Mucormycosis
-
Patho/Etiology
- Caused by fungi of the order Mucorales (e.g., Rhizopus, Mucor).
- Spores are inhaled and germinate in the upper airways or are inoculated through skin trauma.
- Angioinvasion is the hallmark: hyphae invade blood vessels, causing thrombosis, ischemia, and extensive tissue necrosis.
- Fungi thrive in high glucose and acidic environments.
-
Key Associations (Risk Factors)
- Diabetic ketoacidosis (DKA) is the most classic association.
- Immunocompromised states: hematologic malignancies (leukemia, lymphoma), neutropenia, organ/stem cell transplant.
- Long-term corticosteroid use.
- Iron overload (e.g., hemochromatosis) and treatment with deferoxamine.
- Severe trauma or burns.
-
Clinical Presentation
- Presentation depends on the site of infection. Forms include rhinocerebral, pulmonary, cutaneous, GI, and disseminated.
- Rhinocerebral (most common): Starts like acute sinusitis with facial pain, headache, and nasal congestion. Progresses rapidly to cause:
- Black necrotic eschar on the nasal turbinates or hard palate.
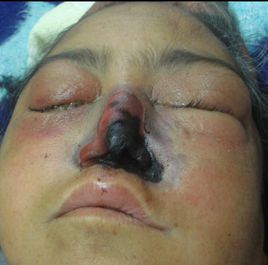
- Periorbital swelling, proptosis, diplopia, and vision loss due to orbital invasion.
- Cranial nerve palsies.
- Altered mental status if it extends into the brain via the cribriform plate.
- Black necrotic eschar on the nasal turbinates or hard palate.
- Pulmonary: Fever, cough, dyspnea, hemoptysis; often seen in neutropenic patients.
- Cutaneous: Erythematous lesion progressing to a necrotic ulcer with a central black eschar, often at a site of trauma.
-
Diagnosis
- Urgent tissue biopsy is the gold standard for diagnosis.
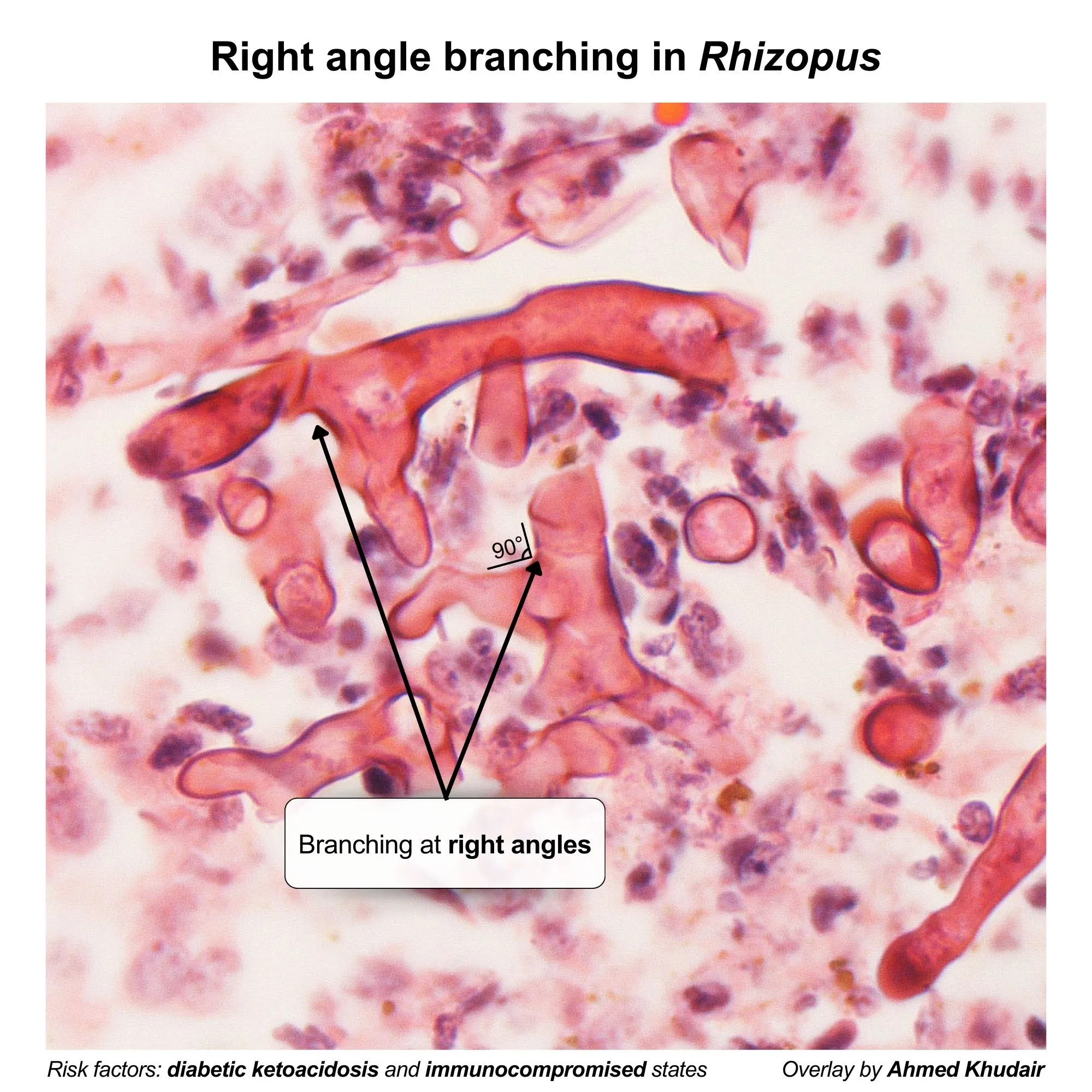
- Histopathology: Shows broad, nonseptate (or pauciseptate) hyphae with wide-angle (90° or right-angle) branching.
- Imaging (CT/MRI): Used to assess the extent of sinus, orbital, and intracranial involvement. Findings include mucosal thickening and bony erosion.
- Culture is often negative and should not delay treatment.
-
DDx (Differential Diagnosis)
- Rhinocerebral: Invasive aspergillosis (has septate hyphae with acute-angle branching), bacterial sinusitis (less rapid, no eschar), cavernous sinus thrombosis.
- Pulmonary: Invasive aspergillosis, lung abscess, malignancy.
- Cutaneous: Ecthyma gangrenosum (caused by Pseudomonas aeruginosa), necrotizing fasciitis.
-
Management/Treatment
- A true medical and surgical emergency.
- 1. Surgical Debridement: Aggressive and immediate removal of all necrotic tissue is crucial.
- 2. Antifungal Therapy:
- First-line: Liposomal Amphotericin B (IV).
- Alternatives/Step-down: Posaconazole or Isavuconazole.
- 3. Reverse Underlying Condition: Control hyperglycemia and acidosis in DKA, reduce immunosuppressants if possible.
-
Complications
- Cavernous sinus thrombosis, carotid artery thrombosis.
- Brain abscess, massive tissue destruction, blindness.
- Disseminated disease and death. The overall mortality rate is very high (~50%).