripheral tissues to the liver (reverse cholesterol transport): via HDL and IDL
- HDL
- Transport cholesterol from peripheral tissues (e.g., atherosclerotic arteries) to the liver (reverse cholesterol transport), where it is excreted (e.g., via bile)
- LDL
- Transport cholesterol from the liver to peripheral tissues and arteries
- VLDL
- Transport hepatic triglycerides from the liver to peripheral tissues
- Chylomicron
- Secreted by the intestinal epithelial cells into lymphatics
- Transport dietary triglycerides from the intestine to peripheral tissues
Lipoproteins (HDL, VLDL, LDL)
- Protein is denser than fat.
- Therefore, the higher the ratio of protein to fat, the higher the density of the lipoprotein particle.
- VLDL: ~0.98 g/mL (high TG, to adipocytes)
- IDL: ~1.0 g/mL (“intermediate” means an intermediate step between VLDL and LDL, not intermediate density)
- LDL: ~1.04 g/mL (high cholesterol, to peripheral cells)
- HDL: ~1.12 g/mL
I. Lipid Synthesis
This primarily occurs in the liver in the well-fed state (stimulated by insulin).
A. Fatty Acid Synthesis
- Location: Cytoplasm.
- Substrate: Acetyl-CoA (transported from mitochondria via the citrate shuttle).
