| Degree | Names | Layers Involved | Clinical Appearance | Sensation | Healing / Scarring |
|---|---|---|---|---|---|
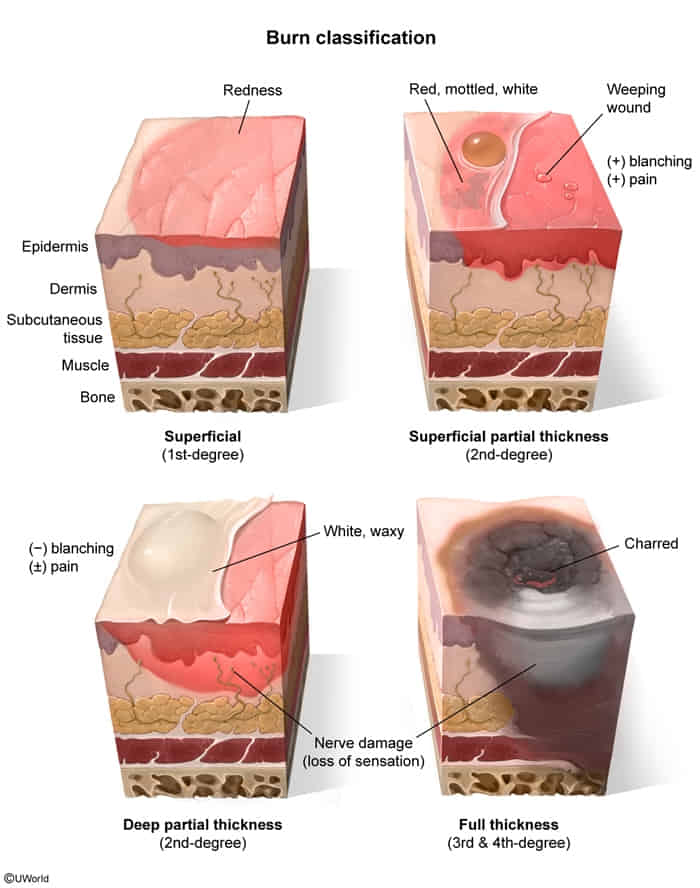
| 1st | Superficial | Epidermis only | Dry, red, blanches with pressure, no blisters | Painful & tender | Heals within 3-6 days; no scarring |
| 2nd | Superficial Partial-Thickness | Epidermis + Papillary Dermis | Blisters (often intact), moist, red, weepy; blanches well | Very painful, sensitive to air | Heals in 7-21 days; minimal to no scarring |
| 2nd | Deep Partial-Thickness | Epidermis + Reticular Dermis | Blisters (easily unroofed), mottled pink/white, sometimes waxy or dry | Painful but may have decreased sensation | Heals in >21 days; significant scarring, may need skin graft |
| 3rd | Full-Thickness | Epidermis + Dermis + Subcutaneous fat | Waxy white, leathery, charred, or black; does not blanch | Painless and insensate due to nerve destruction | Requires excision and skin grafting; severe scarring |
| 4th | Full-Thickness | Extends into fascia, muscle, and/or bone | Charred, black, or white with exposed deep tissues (muscle, bone) | Painless, insensate | Requires extensive surgical intervention, possibly amputation |
Burn Surface Area and Fluid Replacement
1. Estimating Total Body Surface Area (TBSA) Burned
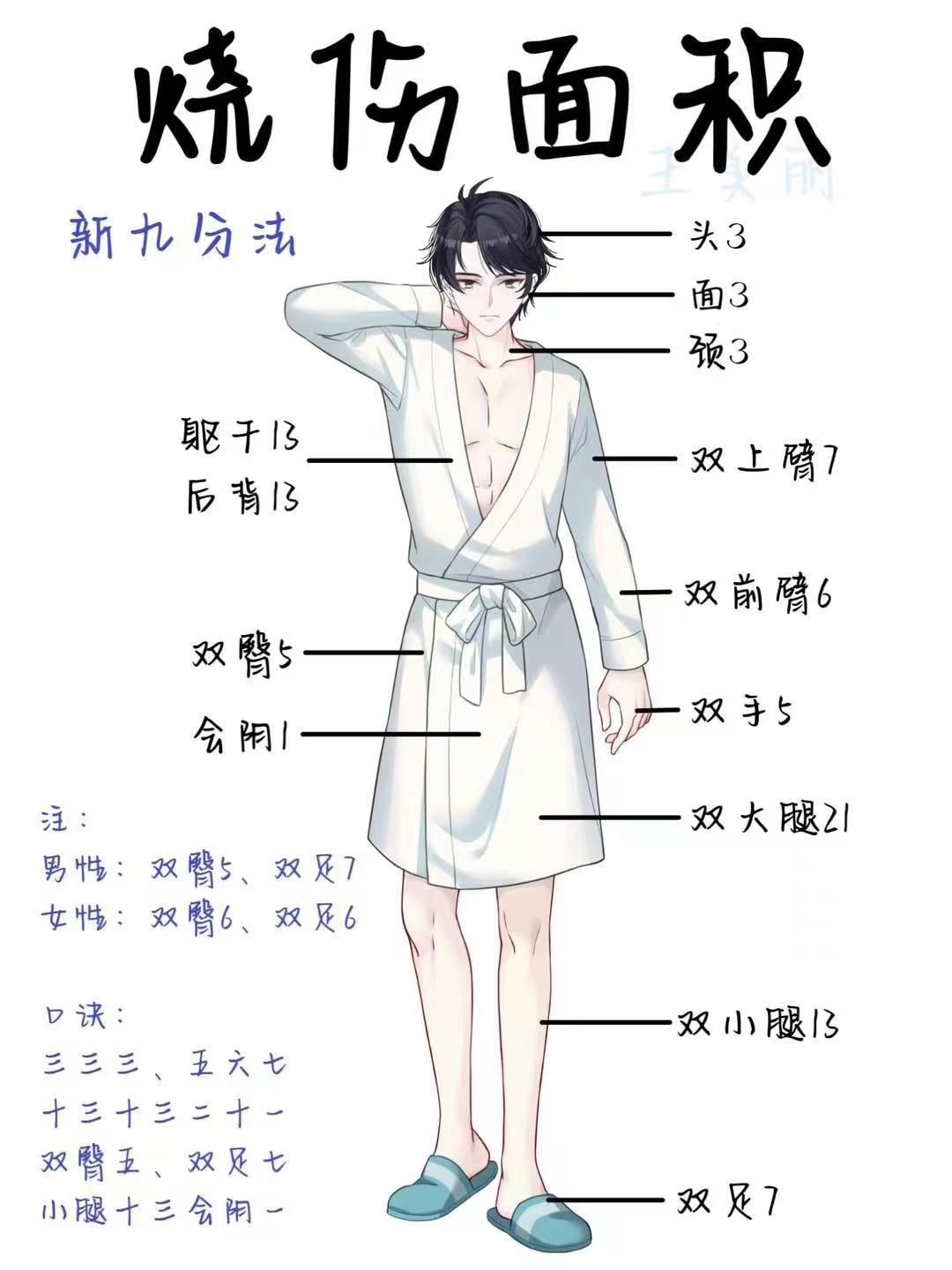
- Rule of Nines (Adults): A quick method to estimate TBSA for partial and full-thickness burns.
- Head & Neck: 9%
- Each Arm: 9%
- Anterior Torso: 18%
- Posterior Torso: 18%
- Each Leg: 18%
- Genitalia/Perineum: 1%
- Rule of Nines (Pediatric): Modified due to different body proportions (larger head, smaller legs).
- Head & Neck: 18%
- Each Arm: 9%
- Anterior Torso: 18%
- Posterior Torso: 18%
- Each Leg: 14%
- Lund-Browder Chart: More accurate, especially for children, as it adjusts for age.
- Palmar Method: The surface area of the patient’s palm (including fingers) is roughly 1% of their TBSA, useful for smaller, patchy burns.
Important Note: Only partial-thickness (2nd degree) and full-thickness (3rd degree) burns are included in the TBSA calculation for fluid resuscitation. Superficial (1st degree) burns like simple erythema are excluded.
2. Fluid Resuscitation