- Rate-Limiting Enzyme: Acetyl-CoA Carboxylase (ACC). It converts acetyl-CoA to malonyl-CoA and requires biotin (vitamin B7).
- Activation: Insulin, Citrate.
- Inhibition: Glucagon, Palmitoyl-CoA.
- Key Enzyme Complex: Fatty Acid Synthase. It uses malonyl-CoA and requires NADPH to produce palmitate (a 16-carbon fatty acid).
B. Cholesterol Synthesis
- Location: Cytoplasm and smooth endoplasmic reticulum.
- Substrate: Acetyl-CoA.
- Rate-Limiting Enzyme: HMG-CoA Reductase. It converts HMG-CoA to mevalonate.
- Inhibition: High cholesterol levels, Glucagon. Statins are competitive inhibitors of this enzyme.
- Activation: Insulin.
II. Lipid Transport via Lipoproteins
Lipids are transported in the blood as lipoproteins, which consist of a lipid core and an outer shell of apolipoproteins and phospholipids.
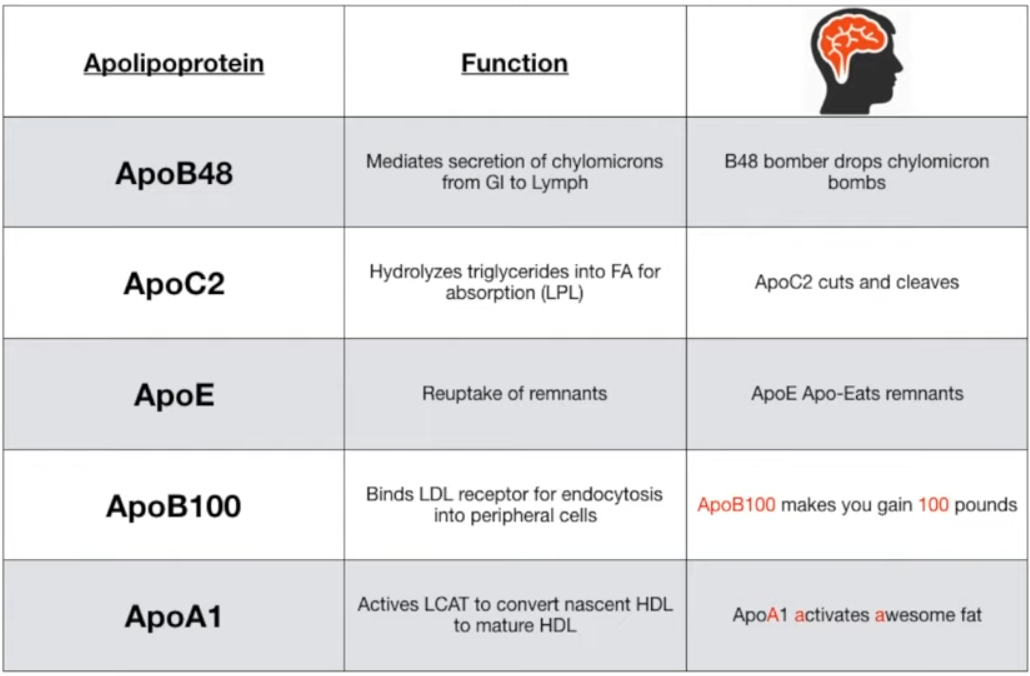
Key Apolipoproteins
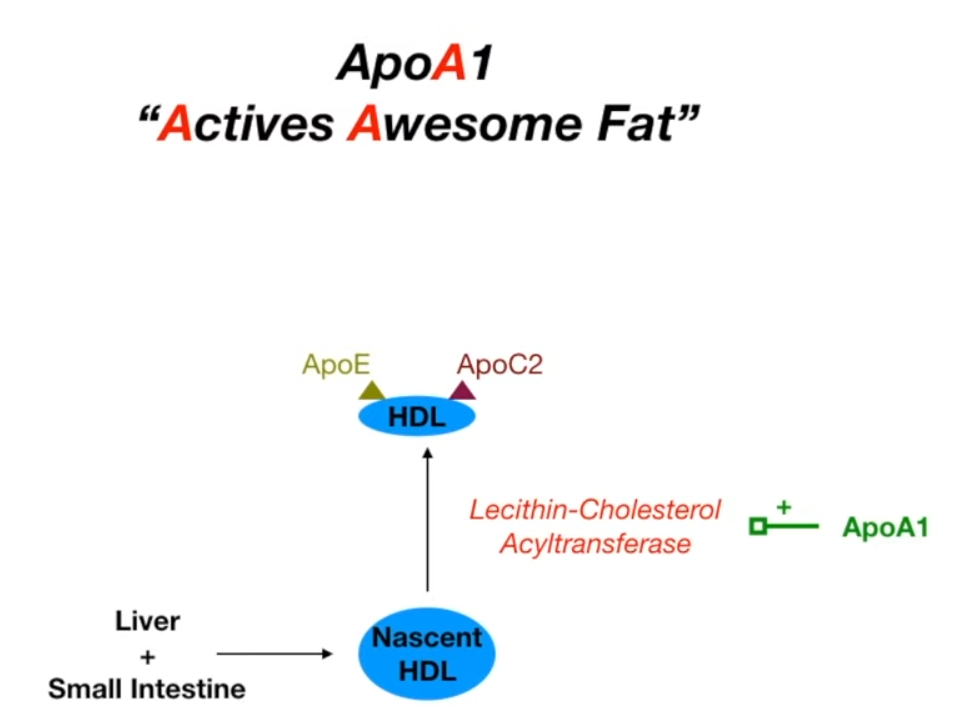
- ApoA-I: Activates LCAT for HDL maturation. Found on HDL.
- ApoB-48: Mediates chylomicron secretion from enterocytes.
- ApoB-100: Binds to the LDL receptor for uptake. Found on VLDL, IDL, and LDL.
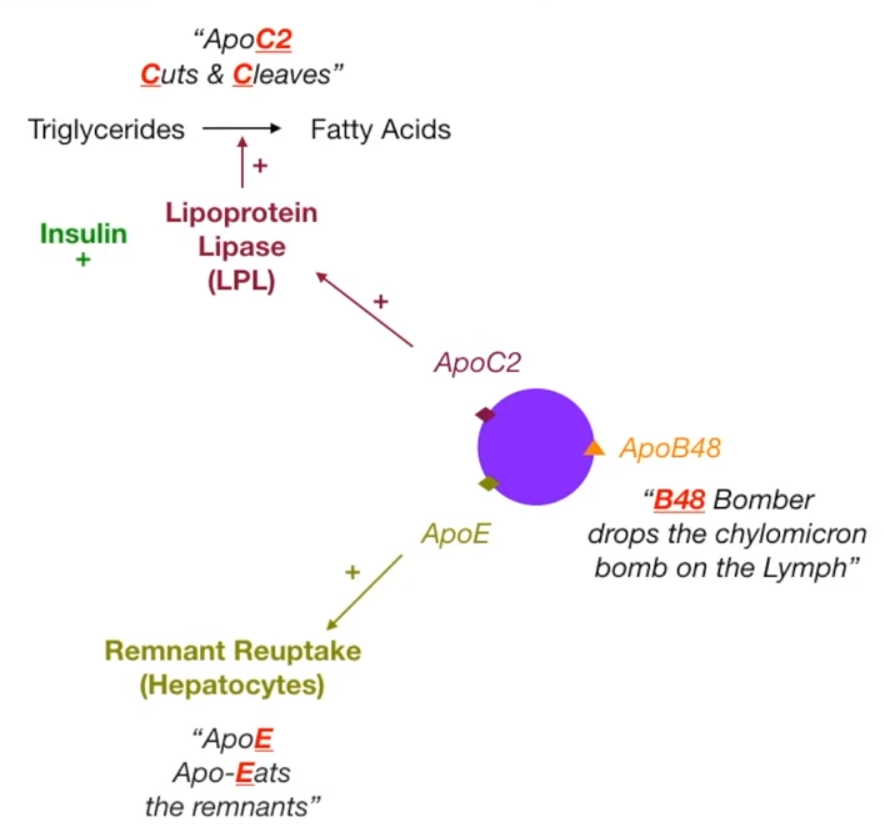
- ApoC-II: Activates lipoprotein lipase (LPL) to break down triglycerides.
- ApoE: Mediates remnant uptake by the liver.
Transport Pathways
Drawing 2025-06-21 09.29.42.excalidraw
⚠ Switch to EXCALIDRAW VIEW in the MORE OPTIONS menu of this document. ⚠ You can decompress Drawing data with the command palette: ‘Decompress current Excalidraw file’. For more info check in plugin settings under ‘Saving’
Excalidraw Data
Text Elements
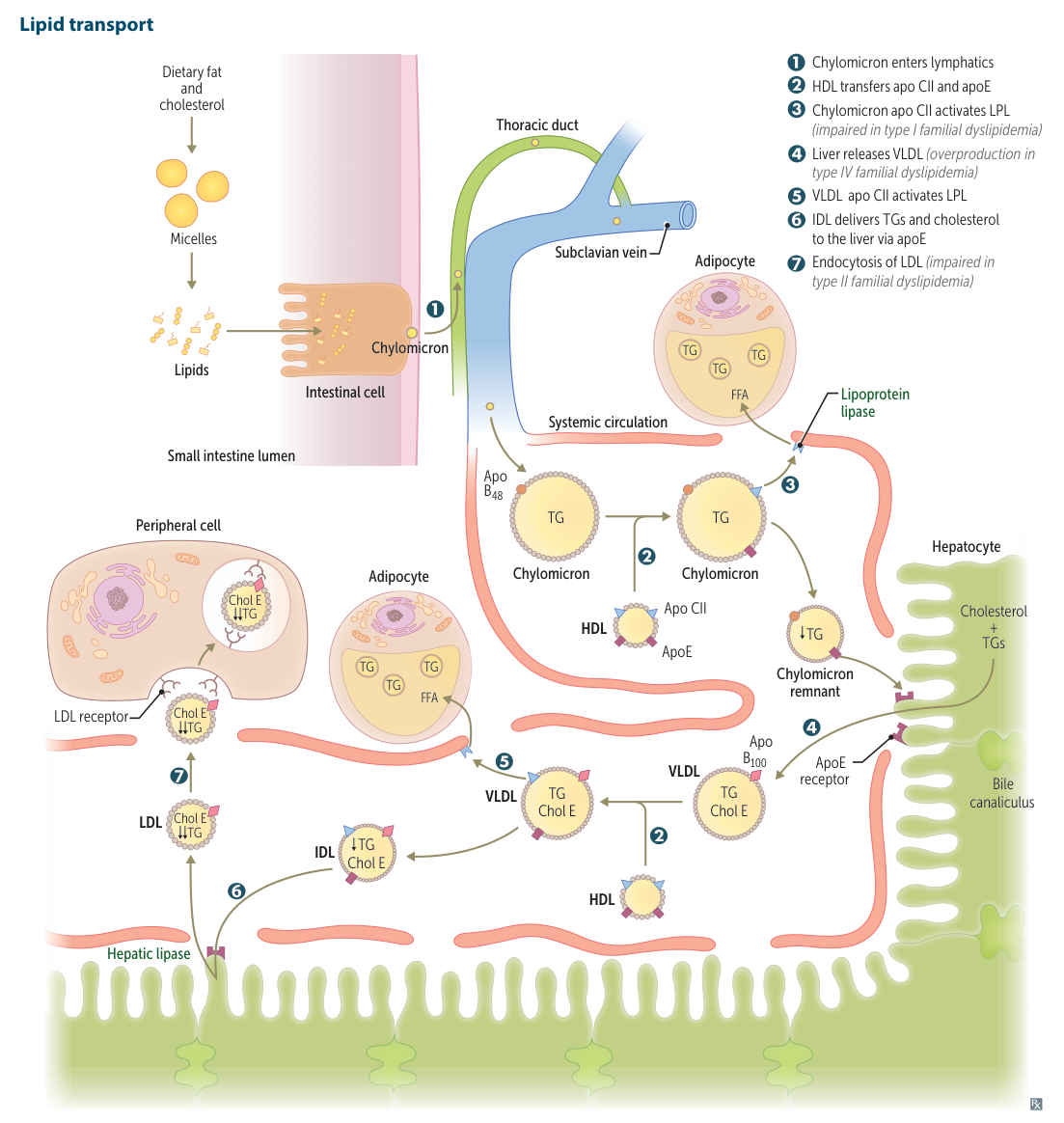
Exogenous Pathway: Transport of Dietary Lipids
Endogenous Pathway: Transport of Endogenously Synthesized Lipids
Embedded Files
0323f0f6001370e0d5340304ddada336d6c196b3: Pasted Image 20250621093052_384.png
Link to original
-
Exogenous Pathway (Dietary Fat)
- Chylomicrons are created in the intestine (containing ApoB-48) to transport dietary triglycerides.
- In the blood, they acquire ApoC-II and ApoE from HDL.
- Lipoprotein Lipase (LPL), activated by ApoC-II, cleaves triglycerides, releasing fatty acids to peripheral tissues.
- Chylomicron remnants (rich in cholesterol) are cleared by the liver via ApoE. t
-
Endogenous Pathway (Liver-Synthesized Fat)
- VLDL is created in the liver (containing ApoB-100) to transport endogenous triglycerides.
- LPL degrades triglycerides in VLDL, forming IDL (VLDL remnant).
- IDL can be cleared by the liver or further processed by hepatic lipase into LDL.
- LDL (“bad cholesterol”) delivers cholesterol to peripheral tissues via LDL receptors that recognize ApoB-100.
-
Reverse Cholesterol Transport
- HDL (“good cholesterol”) is secreted by the liver and intestine (containing ApoA-I).
- It picks up excess cholesterol from peripheral tissues.
- LCAT (activated by ApoA-I) esterifies the cholesterol, trapping it in the HDL core.
- HDL returns the cholesterol to the liver for excretion in bile.
Common steps for exo and endo pathways: bind to HDL, deliver TG to adipocytes, bind to ApoE receptor and cleared by hepatic lipase
Tip
Late-onset familial Alzheimer disease is associated with the ε4 allele of Apolipoprotein E.