Intravenous fluid resuscitation is crucial for patients with significant burns to prevent burn shock.
- Indications: Generally required for burns >20% TBSA in adults and >10-15% TBSA in children.
- American Burn Association (ABA) / Consensus Formula (Current Recommendation): This is recommended over the traditional Parkland formula to reduce “fluid creep” and associated complications (e.g., pulmonary edema, compartment syndrome). The starting rate is based on the injury type:
- Flame, Chemical, or Scald Injury:
- Adults & Children ≥ 14 years: 2 mL x kg x %TBSA.
- Children < 14 years: 3 mL x kg x %TBSA.
- Electrical Injury:
- All ages: 4 mL x kg x %TBSA. This higher volume is used due to the extensive deep tissue injury that is often not visible on the surface.
- Flame, Chemical, or Scald Injury:
- Fluid Administration Schedule:
- First 8 hours: Give the first half of the total calculated volume.
- Next 16 hours: Give the second half of the total volume.
- Key Point: The “first 8 hours” starts from the time of the burn injury, not from the time of hospital arrival.
- Choice of Fluid:
- Lactated Ringer’s (LR) is the preferred crystalloid solution due to its physiologic composition.
- Normal saline can also be used.
3. Monitoring and Titration
The Parkland formula is an initial estimate. Fluid rates must be titrated based on the patient’s response.
- Primary Indicator: Urine output (UOP) is the most reliable indicator of adequate resuscitation. An indwelling urinary catheter is essential for accurate monitoring.
- Target UOP:
- Adults: 0.5 - 1.0 mL/kg/hr (commonly 30-50 mL/hr).
- Children (<30 kg): 1.0 mL/kg/hr.
- Other Monitoring Parameters:
- Mental status, heart rate, blood pressure, and palpable peripheral pulses are also important indicators of adequate perfusion.
- Special Considerations:
- Pediatric Patients: In addition to resuscitation fluids, children also require maintenance fluids, often containing dextrose.
- Inhalational Injury: Patients with inhalation injury often have significantly increased fluid requirements.
- Electrical Burns: High-voltage electrical burns can cause extensive deep tissue damage not apparent on the surface, leading to higher fluid needs.